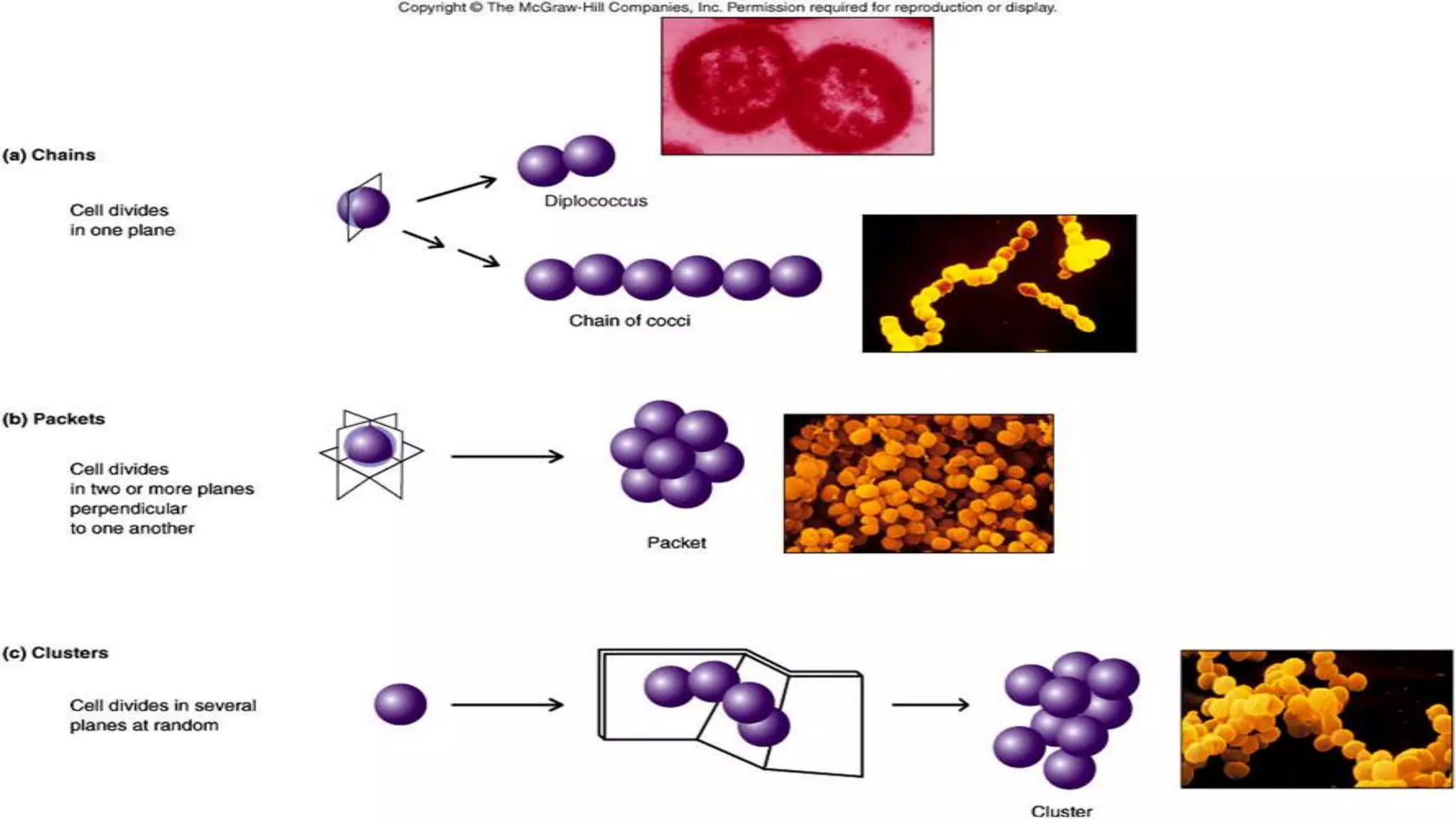
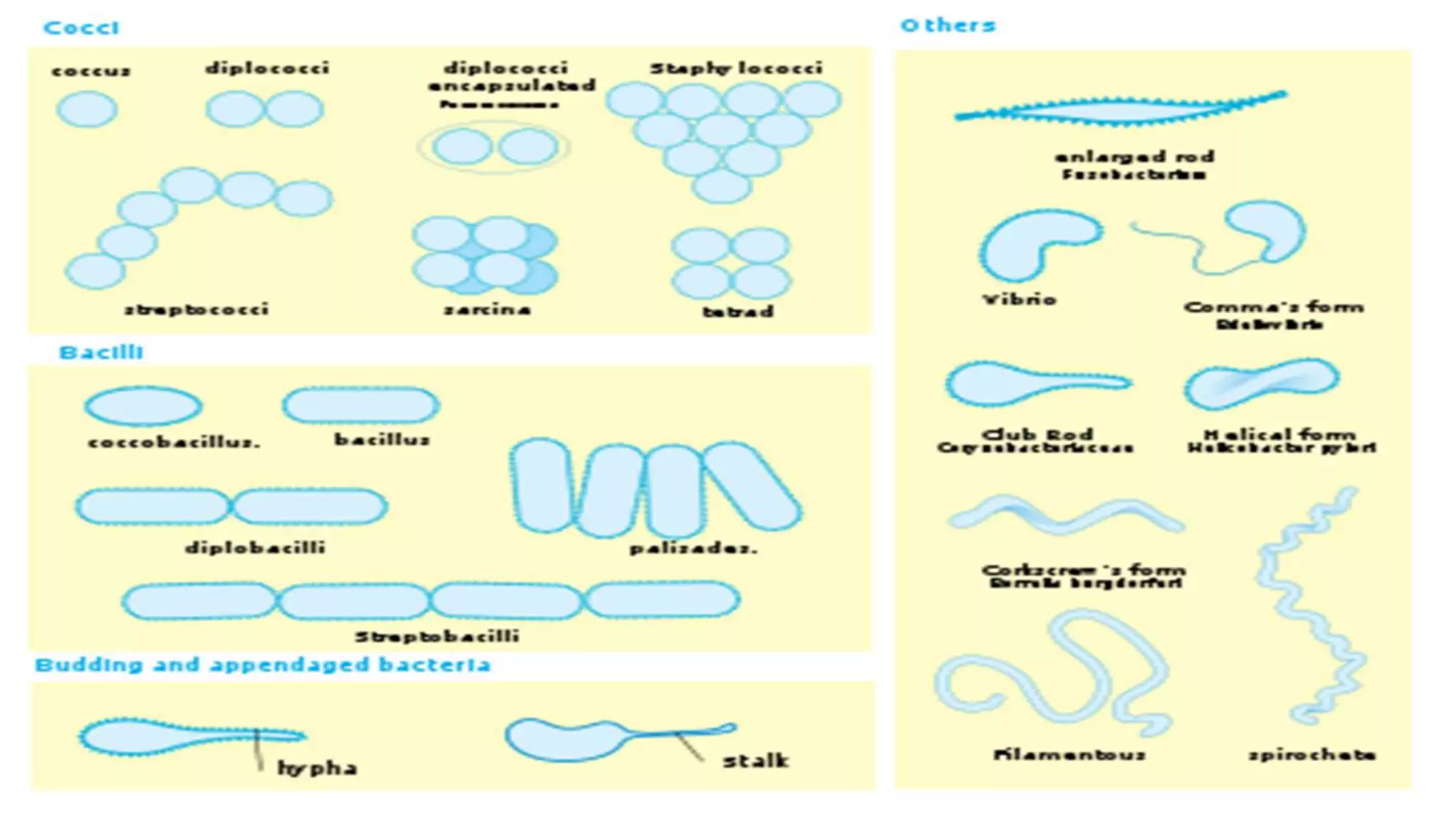
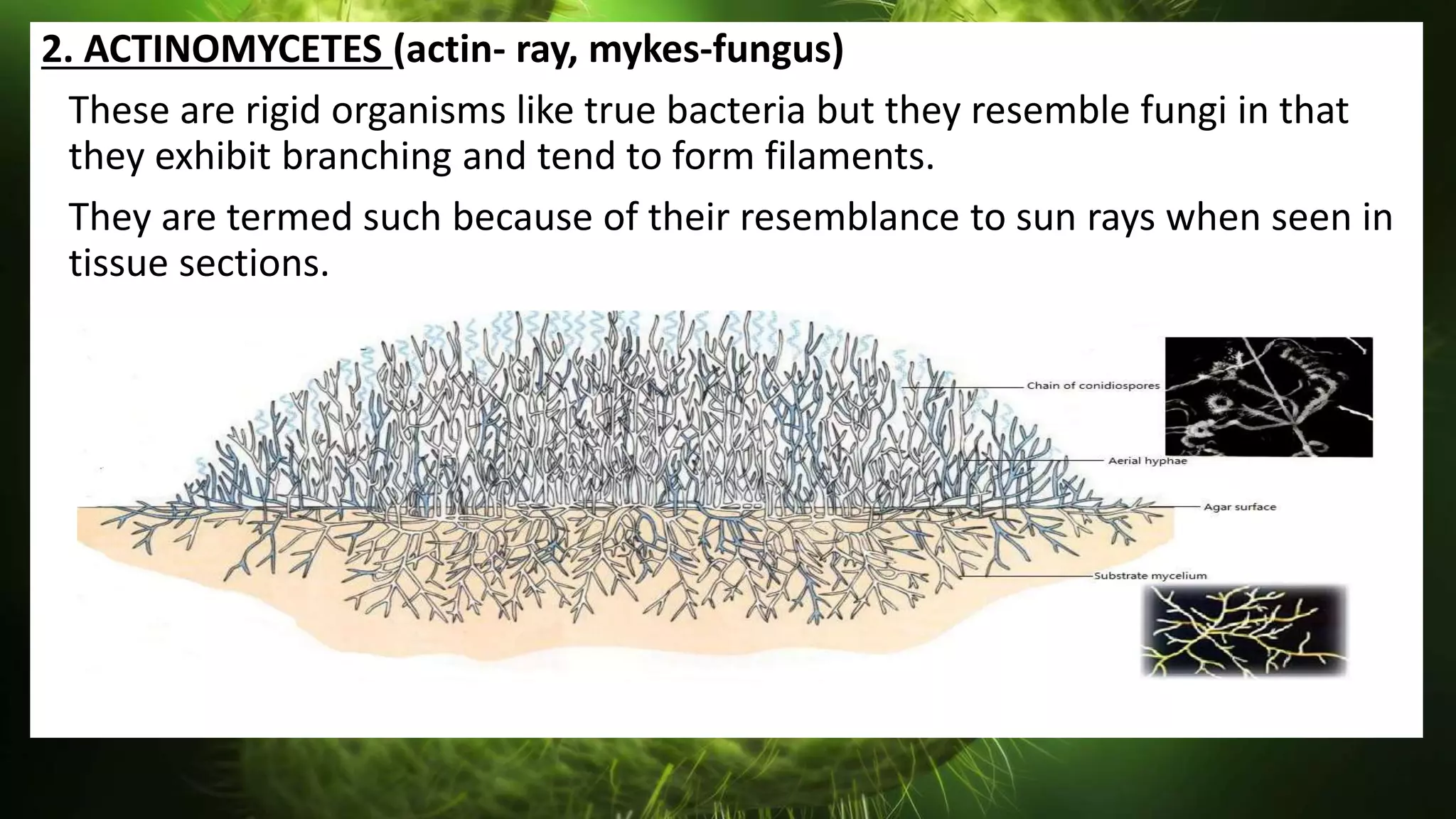
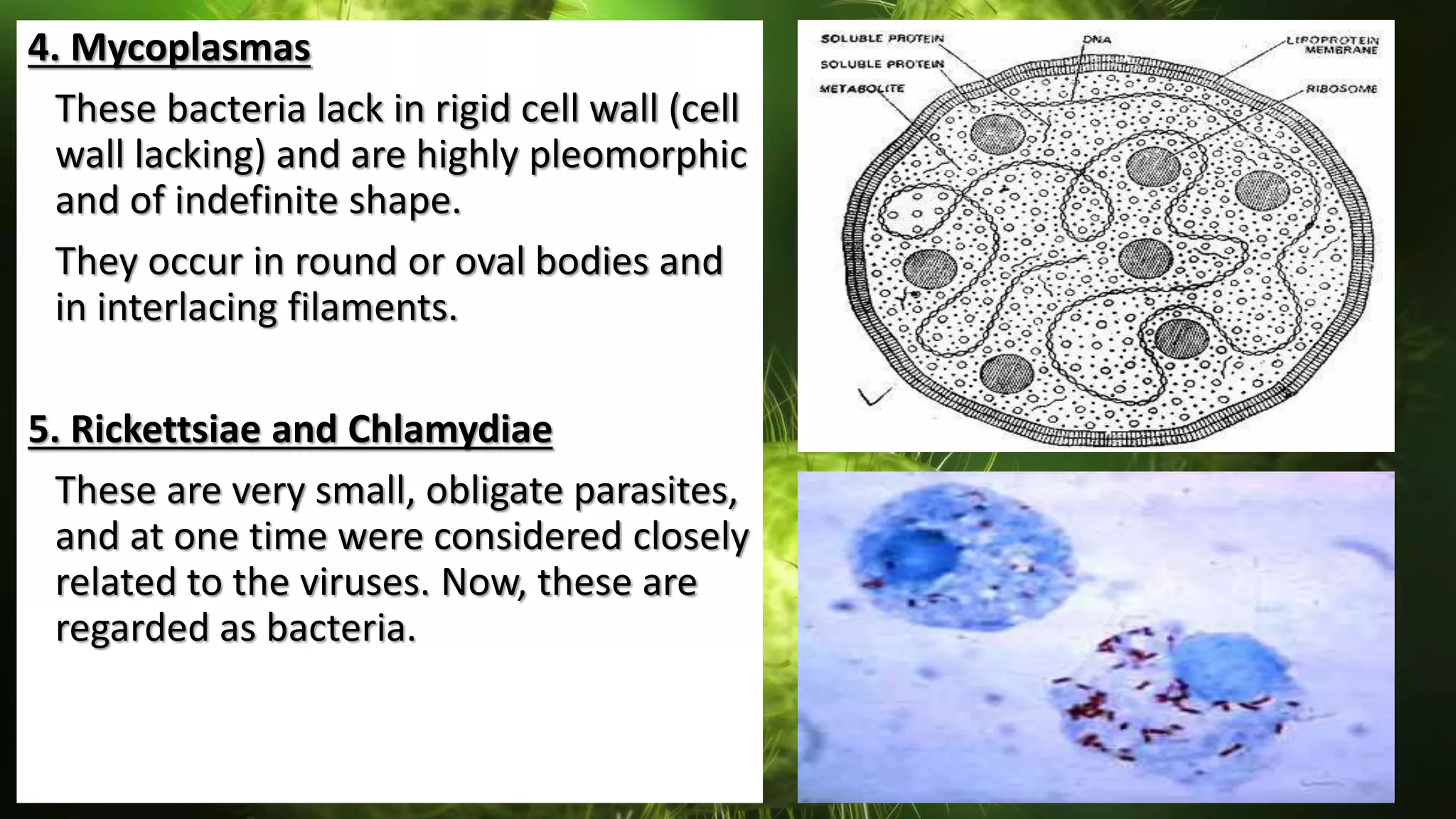
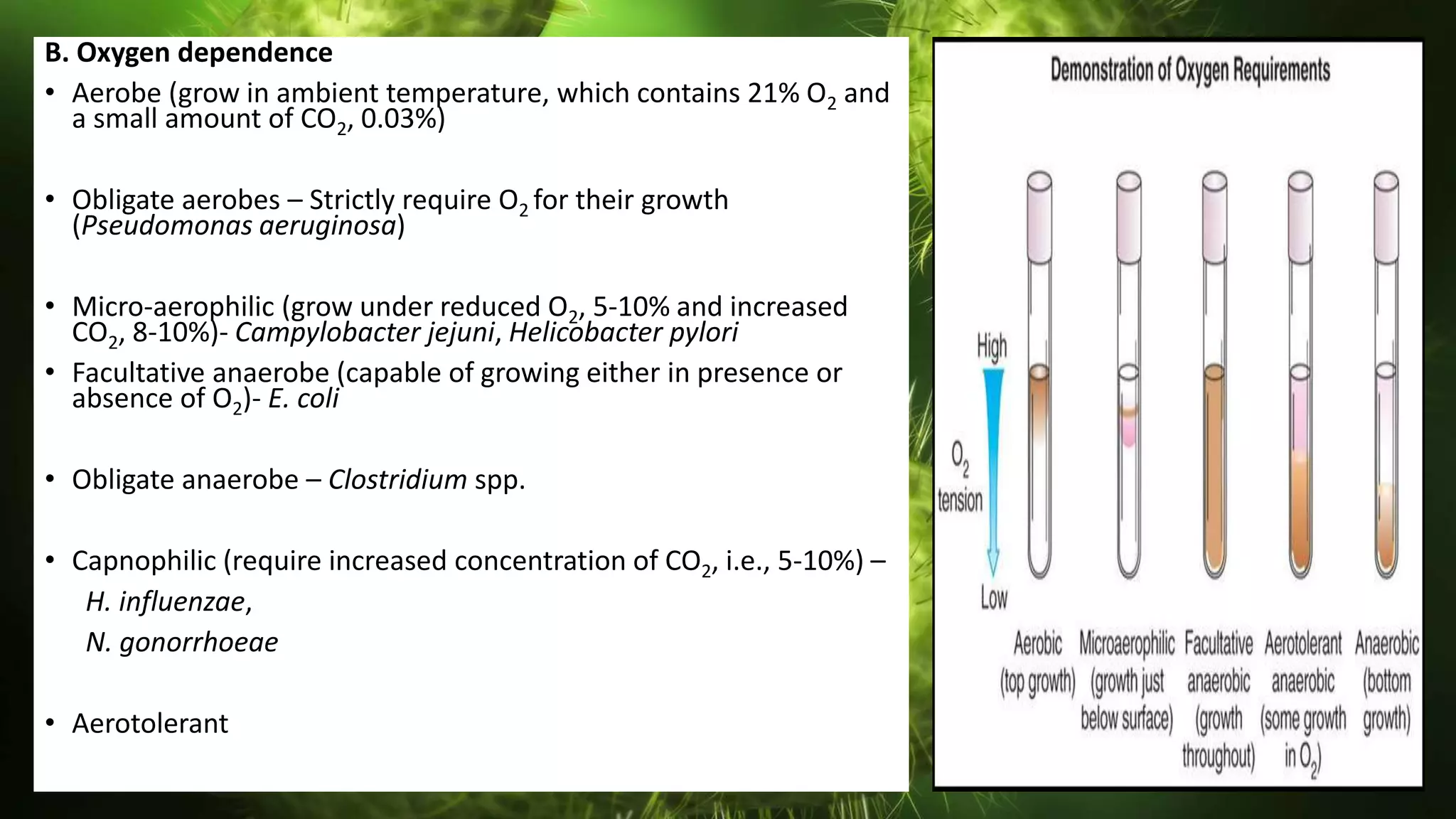
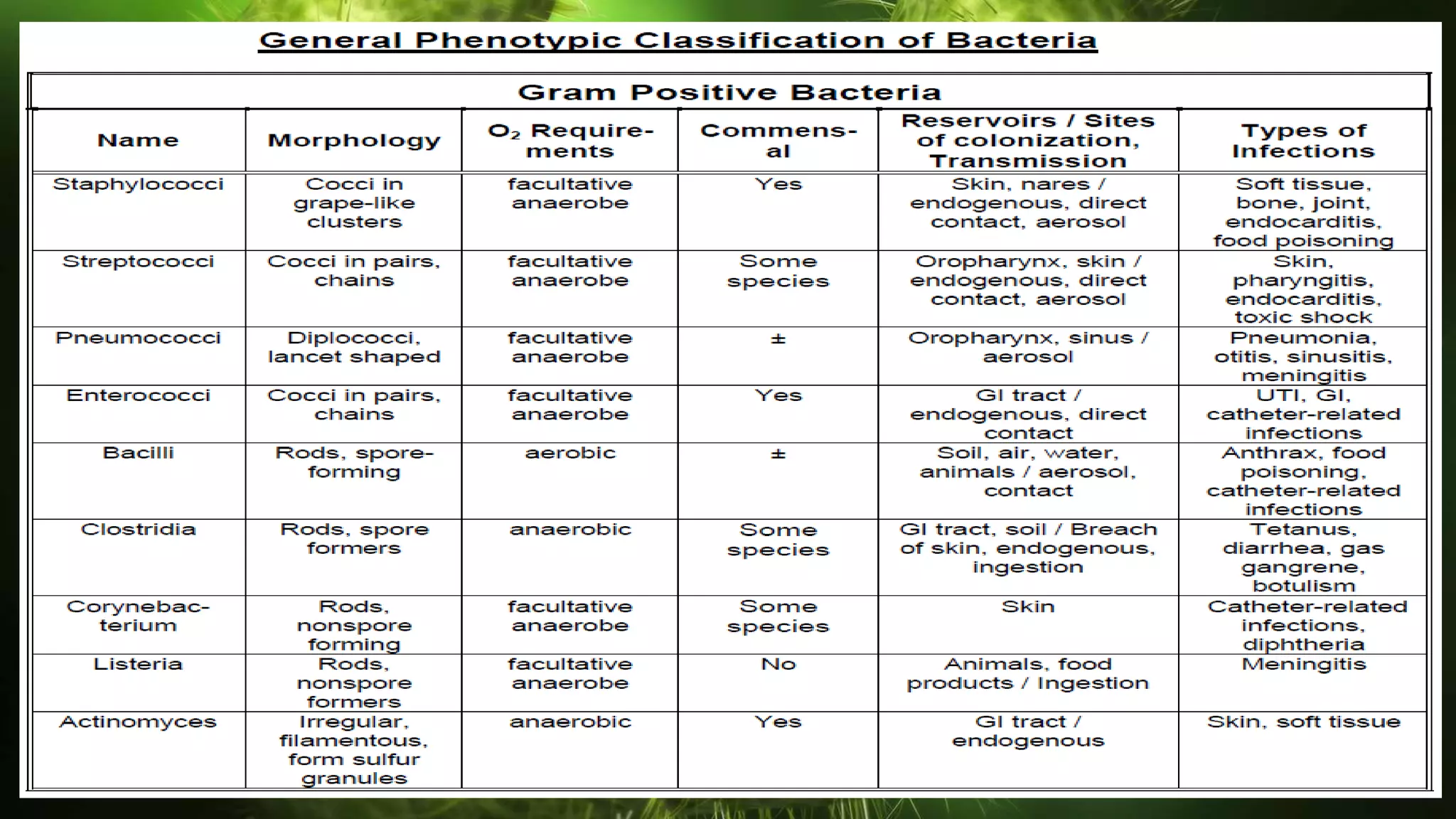
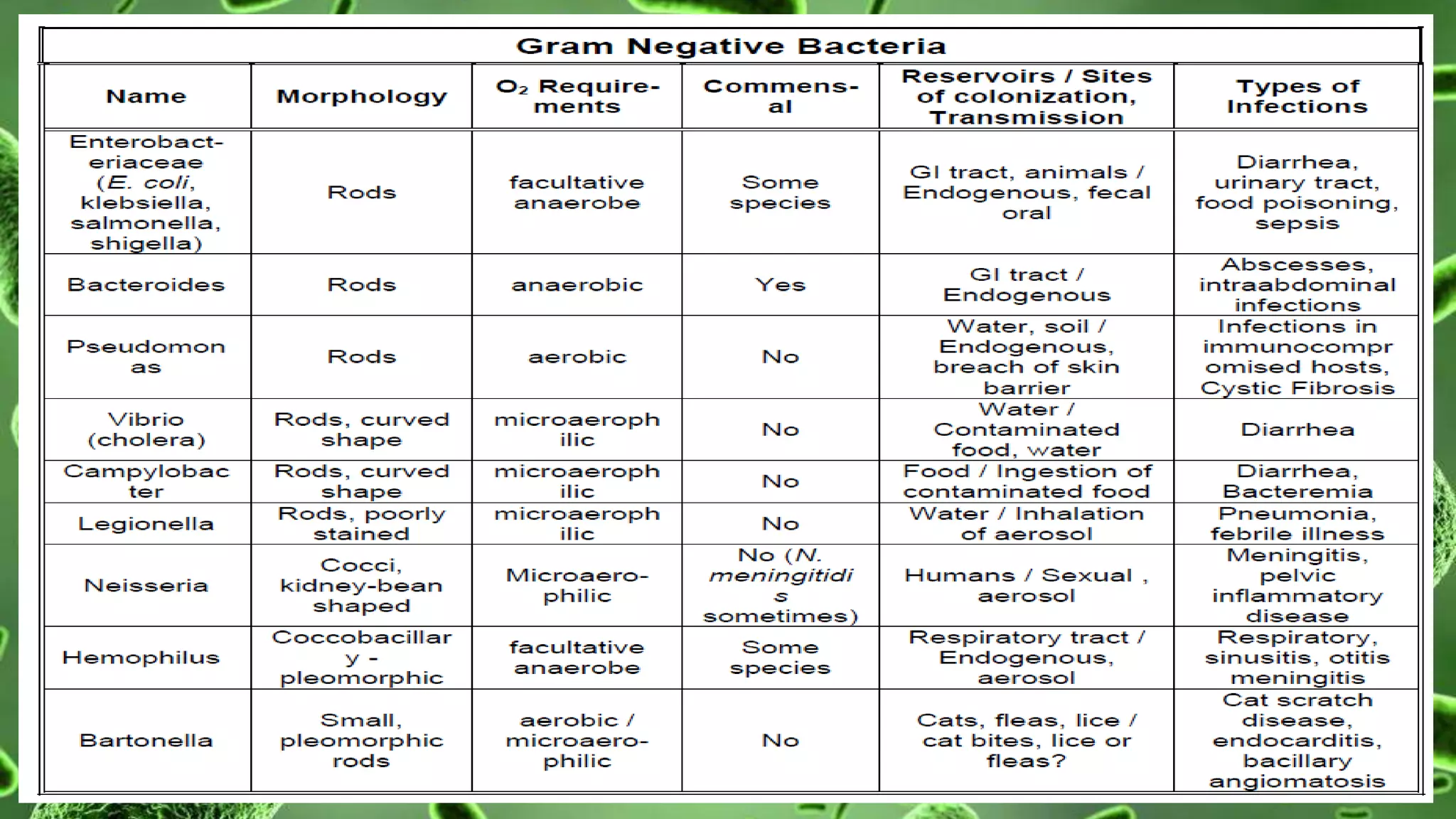
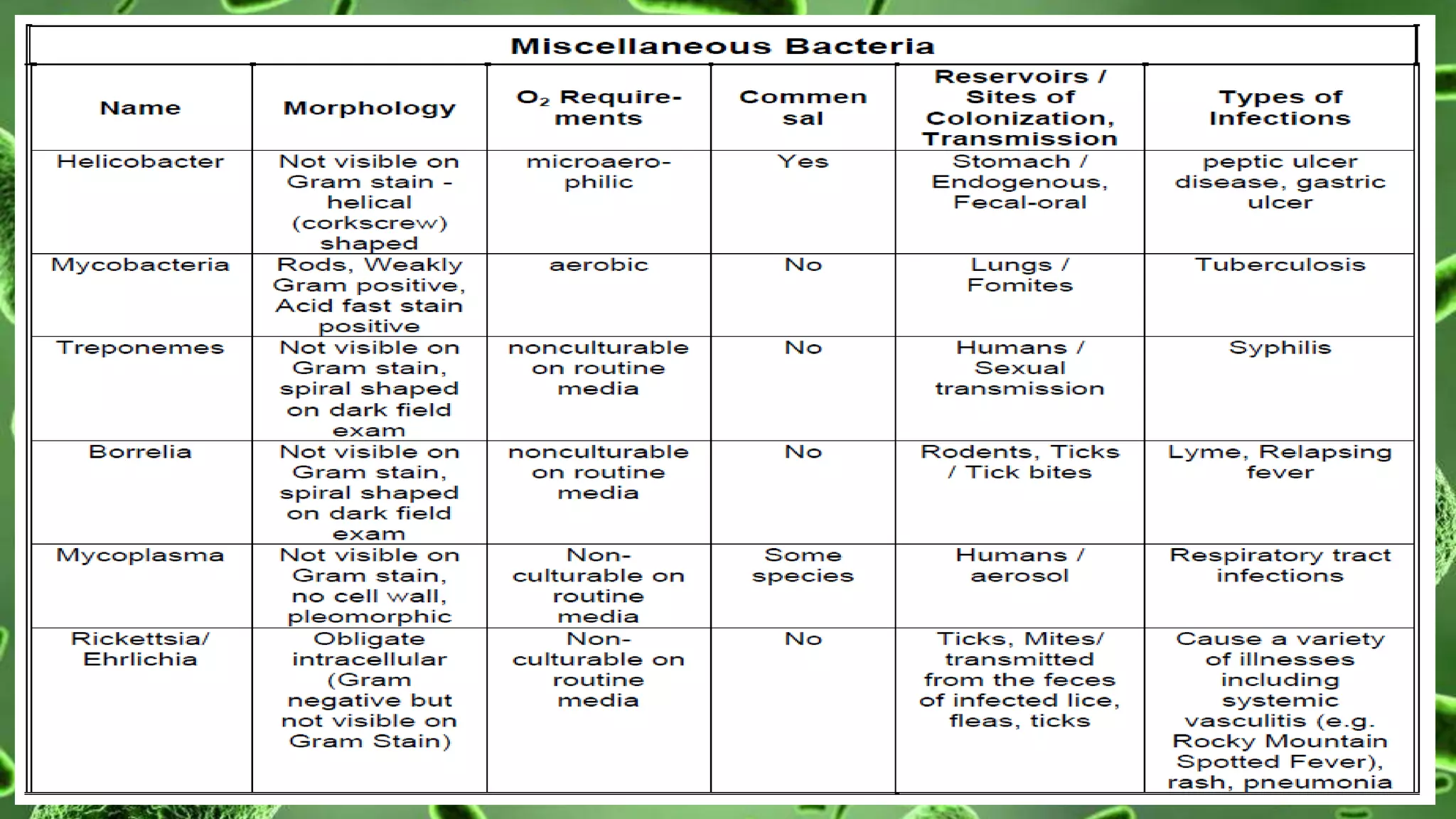
The document discusses the classification of bacteria. It explains that reliable classification is important for scientists to track the tremendous variety of microorganisms. Historically, classification has changed as new techniques became available, moving from morphology-based to genetics-based approaches. Modern classification is based on phenotypic characteristics like Gram staining and biochemical reactions as well as genotypic analysis including rRNA sequencing, DNA-DNA hybridization, and G+C content. Bacteria can be classified by their morphology, staining, culture characteristics, environmental requirements, and pathogenicity.