1. Proteinuria refers to excess protein in the urine, usually over 150 mg per day. It can occur via three main mechanisms: leaky glomerular filtration barrier, malfunctioning tubular reabsorption, or overflow proteinuria.
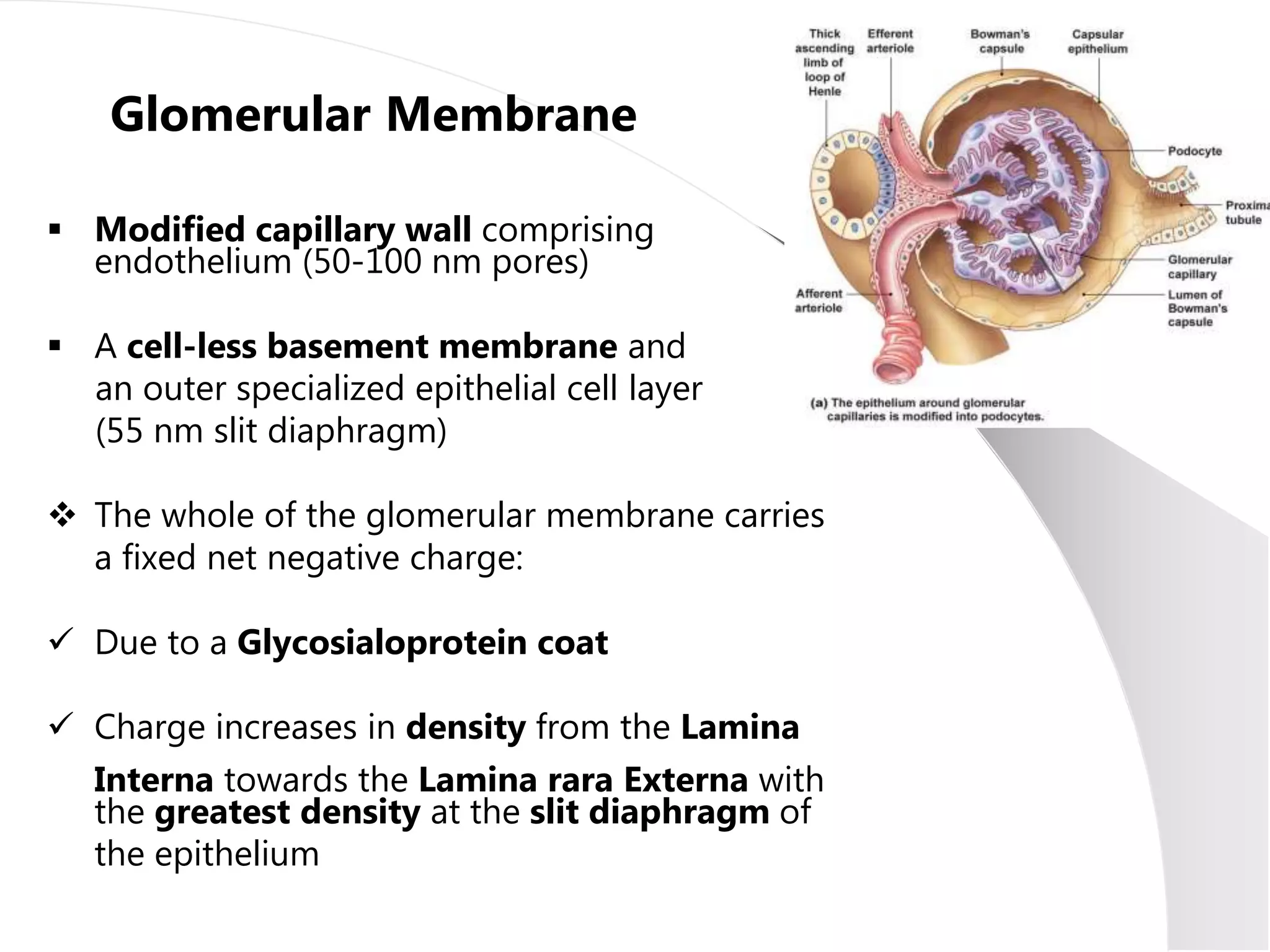
2. The glomerular filter normally excludes large proteins while smaller proteins pass through and are reabsorbed by tubules. Proteinuria occurs when this barrier or reabsorption is damaged.
3. Proteinuria is an important marker for kidney disease staging and prognosis, with higher levels associated with worse outcomes. The type and selectivity of proteinuria can help classify underlying glomerular diseases.



























![Urine protein selectivity and classification of
glomerulonephritis
Selectivity: based on assumption that there may be differentia
filtration of large molecular weight proteins in glomerular dise
Protein selectivity is based on a comparison of the relative
clearance of IgG(150 000 Da) and transferrin (69 000 Da)
calculated as follows:
Clearance of IgG = [IgG]U x [Trans]P
Clearance of transferrin [IgG]P x [Trans]U
where:
[IgG ]u = Urine IgG concentration
[Trans]p = Plasma transferrin concentration
[IgG ]p = Plasma IgG concentration
[Trans]u = Urine transferrin concentration](https://image.slidesharecdn.com/proteinuriaandparaproteinemias-200130090732/75/Proteinuria-and-paraproteinemias-30-2048.jpg)








![Methods of assessing tubular damage
Tests of reabsorption of glucose, phosphate, bicarbonate
and amino acids
High molecular weight protein are commonly used
markers of renal tubular damage
N-Acetyl β-D Glucosaminidase (NAG) [1,50,000
Da]
Lactate Dehydrogenase
γ-glutamyl transferase
Alkaline phosphatase](https://image.slidesharecdn.com/proteinuriaandparaproteinemias-200130090732/75/Proteinuria-and-paraproteinemias-39-2048.jpg)










![Monoclonal Proteins
Appear as homogenous, compact bands on
electrophoretic separations
Detectable in serum are intact immunoglobulins; if
there is renal damage, leaks into Urine
Low Molecular weight fragments and monoclonal free
light chains [Bence Jones Proteins (BJPs)] can pass
through normal glomeruli and appear in urine [In the
absence of Renal Damage, may be detected in serum too]](https://image.slidesharecdn.com/proteinuriaandparaproteinemias-200130090732/75/Proteinuria-and-paraproteinemias-50-2048.jpg)























![Gamma Heavy Chain Disease (Franklin's Disease)
Frequently associated with Autoimmune diseases, especially Rheumatoid
Arthritis
Diagnosis: Anomalous serum M component [Often <20 g/L (<2 g/dL)]
Alpha Heavy Chain Disease (Seligmann's Disease)
Most common of the heavy chain diseases
Closely related to a malignancy known as Mediterranean lymphoma
Alpha heavy chains assesment is difficult
Mu Heavy Chain Disease
Seen in patients with Chronic Lymphocytic Leukemia
Presence of vacuoles in the malignant lymphocytes and the excretion of
kappa light chains in the urine](https://image.slidesharecdn.com/proteinuriaandparaproteinemias-200130090732/75/Proteinuria-and-paraproteinemias-74-2048.jpg)


