This document provides an overview of exodontia (tooth extraction) principles, techniques, and complications. It begins with definitions of tooth extraction and discusses the history of dental extraction forceps. Different techniques for tooth extraction are described, including the forceps technique, elevator technique, and transalveolar extraction technique involving bone removal. Factors related to patient positioning and anesthesia are outlined. Indications, contraindications, and complications of tooth extraction are summarized. The document concludes with descriptions of various extraction techniques and post-operative care.















![A. Absolute : Central Haemangioma. May cause uncontrolled bleeding.
A-V malformation.
B. Relative :
When some precautions have to be taken.
1. Local Acute cellulitis.
ANUG.
2. Systemic Uncontrolled Diabetes Mellitus,
Hypertension.
Bleeding disorders.
Cardiovascular diseases.
Liver disorders.
Patients on long-term steroid therapy.
Teeth that have undergone radiation [6 months – 1 yr ].](https://image.slidesharecdn.com/exodontia-130425161232-phpapp02/85/Exodontia-18-320.jpg)




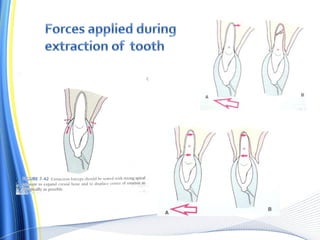





































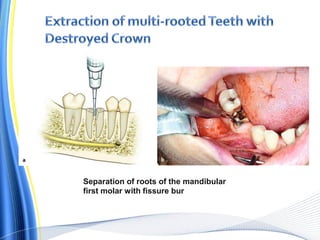

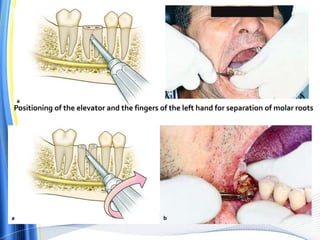

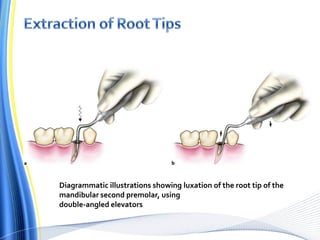






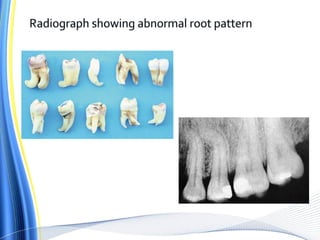












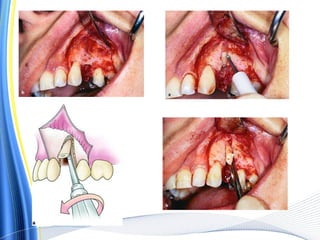
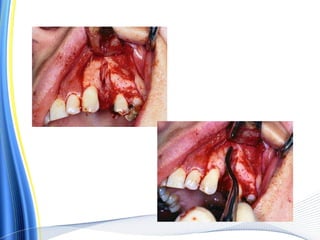

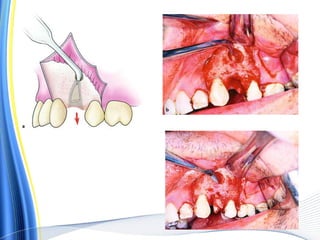

















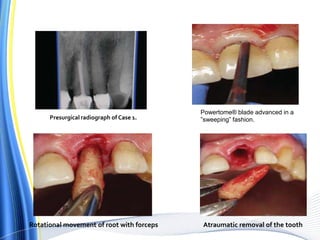

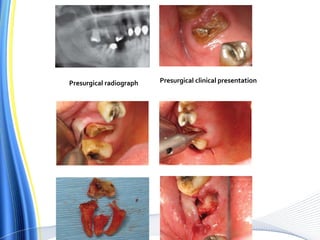





![ For the surgical extraction of the teeth, the covering bone was first
ablated, layer by layer, using the Er:YAG laser.
In the case of the fiber-optic Er:YAG [erbium:yttrium-aluminum
garnet ], laser the fiber is closely guided around the teeth, creating a
narrow gap with minimal bone loss.
The benefits of laser therapy include the creation of a bloodless
surgical field and thus improved visualization during surgery,
decreased postoperative pain, and limited scarring and contraction.
Time consuming, sound and smell, significantly inhibition the
laser cutting because of the overall volume of irrigation and blood
covering the bone surface.](https://image.slidesharecdn.com/exodontia-130425161232-phpapp02/85/Exodontia-131-320.jpg)