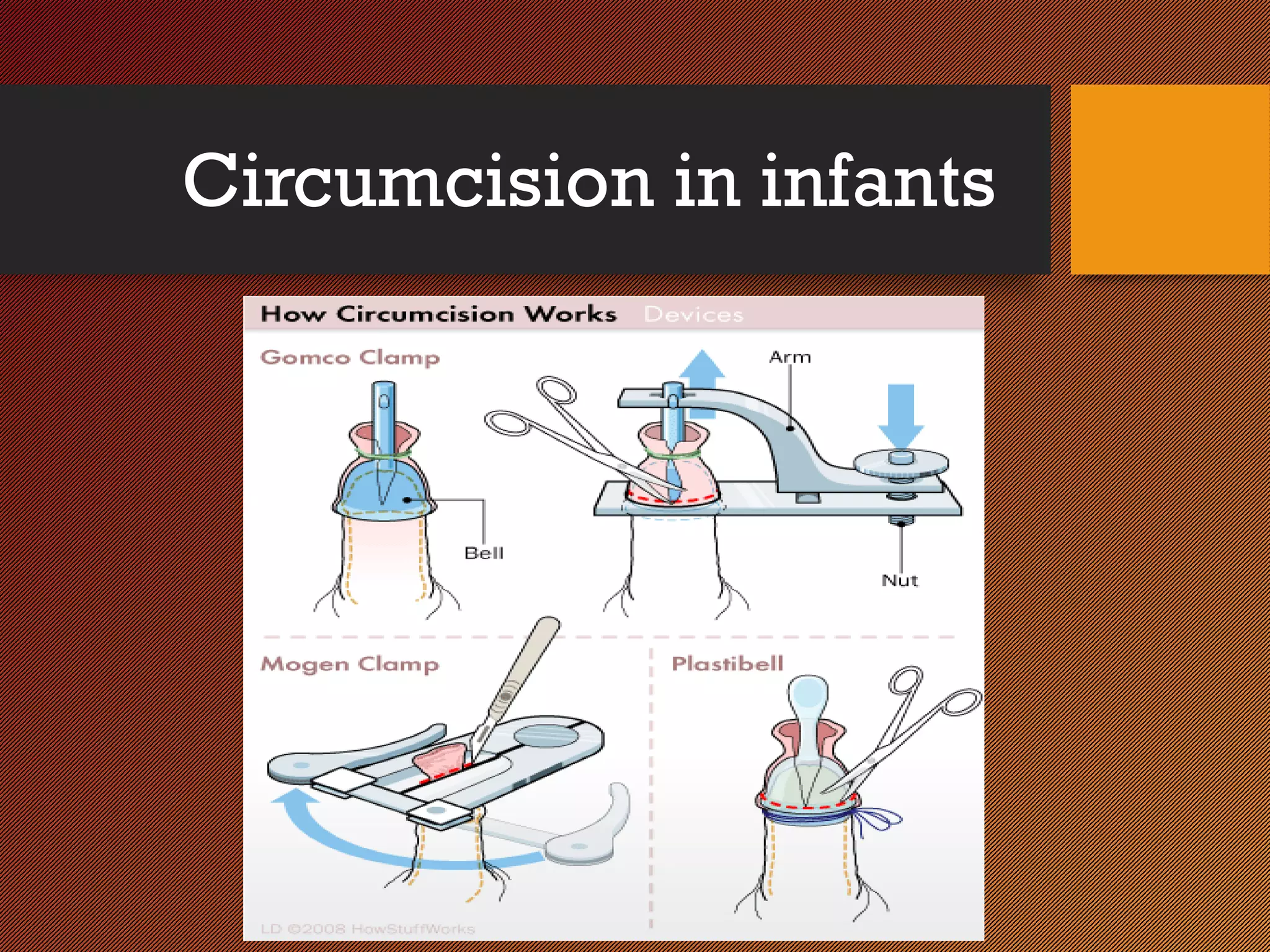
The document discusses phimosis, paraphimosis, and circumcision, detailing their definitions, causes, and treatment options. It highlights that phimosis can be physiological and may resolve naturally, while paraphimosis requires careful management to prevent complications. Circumcision is explored as a treatment for various conditions associated with these disorders, along with its historical context, indications, techniques, and potential complications.