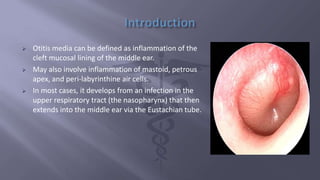
This document discusses otitis media, an inflammation of the middle ear. It begins with an introduction and case presentation of a 4 year old boy with ear pain, fever, and cough. It then covers the epidemiology, anatomy, classification, etiology, risk factors, pathology, clinical features, differential diagnosis, management, and complications of otitis media. The peak incidence is in children aged 1-4 years and is more common in boys. Acute otitis media, otitis media with effusion, chronic suppurative otitis media, and adhesive otitis media are subtypes discussed. Pneumoniae, influenzae, and Moraxella are common bacterial causes while viruses like R





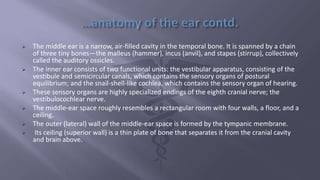









![1. Catarrhal stage: Is characterized by occlusion of Eustachian tube and congestion
of middle ear.
2. Stage of exudation: Exudate collects in the middle ear and ear drum is pushed
laterally. Initially the exudate is mucoid, later it becomes purulent.
3. Stage of suppuration: Pus in the middle ear collects under tension, stretches the
drum & perforates it by pressure necrosis & the exudate starts escaping into
external auditory canal
4. Stage of healing: The infection starts resolving from any of the stages mentioned
& usually clears up completely without leaving any sequelae.
5. Stage of complications: Infection may spread to the mastoid antrum. Initially it
causes Catarrhal mastoiditis [congestion of the mastoid mucosa], stage of
coalescent mastoiditis & later empyema of the mastoid.](https://image.slidesharecdn.com/otitismedia-oluafolabi-170219121000/85/A-Presentation-on-Otitis-Media-by-Boluwatife-O-Afolabi-18-320.jpg)