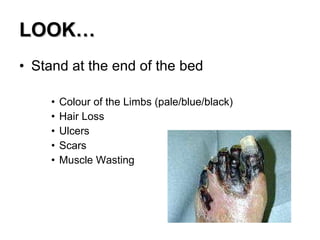
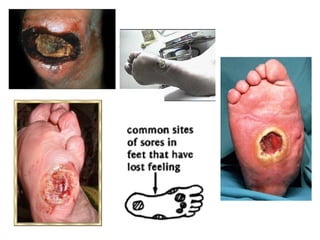
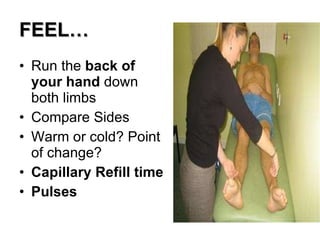
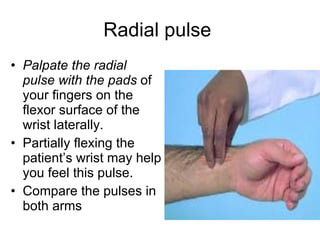
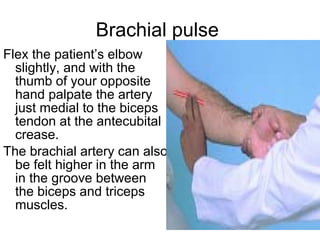
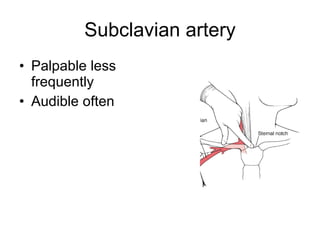
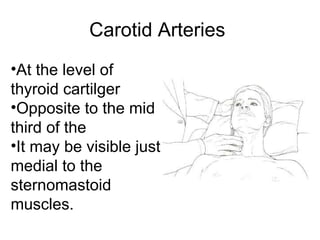
This document provides guidance on performing a peripheral vascular examination, including examining the arms and legs to check for signs of vascular disease. It describes how to inspect and palpate pulses in the upper and lower limbs, listen for bruits, and perform additional tests like Buerger's angle test. The document also covers examining the venous system, including inspection for varicose veins, palpating for fascial defects, and tests like Trendelenburg's test to check for venous incompetence.