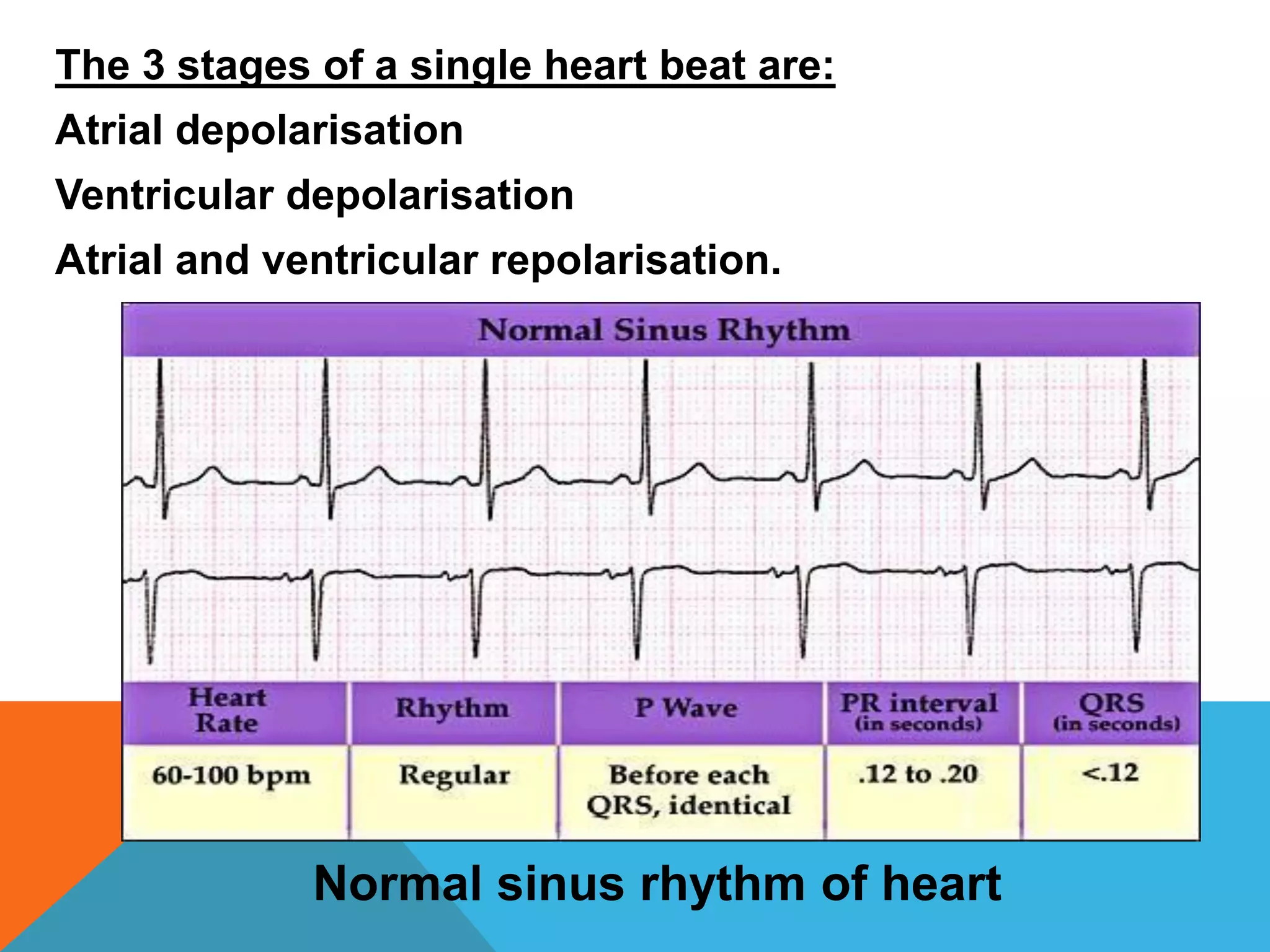
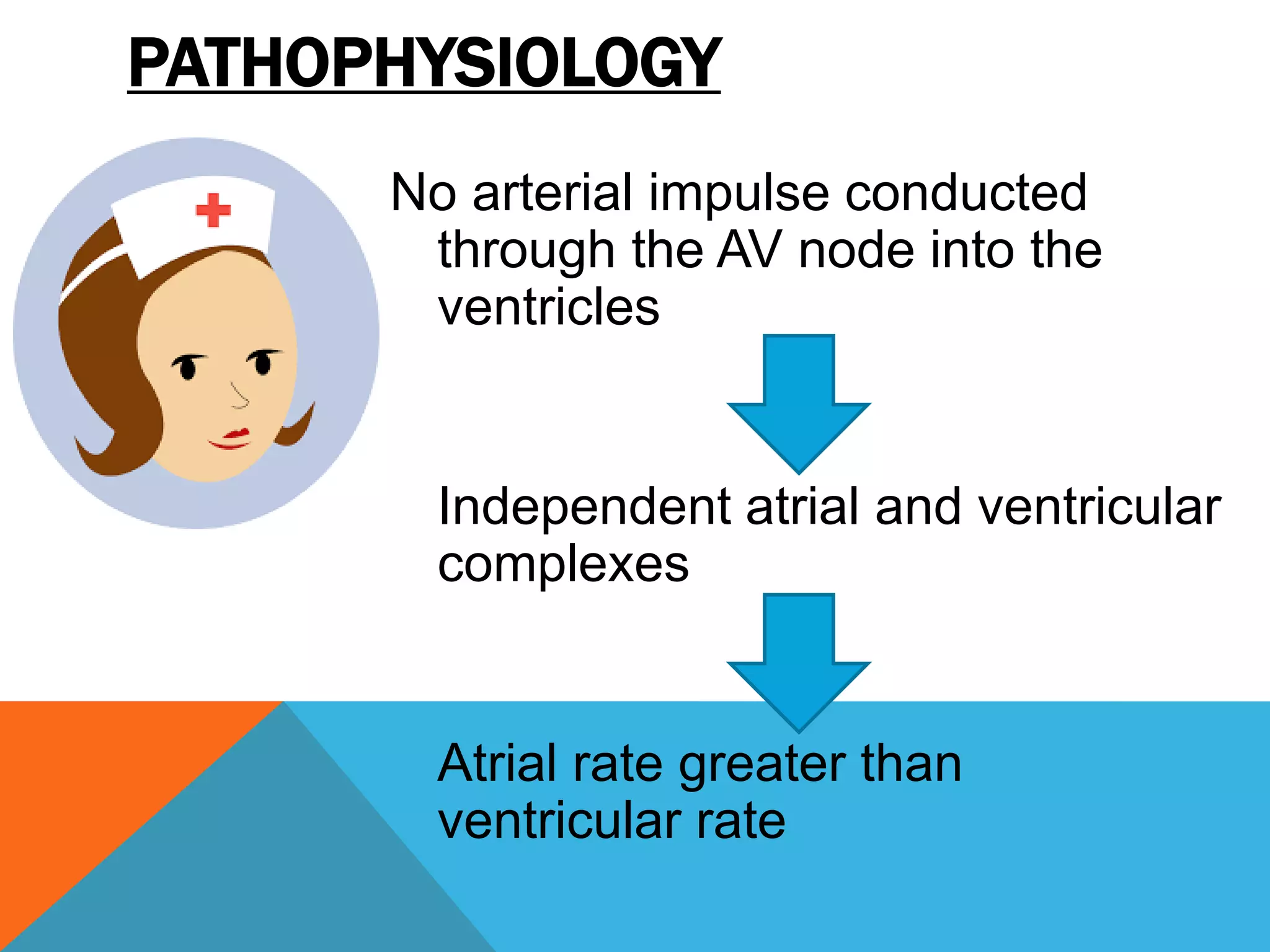
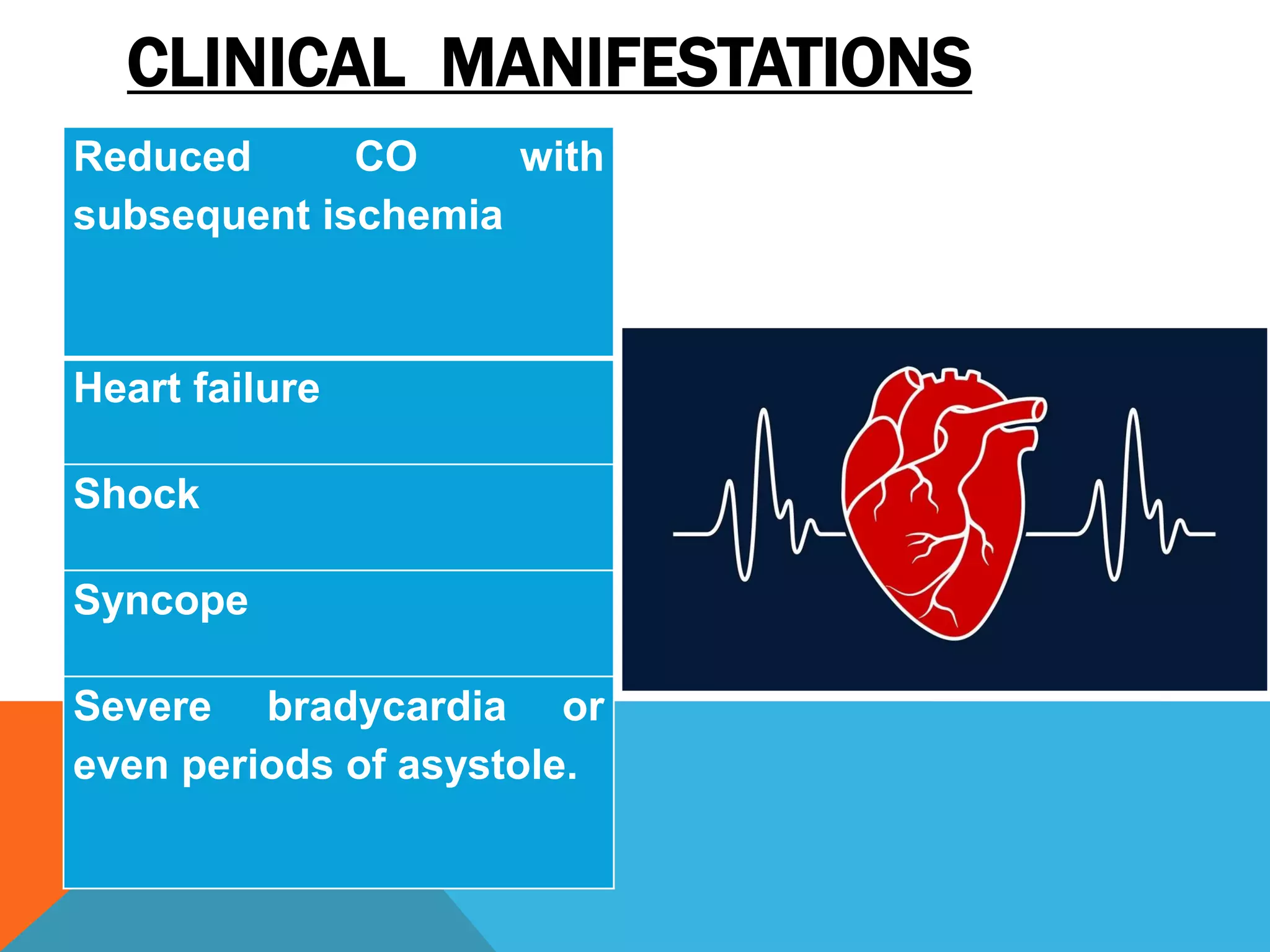
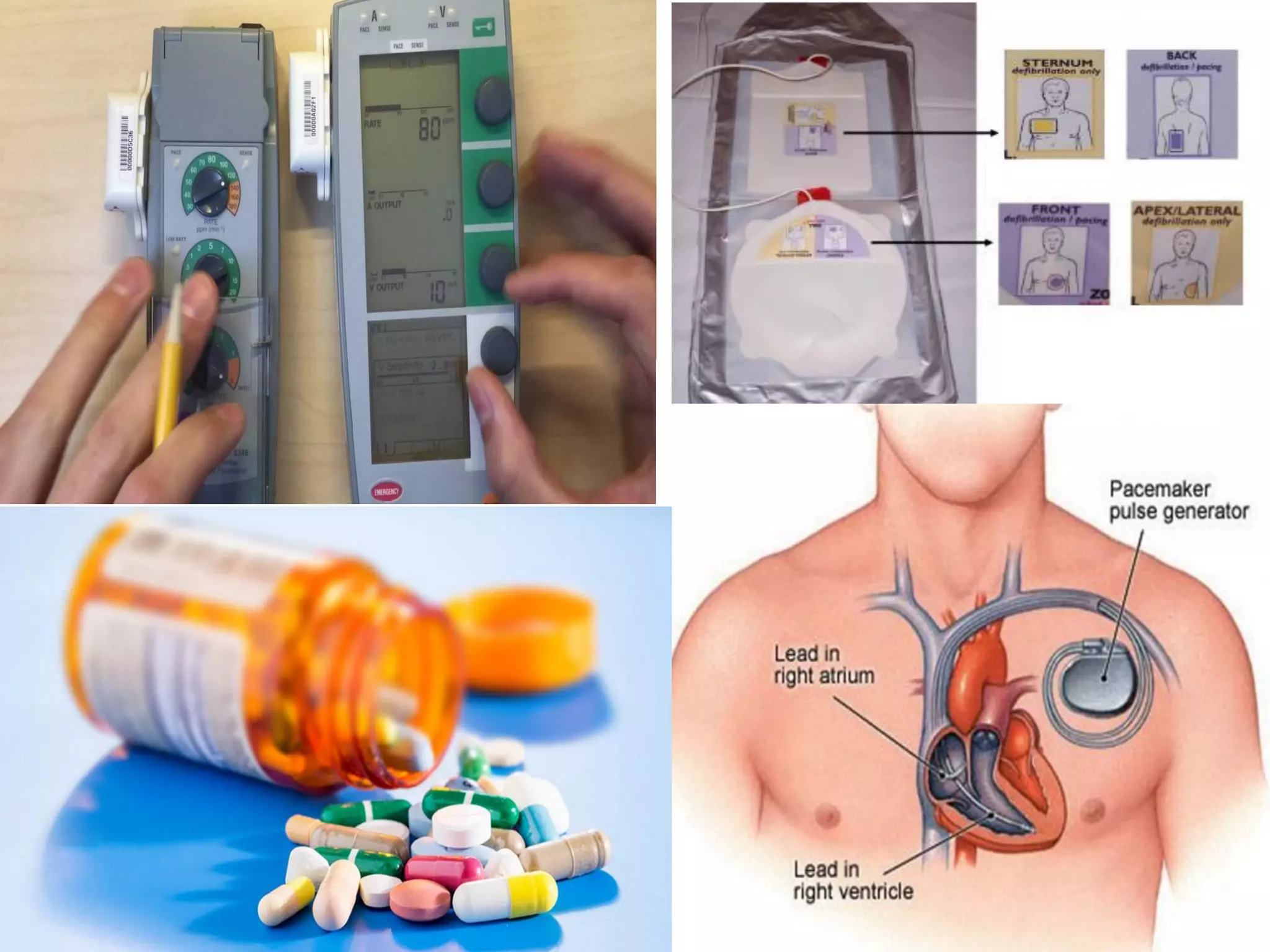
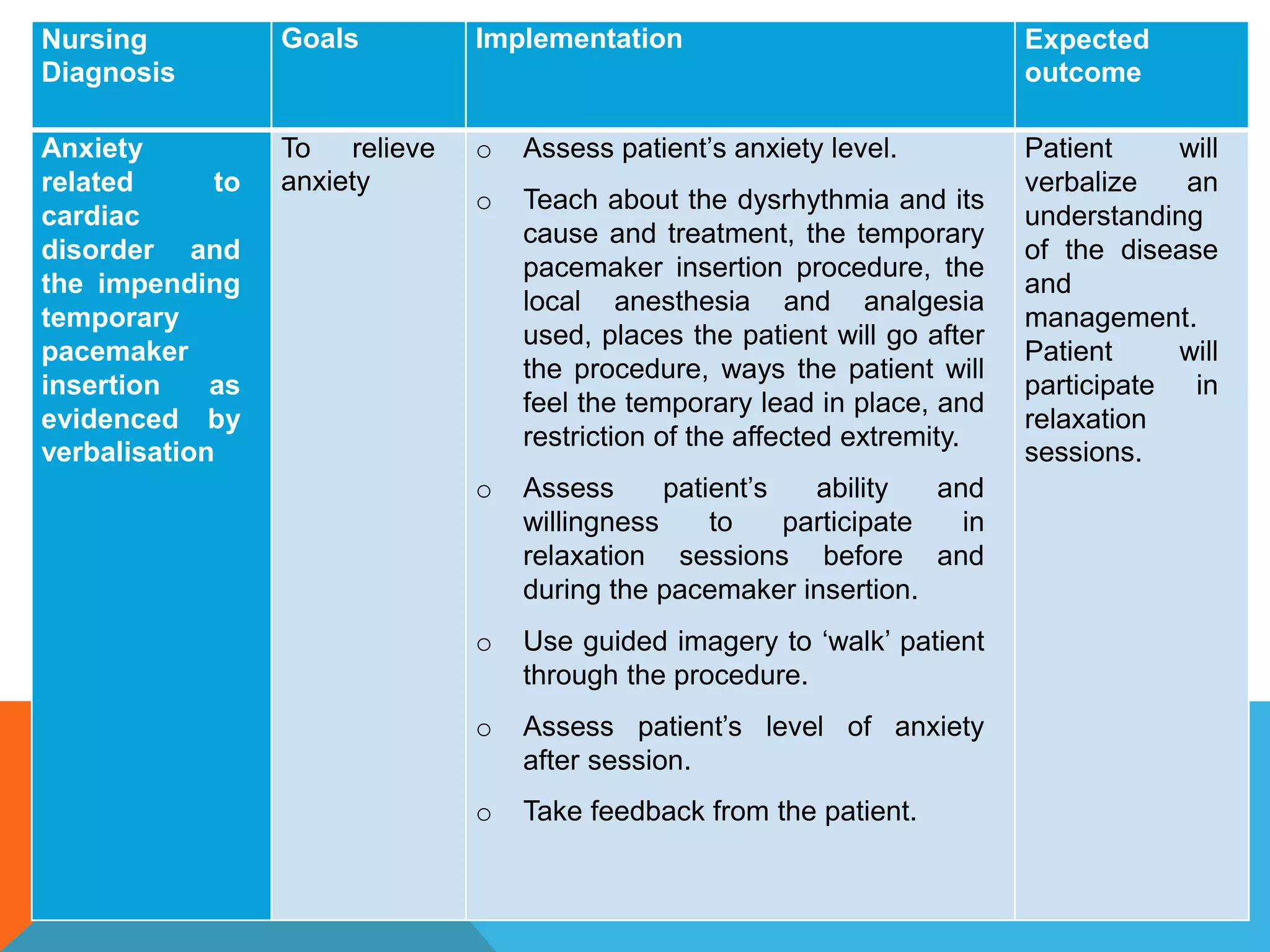
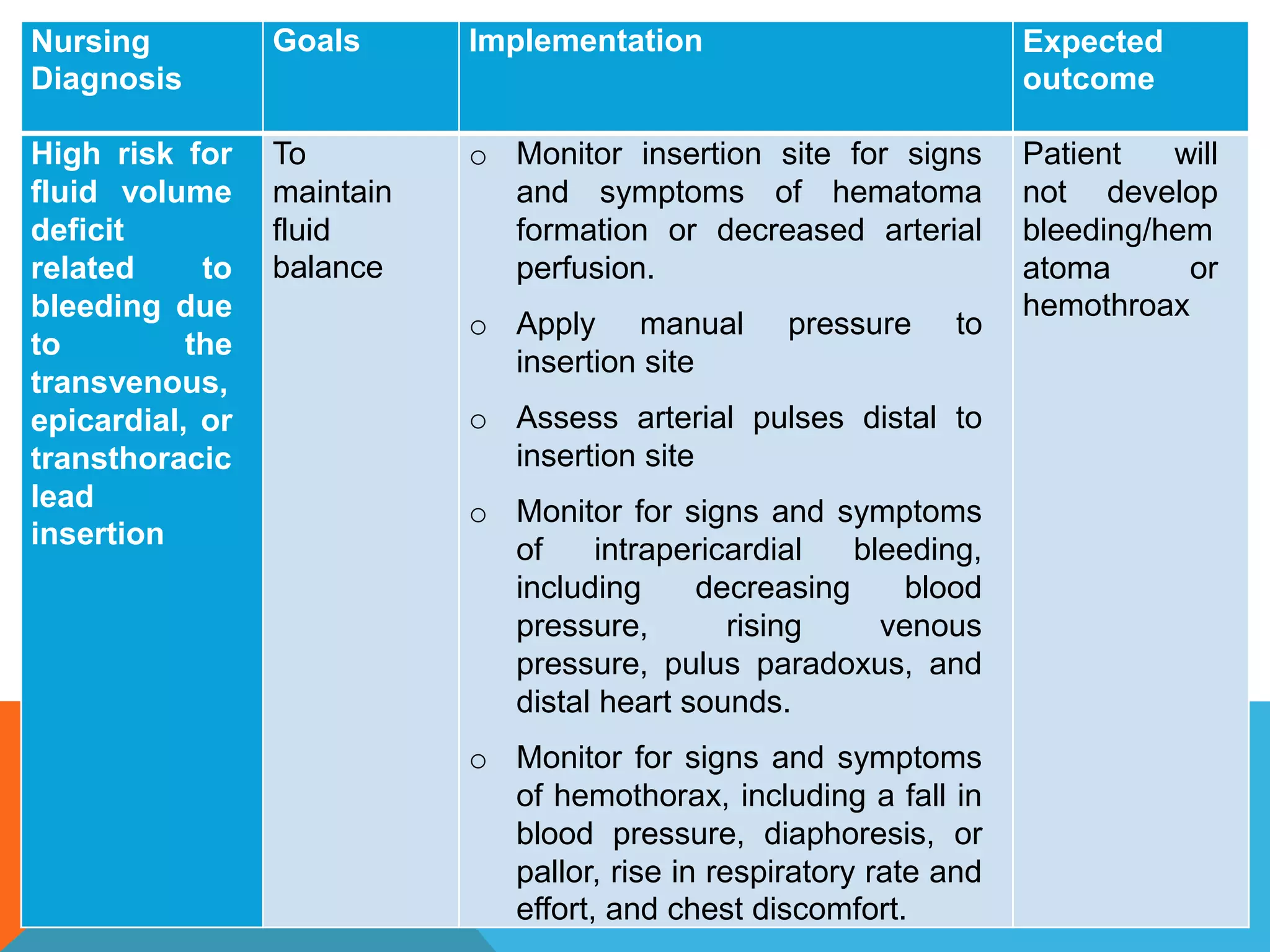
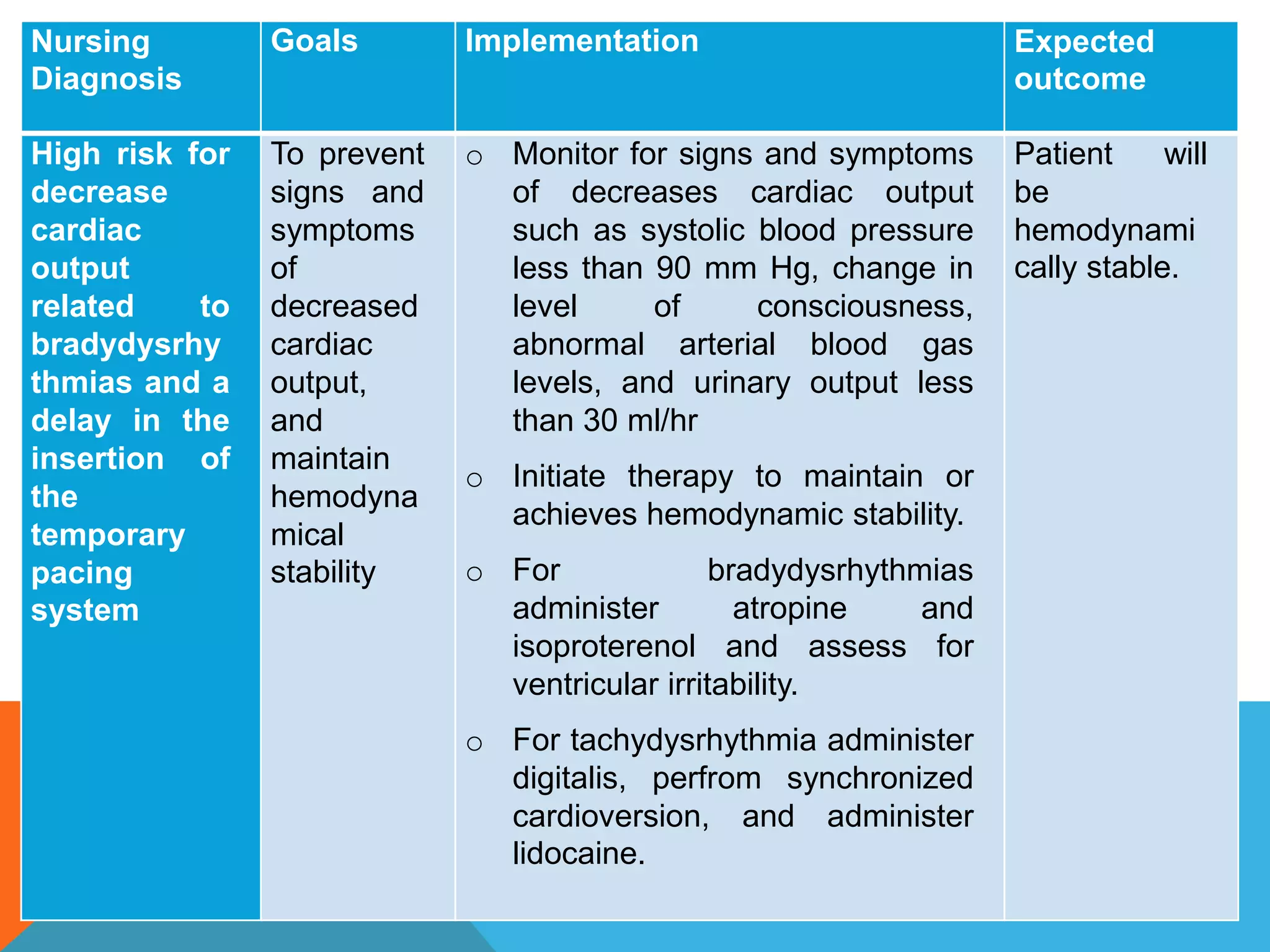
Heart block is a disturbance in the heart's electrical conduction system that can be classified into first-degree, second-degree (types I and II), and third-degree blocks. First-degree block has prolonged conduction without missed beats, while second-degree type I presents with progressively lengthening PR intervals before a block, and type II shows non-conducted beats without lengthening, frequently requiring pacing. Third-degree block leads to complete dissociation between atrial and ventricular impulses, necessitating urgent pacemaker intervention to prevent severe complications like heart failure and syncope.