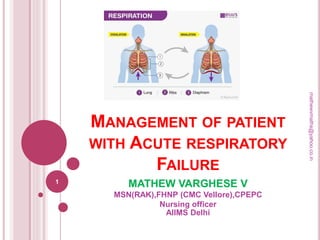
Acute Respiratory failure
- 1. MANAGEMENT OF PATIENT WITH ACUTE RESPIRATORY FAILURE MATHEW VARGHESE V MSN(RAK),FHNP (CMC Vellore),CPEPC Nursing officer AIIMS Delhi mathewvmaths@yahoo.co.in 1
- 2. INTRODUCTION Respiratory failure is a sudden and life-threatening deterioration of the gas exchange function of the lung. It exists when the exchange of oxygen for carbon dioxide in the lungs cannot keep up with the rate of oxygen consumption and carbon dioxide production by the cells of the body. Respiratory failure is a condition in which your blood doesn't have enough oxygen or has too much carbon dioxide. Sometimes you can have both problems. mathewvmaths@yahoo.co.in 2
- 4. DEFINITION OF RESPIRATORY FAILURE Respiratory failure is a syndrome of inadequate gas exchange due to dysfunction of one or more essential components of the respiratory system: Such as Chest wall (including pleura and diaphragm) Airways Alveolar – capillary units Pulmonary circulation Nerves CNS or Brain Stem mathewvmaths@yahoo.co.in 4
- 6. EPIDEMIOLOGY OF RESPIRATORY FAILURE Incidence: about 360,000 cases per year in the United States 36% die during hospitalization Morbidity and mortality rates increase with age and presence of co morbidities It is the main cause of death from pneumonia and chronic obstructive pulmonary disease (COPD), which together comprise the third-leading cause of death in the United States today. mathewvmaths@yahoo.co.in 6
- 7. TYPES OF RESPIRATORY FAILURE Respiratory Failure Acute Chronic mathewvmaths@yahoo.co.in 7
- 8. ACUTE RESPIRATORY FAILURE Acute respiratory failure (ARF) is defined as a fall in arterial oxygen tension (PaO2) to less than 50 mm Hg (hypoxemia) and a rise in arterial carbon dioxide tension (PaCO2) to greater than 50 mm Hg (hypercapnia), with an arterial pH of less than 7.35. mathewvmaths@yahoo.co.in 8
- 9. ARF Respiratory system mechanisms leading to ARF include: Alveolar hypoventilation Diffusion abnormalities Ventilation–perfusion mismatching Shunting mathewvmaths@yahoo.co.in 9
- 10. CHRONIC RESPIRATORY FAILURE Chronic respiratory failure is defined as deterioration in the gas exchange function of the lung that has developed insidiously or has persisted for a long period after an episode of ARF. The absence of acute symptoms and the presence of a chronic respiratory acidosis suggest the chronicity of the respiratory failure. mathewvmaths@yahoo.co.in 10
- 11. CAUSES OF CHRONIC RESPIRATORY FAILURE Two causes of chronic respiratory failure are COPD and neuromuscular diseases. Patients with these disorders develop a tolerance to the gradually worsening hypoxemia and hypercapnia. However, a patient with chronic respiratory failure may develop ARF. This is seen in the COPD patient who develops an exacerbation or infection that causes additional deterioration of the gas exchange mechanism. mathewvmaths@yahoo.co.in 11
- 12. TYPES OF ACUTE RESPIRATORY FAILURE Type I or Hypoxemic respiratory failure Type II or Hypercapnic respiratory failure Type III Respiratory Failure: Perioperative Respiratory Failure Type IV Respiratory Failure: Shock mathewvmaths@yahoo.co.in 12
- 13. TYPE I OR HYPOXEMIC RESPIRATORY FAILURE It means that a person is not exchanging oxygen properly in their lungs. This may be due to swelling or damage to the lungs. A person with type 1 acute respiratory failure has very low oxygen levels. PaO2<60 mm of Hg Failure of oxygen exchange mathewvmaths@yahoo.co.in 13
- 14. DEFINITION Type 1 respiratory failure is defined as a low level of oxygen in the blood (hypoxemia) with either a normal (normocapnia) or low (hypocapnia) level of carbon dioxide (PaCO2) but not an increased level (hypercapnia). It is typically caused by a ventilation/perfusion (V/Q) mismatch; the volume of air flowing in and out of the lungs is not matched with the flow of blood to the lungs. mathewvmaths@yahoo.co.in 14
- 15. CAUSES OF TYPE 1 ARF ARF • Low ambient oxygen • Ventilation-perfusion mismatch ARF • Alveolar hypoventilation • Diffusion problem ARF • Shunt mathewvmaths@yahoo.co.in 15
- 16. TYPE II OR HYPERCAPNIC RESPIRATORY FAILURE : (PACO2> 45 MM OF HG): FAILURE TO EXCHANGE OR REMOVE CARBON DIOXIDE In type II ARF ,the lungs are not removing enough carbon dioxide The lungs usually exchange carbon dioxide for fresh oxygen. This type of respiratory failure causes carbon dioxide levels to be high. It may result from a drug overdose that has caused a person to breathe too slowly or because of lung damage from smoking, which causes COPD. mathewvmaths@yahoo.co.in 16
- 17. CAUSES OF TYPE II Increased airways resistance Reduced breathing effort A decrease in the area of the lung available for gas exchange Neuromuscular problems Deformed (kyphoscoliosis), rigid (ankylosing spondylitis), or flail chest mathewvmaths@yahoo.co.in 17
- 18. TYPE III RESPIRATORY FAILURE: PERIOPERATIVE RESPIRATORY FAILURE It occurs when a person has had surgery, and the small airways in the lungs have closed in greater numbers. Factors such as pain or stomach surgery, which places higher pressure on the lungs, can also contribute to this type of respiratory failure. mathewvmaths@yahoo.co.in 18
- 19. TYPE IV RESPIRATORY FAILURE: SHOCK Type 4 respiratory failure is a shock state. It means that the body cannot adequately provide oxygen and maintain blood pressure on its own. This can result from serious illness or injury, such as when a person loses too much blood mathewvmaths@yahoo.co.in 19
- 20. PRECIPITATING CONDITIONS LEADING TO ACUTE RESPIRATORY FAILURE Acute exacerbation of asthma Pulmonary embolism Pulmonary edema Acute respiratory distress syndrome Pneumonia Acute epiglottitis Cardiogenic pulmonary edema Pulmonary trauma Inhalation injury Upper/lower airway obstruction Pneumothorax Chronic lung disease Bronchiectasis Alveolar abnormalities Chest wall abnormalities (e.g., kyphoscoliosis) Malignancy Decompensate congestive cardiac failure Collagen vascular disease. mathewvmaths@yahoo.co.in 20
- 21. CLASSIFICATION OF CAUSES Decreased respiratory drive Dysfunction of the chest wall Dysfunction of the lung parenchyma Other causes mathewvmaths@yahoo.co.in 21
- 22. CLINICAL MANIFESTATIONS EARLY SIGNS Restlessness Fatigue Headache Dyspnea Air hunger Tachycardia Increased blood pressure. mathewvmaths@yahoo.co.in 22
- 23. LATE SIGNS Confusion Lethargy Tachycardia Tachypnea Central cyanosis Diaphoresis Finally respiratory arrest mathewvmaths@yahoo.co.in 23
- 24. PATHOPHYSIOLOGY OF ACUTE RESPIRATORY FAILURE – TYPE I Ventilation/ Perfusion (V/Q) mismatch Pulmonary Shunt Other mechanisms Alveolar unit failure Pulmonary vasculature failure mathewvmaths@yahoo.co.in 24
- 25. TYPE II FAILURE (HYPERCAPNIC FAILURE) PATHOPHYSIOLOGIC MECHANISMS Decreased minute ventilation (MV) relative to demand Increased dead space ventilation Nervous system failure Chest wall and pleural space failure Airway failure Neuromuscular transmission failure Muscle (pump) failure mathewvmaths@yahoo.co.in 25
- 26. DIAGNOSIS History Physical Examination Findings Lab investigations • ABG • Complete blood count • Cardiac serologic markers • Microbiology Chest X Ray Electrocardiogram Echocardiography Pulmonary function tests/bedside spirometry Bronchoscopy mathewvmaths@yahoo.co.in 26
- 29. MANAGEMENT MEASURES ABC’s Ensure airway is adequate Ensure adequate supplemental oxygen and assisted ventilation, if indicated Support circulation as needed Treatment of a specific cause when possible Infection management Antimicrobials Source control mathewvmaths@yahoo.co.in 29
- 30. MANAGEMENT MEASURES Airway obstruction Bronchodilators Glucocorticoids Improve cardiac function Positive airway pressure Diuretics, Vasodilators Morphine Ionotrops Revascularization mathewvmaths@yahoo.co.in 30
- 31. MANAGEMENT MEASURES Mechanical ventilation Non - invasive (if patient can protect airway and is hemodynamically stable) Mask: usually orofacial to start Invasive Endotracheal tube (ETT) Tracheostomy – if upper airway is obstructed mathewvmaths@yahoo.co.in 31
- 32. INDICATIONS FOR MECHANICAL VENTILATION Cardiac or respiratory arrest Tachypnea or bradypnea with respiratory fatigue or impending arrest Acute respiratory acidosis Refractory hypoxemia (when the P a O 2 could not be maintained above 60 mm Hg with inspired O 2 fraction (F I O 2 )>1.0) Inability to protect the airway associated with depressed levels of consciousness Shock associated with excessive respiratory work Inability to clear secretions with impaired gas exchange or excessive respiratory work Newly diagnosed neuromuscular disease with a vital capacity <10-15ml/kg Short term adjunct in management of acutely increased intracranial pressure (ICP) mathewvmaths@yahoo.co.in 32
- 33. NON - INVASIVE VENTILATION INDICATION COPD exacerbation Cardiogenic pulmonary edema Obesity hypoventilation syndrome Noninvasive ventilation may be tried in selected patients with asthma or non patients with asthma or non - cardiogenic hypoxemic respiratory failure respiratory failure mathewvmaths@yahoo.co.in 33
- 34. Goals of Mechanical Ventilation Improve ventilation by augmenting respiratory rate and tidal volume Assistance for neural or muscle dysfunction Sedated, comatose or paralyzed patient Neuropathy, myopathy or muscular dystrophy Intra - operative ventilation Correct respiratory acidosis, providing goals of lung - protective ventilation are met Match metabolic demand Rest respiratory muscles mathewvmaths@yahoo.co.in 34
- 35. NURSING DIAGNOSIS AND INTERVENTIONS Nursing Diagnosis: Impaired gas exchange related to ventilation–perfusion inequality Goal: Improvement in gas exchange Nursing Diagnosis: Ineffective airway clearance related to bronchoconstriction, increased mucus production, ineffective cough, bronchopulmonary infection, and other complications Goal: Achievement of airway clearance mathewvmaths@yahoo.co.in 35
- 36. NURSING DIAGNOSIS AND INTERVENTIONS Nursing Diagnosis: Ineffective breathing pattern related to shortness of breath, mucus, bronchoconstriction, and airway irritants Goal: Improvement in breathing pattern Nursing Diagnosis: Self-care deficits related to fatigue secondary to increased work of breathing and insufficient ventilation and oxygenation Goal: Independence in self-care activities mathewvmaths@yahoo.co.in 36
- 37. NURSING DIAGNOSIS AND INTERVENTIONS Nursing Diagnosis: Activity intolerance due to fatigue, hypoxemia, and ineffective breathing patterns Goal: Improvement in activity tolerance Nursing Diagnosis: Ineffective coping related to reduced socialization, anxiety, depression, lower activity level and the inability to work Goal: Attainment of an optimal level of coping Nursing Diagnosis: Deficient knowledge about self- management to be performed at home. Goal: Adherence to therapeutic program and home care mathewvmaths@yahoo.co.in 37
- 38. RESEARCH STUDIES Title :Patients’ Outcomes After Acute Respiratory Failure: A Qualitative Study With the PROMIS Framework Author :Michelle N. Eakin, PhD,Yashika Patel, BA, BS ; Pedro Mendez-Tellez, MD Am J Crit Care (2017) 26 (6): 456–465. https://doi.org/10.4037/ajcc2017834 mathewvmaths@yahoo.co.in 38
- 39. RESEARCH STUDY Objective To describe the survivorship experience of patients who had acute respiratory failure by using the Patient Reported Outcomes Measurement Information System (PROMIS) framework. Methods A total of 48 adult patients who had acute respiratory failure completed at least 1 semistructured telephone- based interview between 5 and 18 months after their stay in the intensive care unit. Participants were asked about overall well-being and important health outcomes. mathewvmaths@yahoo.co.in 39
- 40. RESULTS Major themes were identified within each of the 3 PROMIS components: physical health, mental health, and social health. The following themes were particularly prominent: mobility impairments, pulmonary symptoms, fatigue, anxiety and depression symptoms, and decreased ability to work and participate in valued activities. Impacts on overall well-being and on relationships with friends and family members varied among the survivors. Some survivors reported gratitude, increased appreciation of life, and closer relationships to loved ones. Other survivors reported boredom, social isolation, and wishing they had not survived. mathewvmaths@yahoo.co.in 40
- 41. CONCLUSIONS Survivors of acute respiratory failure reported substantial issues with their physical, mental, and social health. Holistic assessments of outcomes of survivors of critical illness should capture the complex beneficial and adverse impacts of critical illness on survivors’ well-being and social health. mathewvmaths@yahoo.co.in 41
- 42. REFERENCES Midelton G.T., Frishman W.H., Passo S.S. (2002). Congestive heart failure and continuous positive airway pressure therapy: support of a new mo continuous positive airway pressure therapy: support of a new mo dality for improving the prognosis and survival of patients with advanced congestive heart failure. heart failure. Heart Disease, Volume 4 Disease, Volume 4 , Number 2, p 102 Number 2, p 102 - 109 . Arora ,V.K., Shankar Shankar , U. (1995). Acute Lung Injury. , U. (1995). Acute Lung Injury. Lung India, Volume Lung India, Volume XIII, Number 1, p 32 1, p 32 - 34. Behrendt C.F. (2000). Acute respiratory failure in the United States: Inc C.F. (2000). Acute respiratory failure in the United States: Inc idence and 31 - day survival. day survival. Chest, Volume 118, Number 4, p 1100 Chest, Volume 118, Number 4, p 1100 - 1105. mathewvmaths@yahoo.co.in 42
