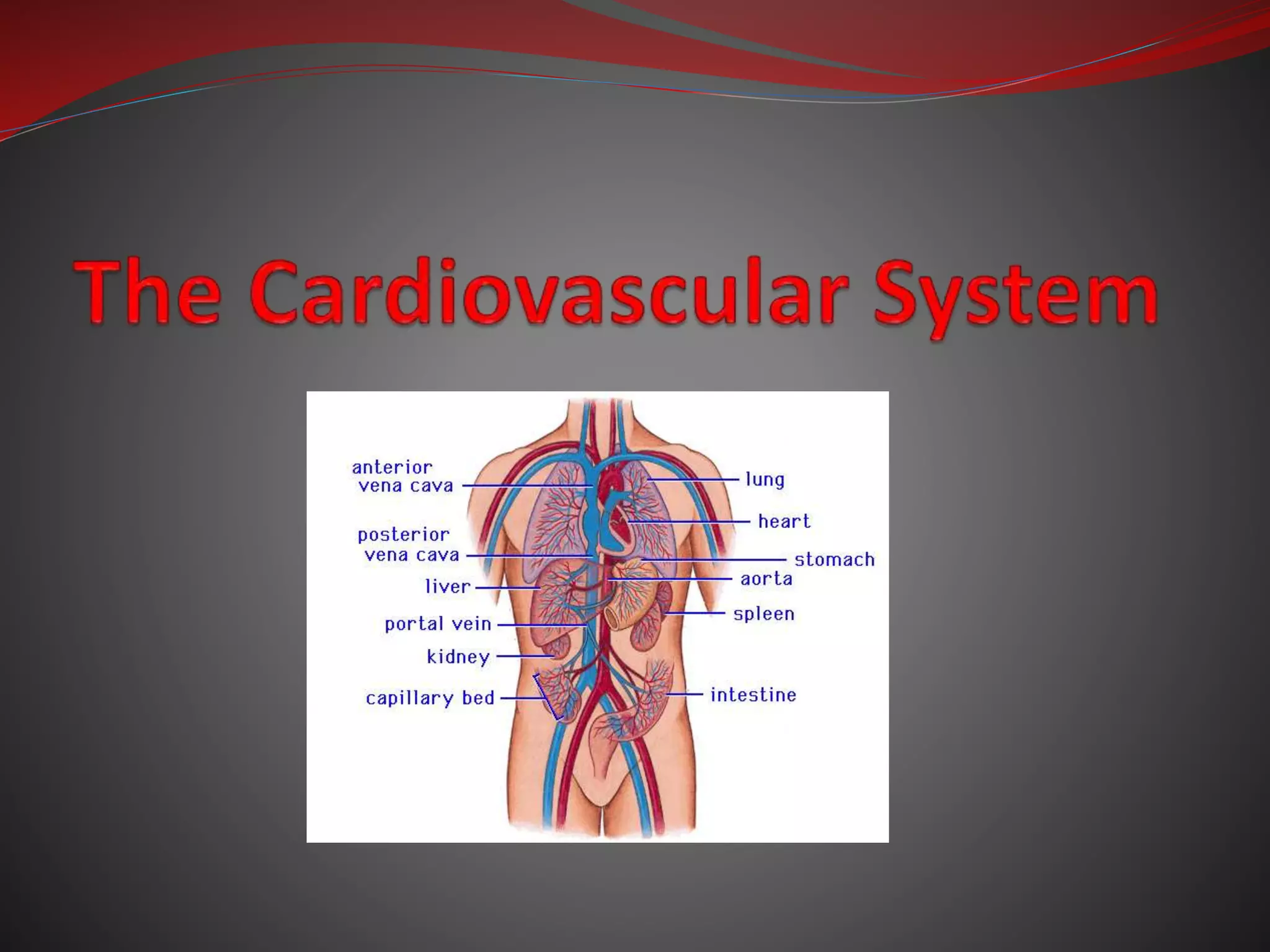
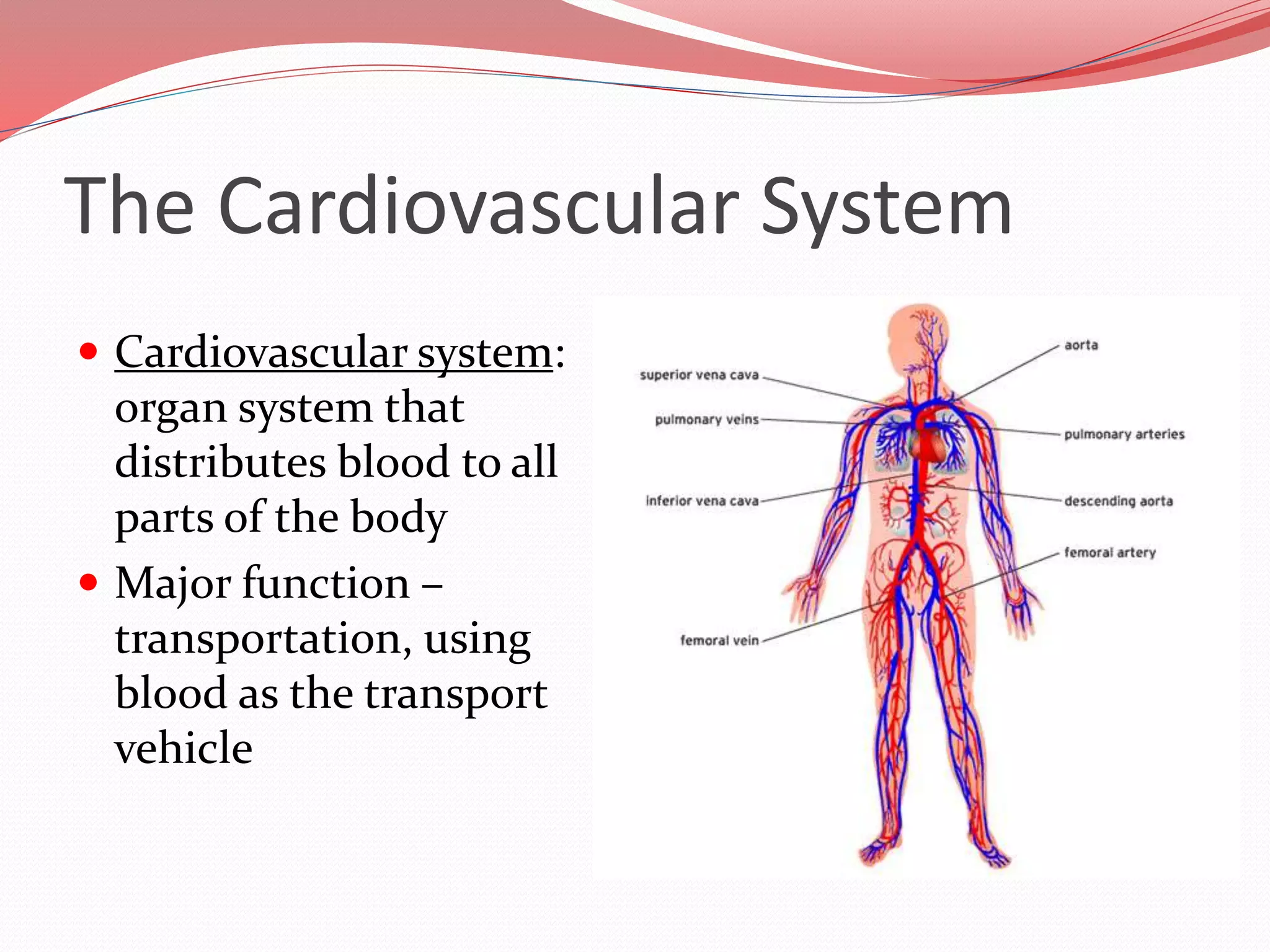
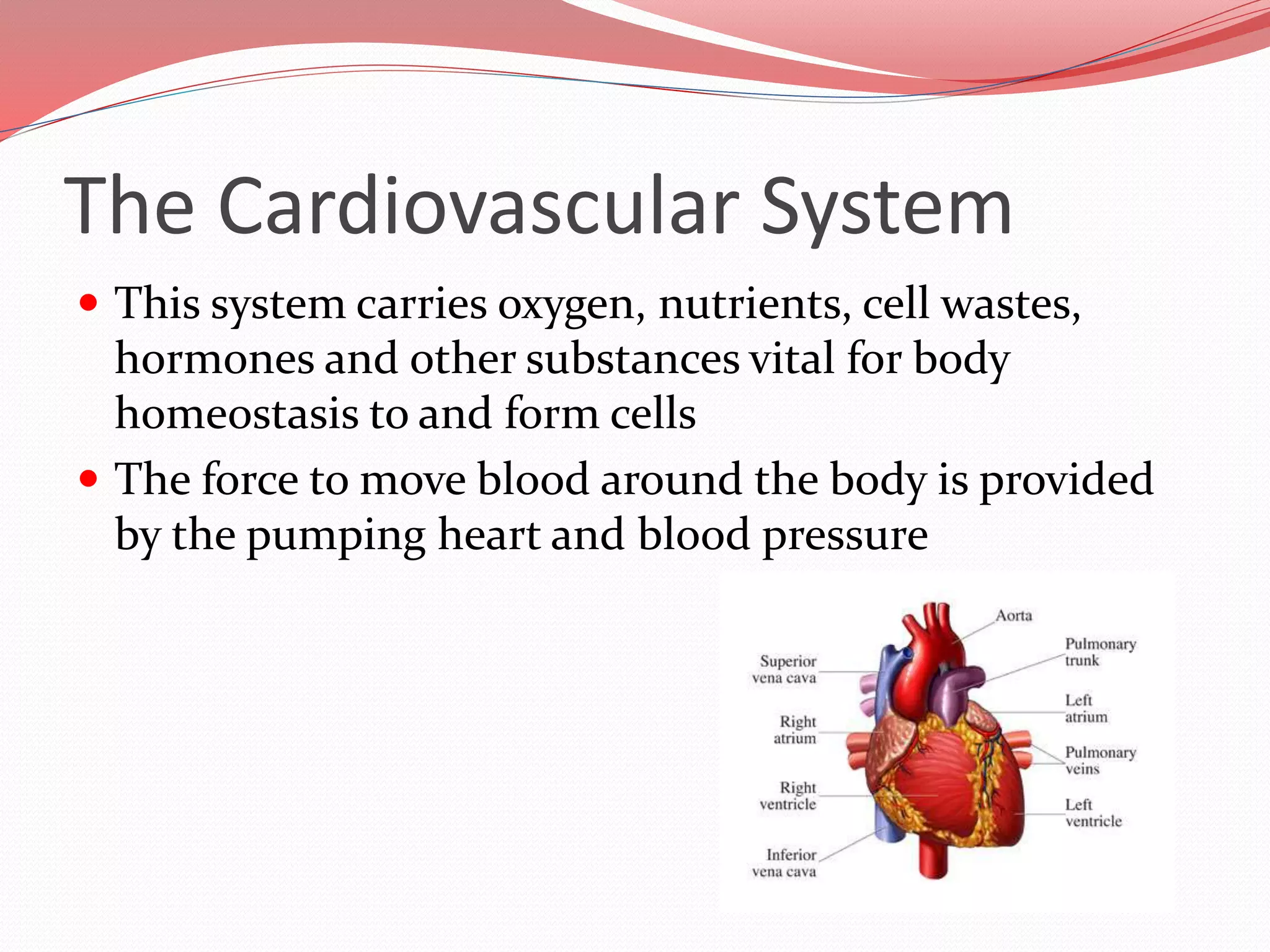
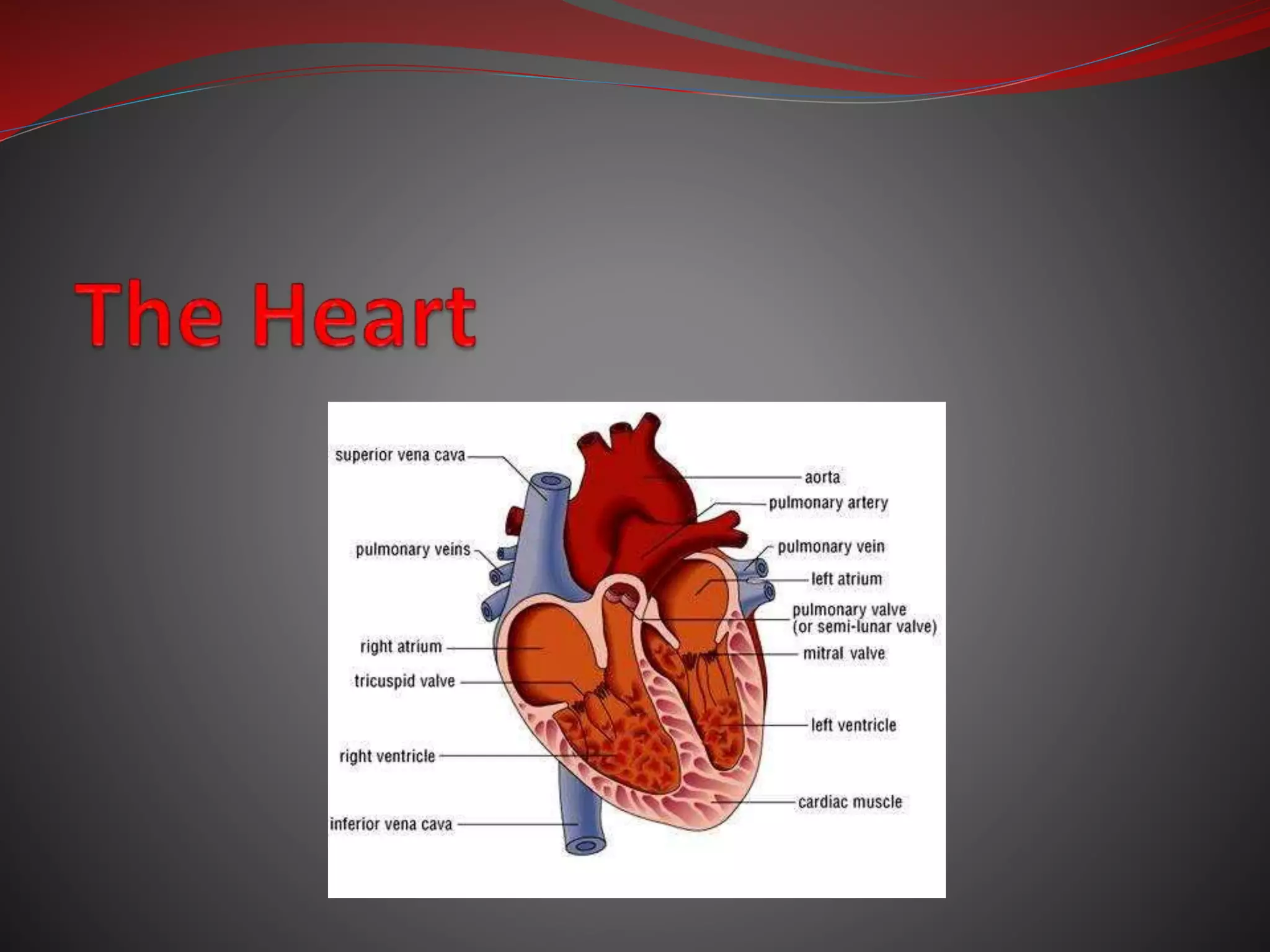
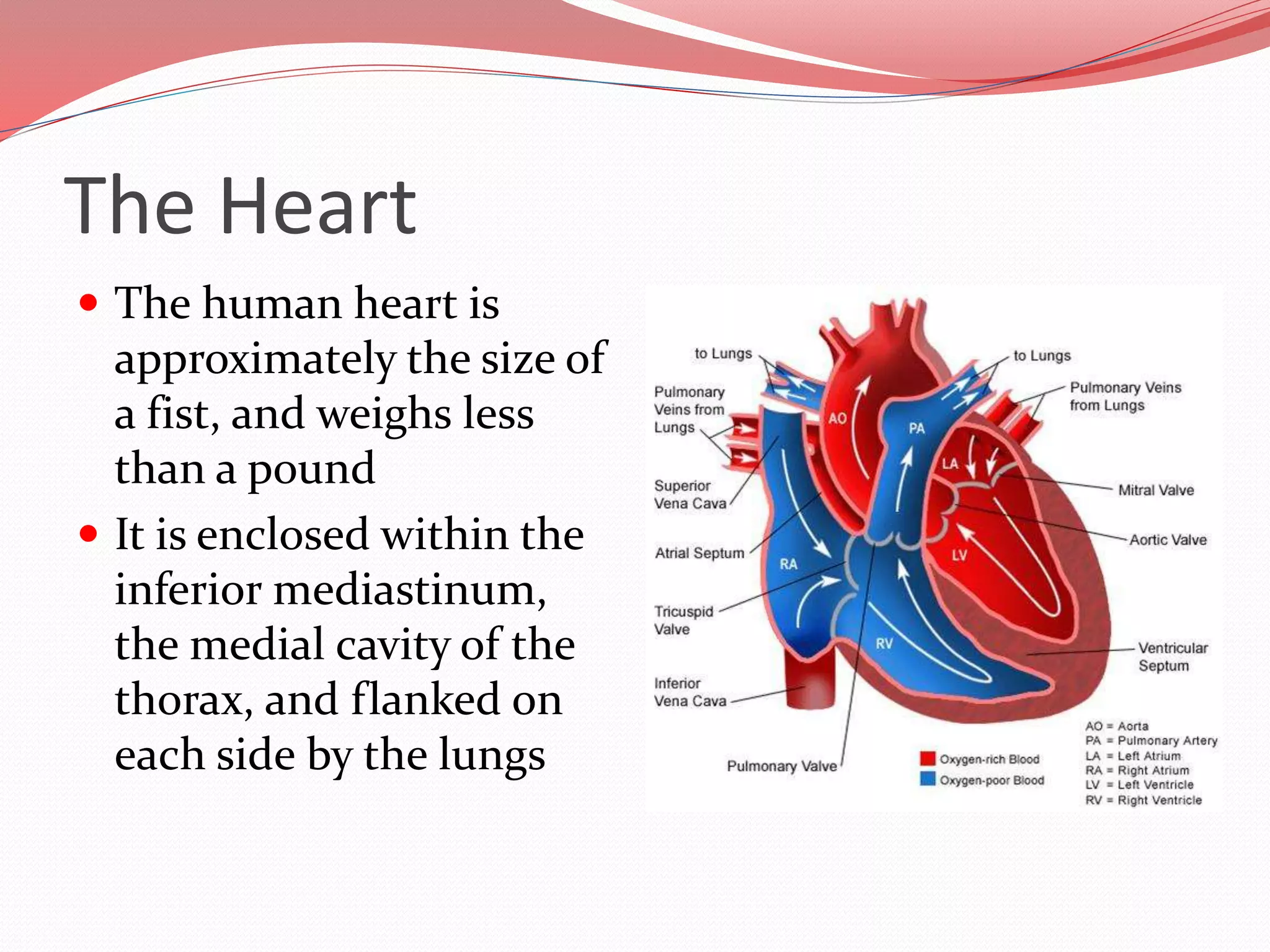
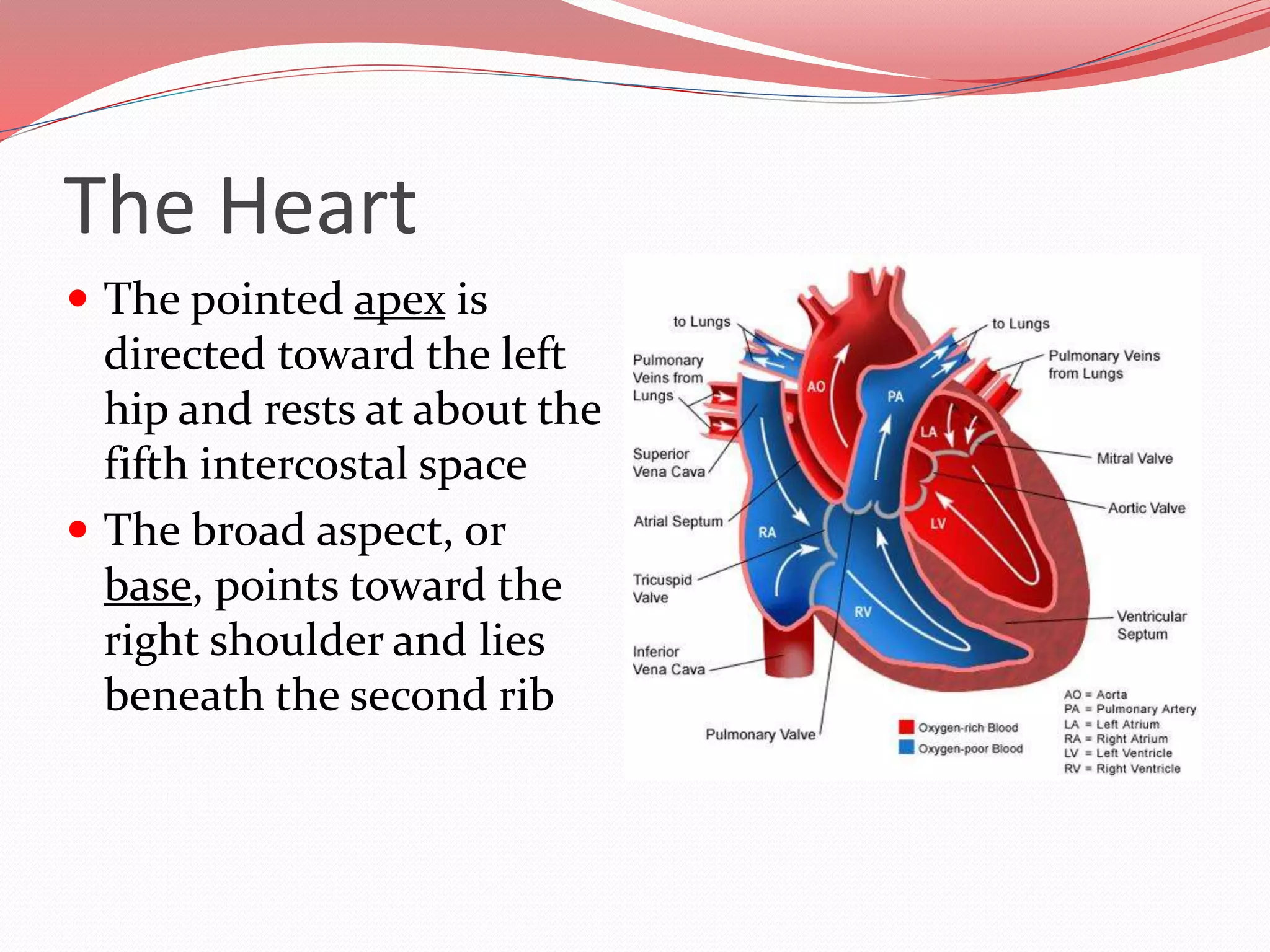
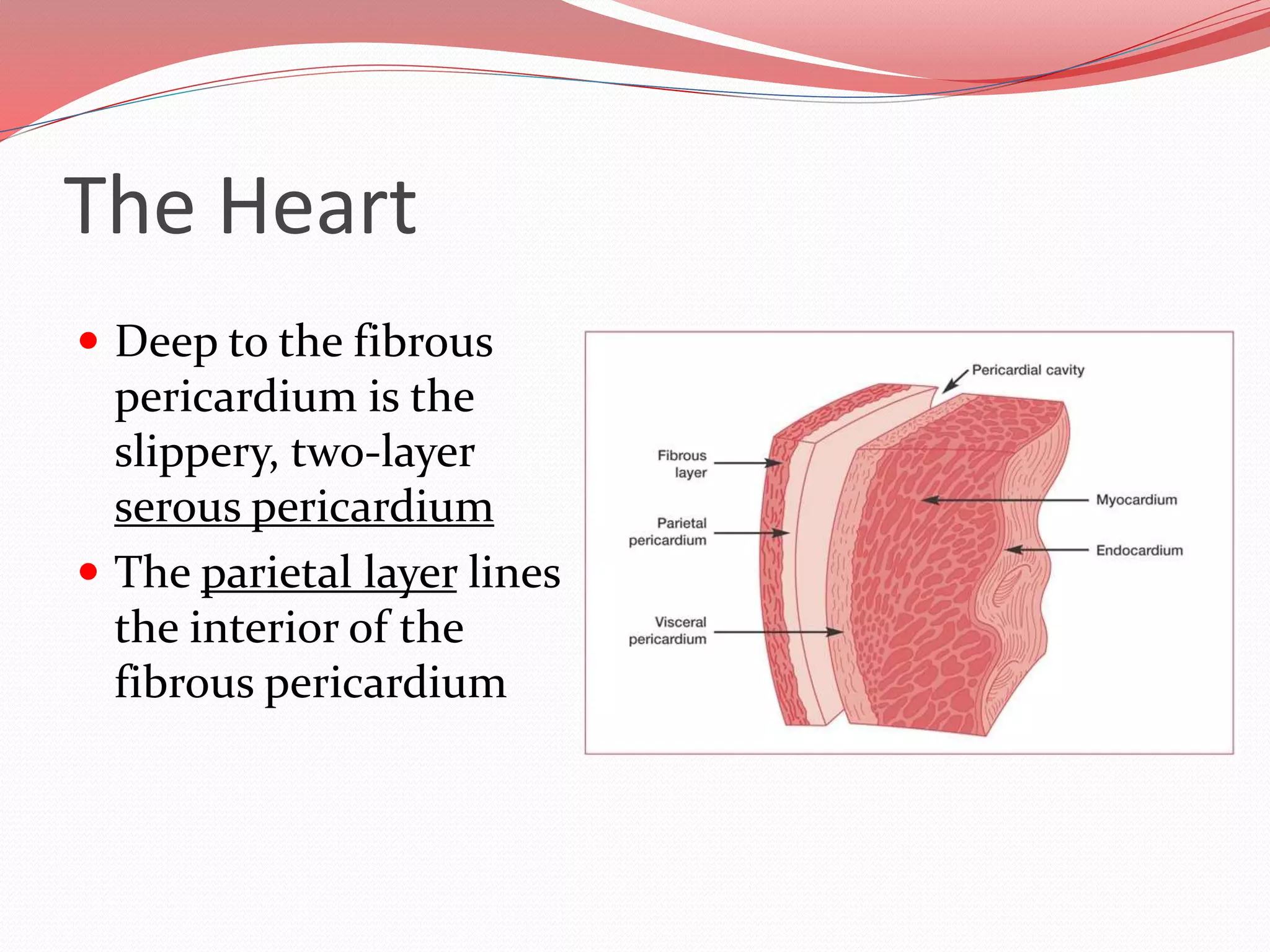
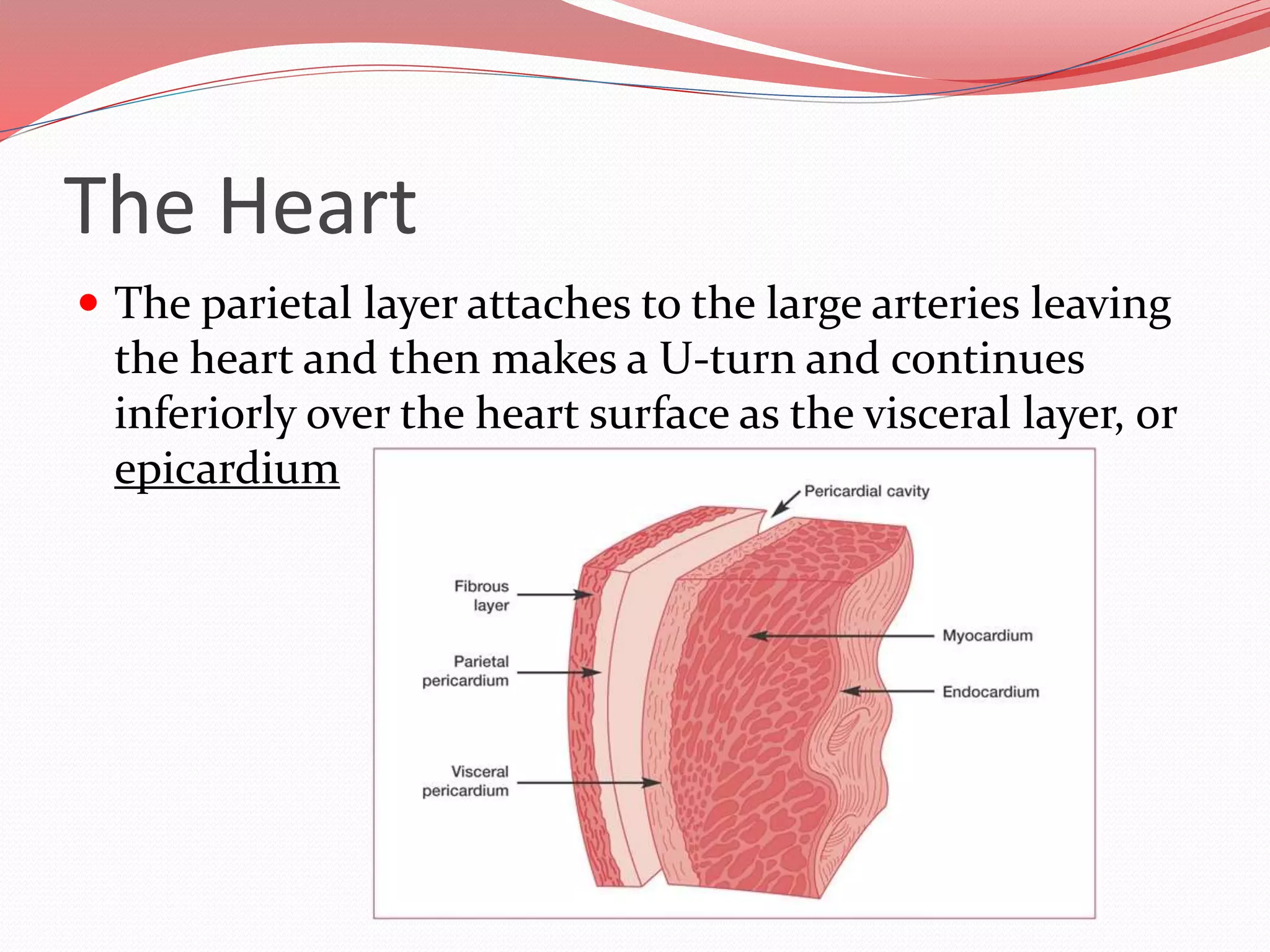
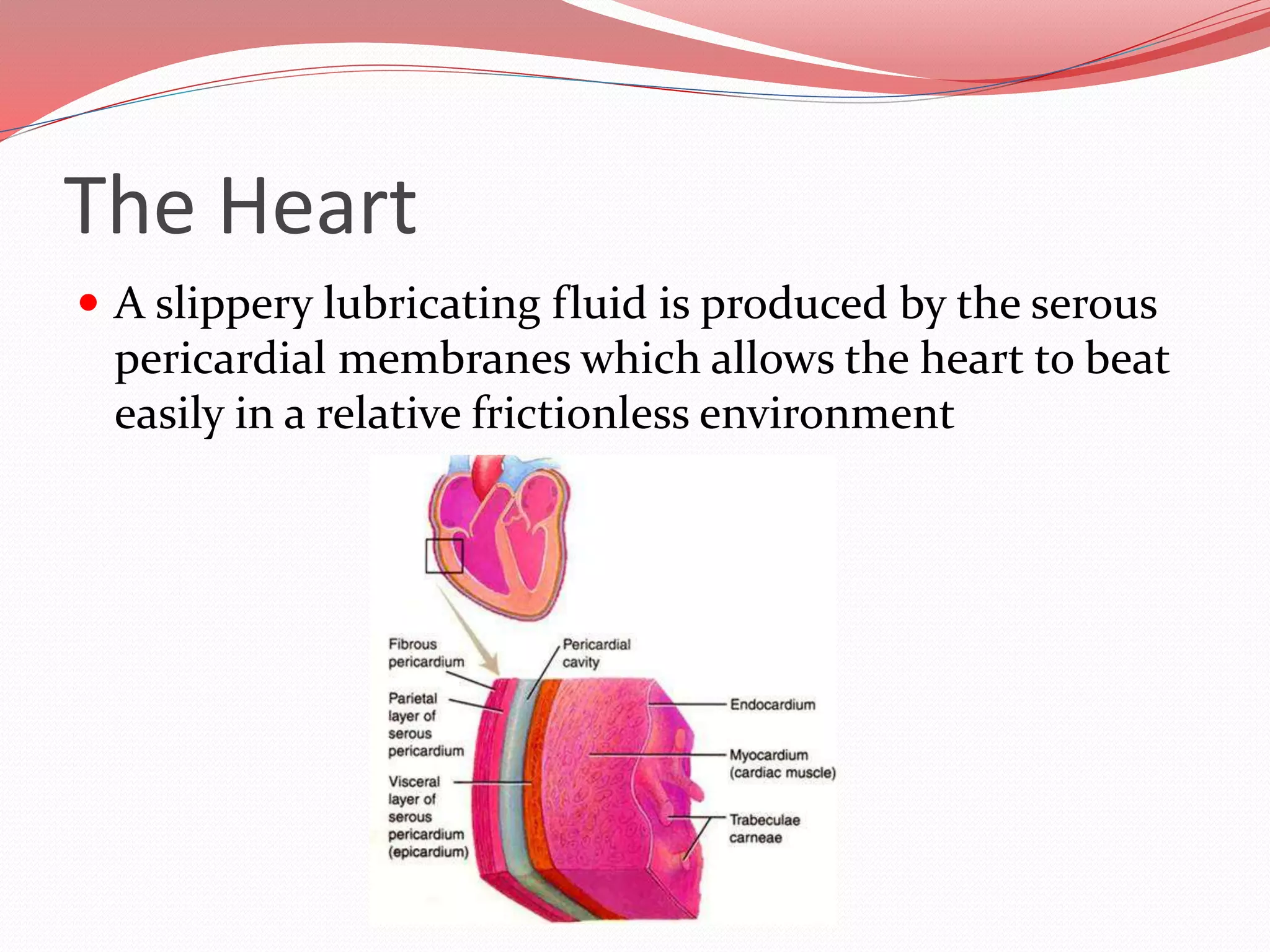
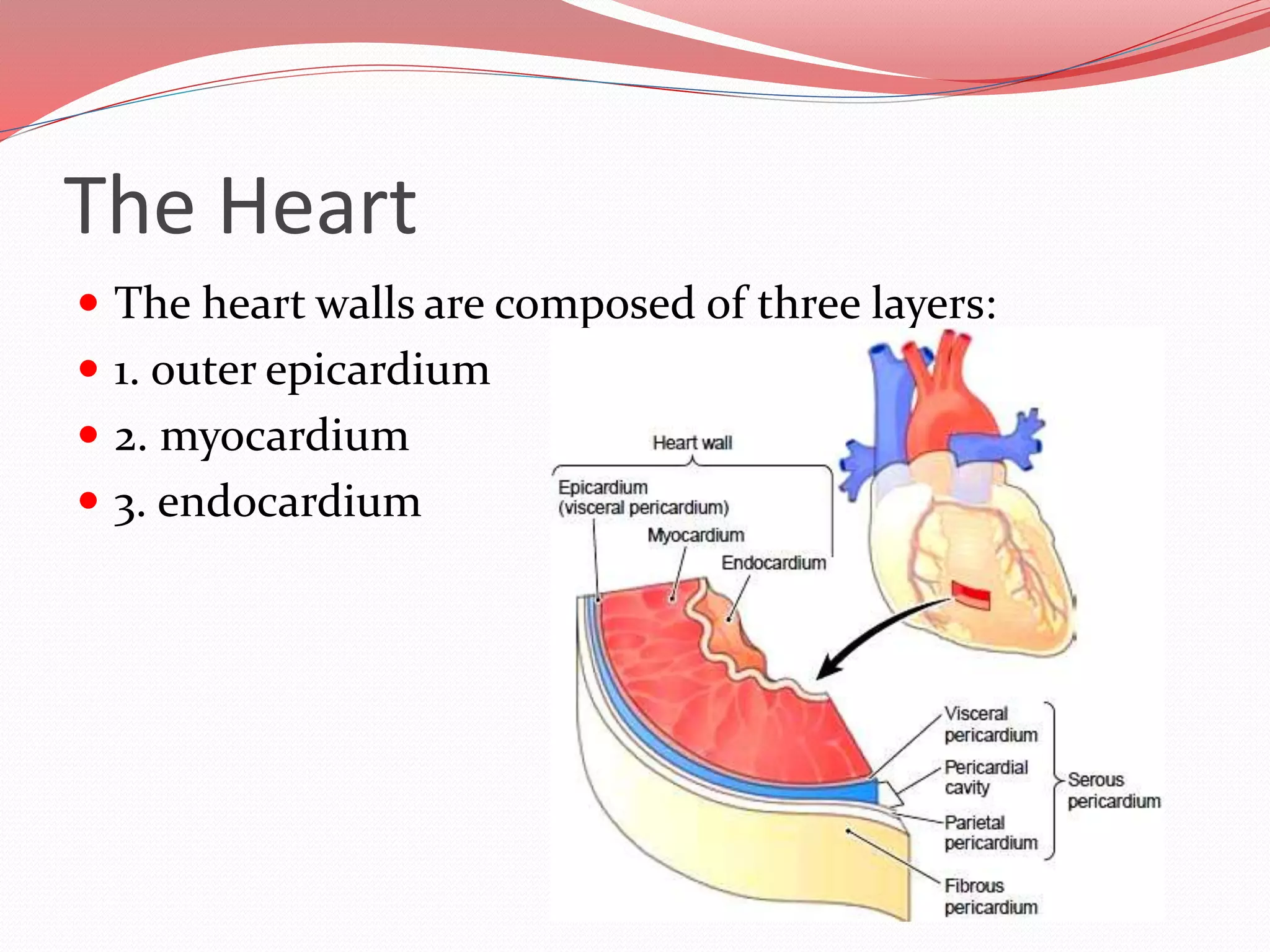
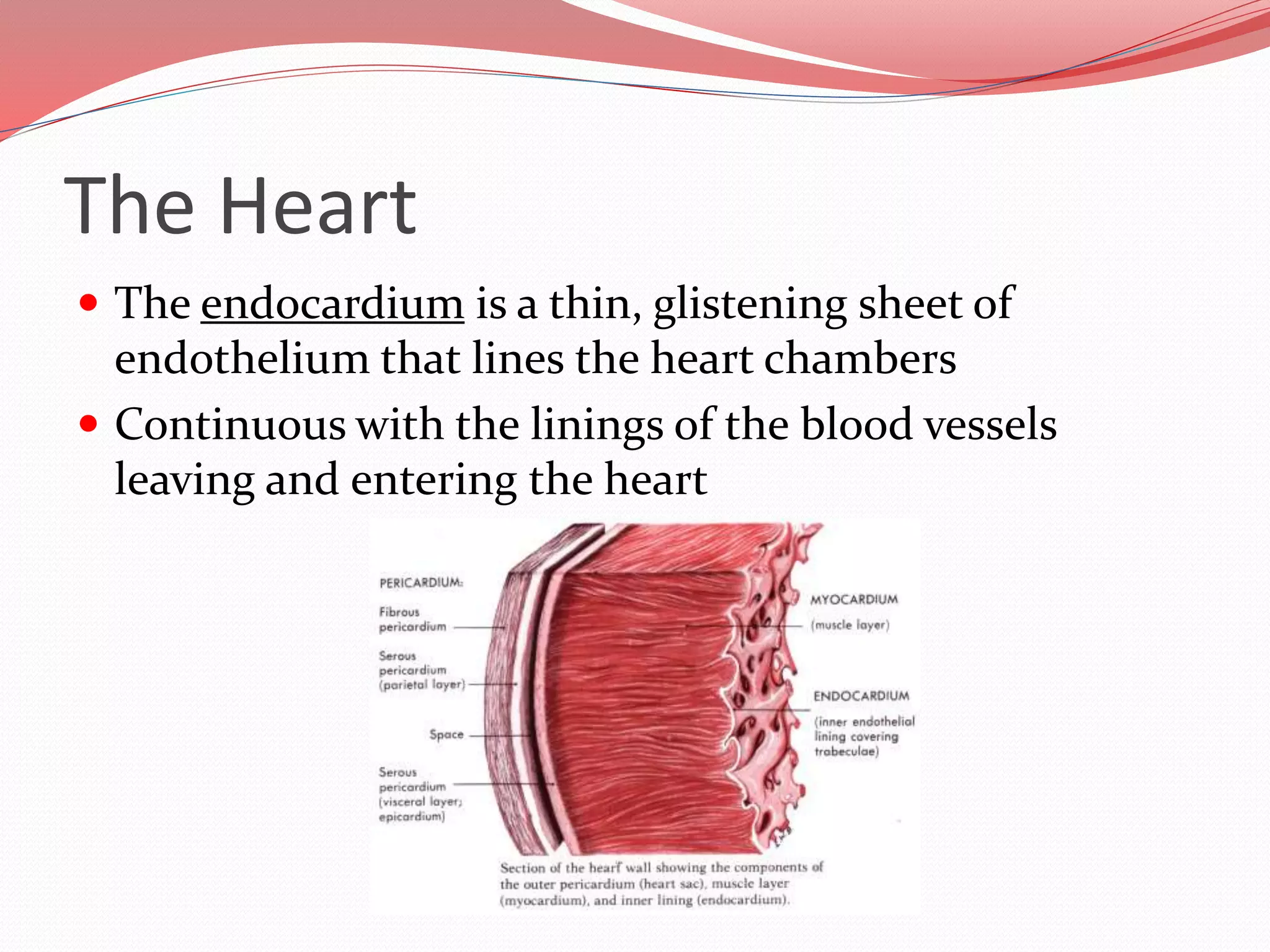
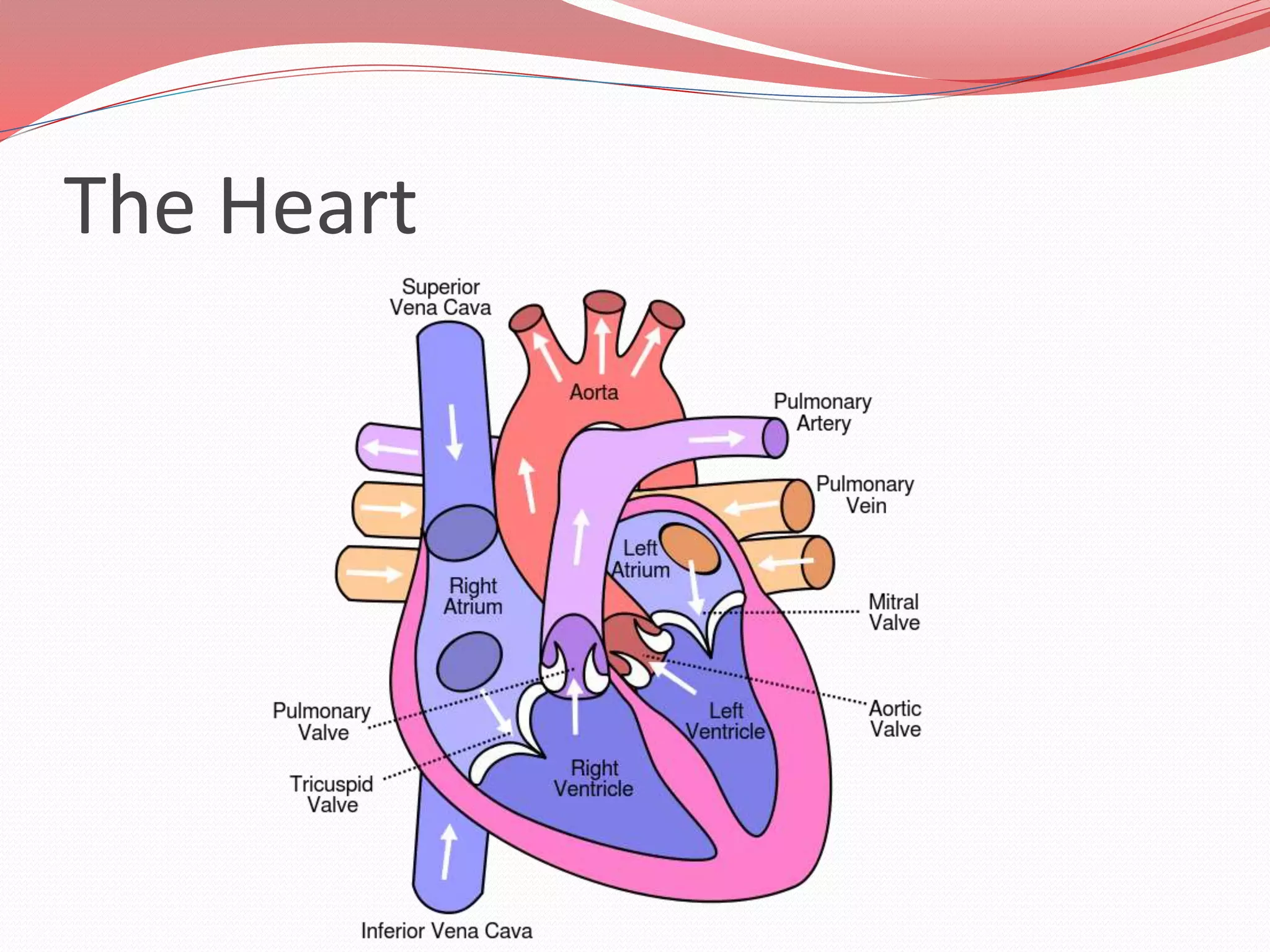
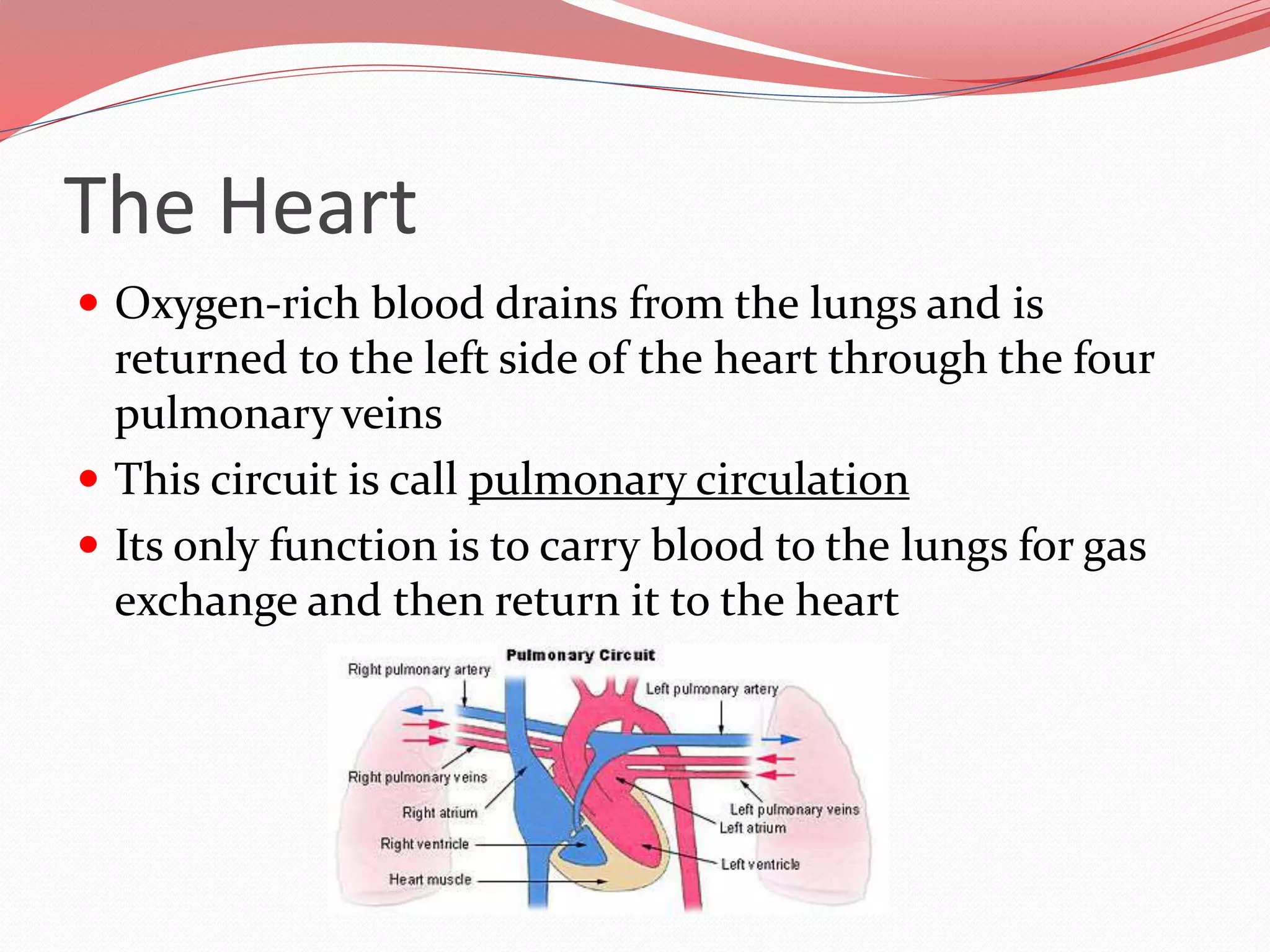
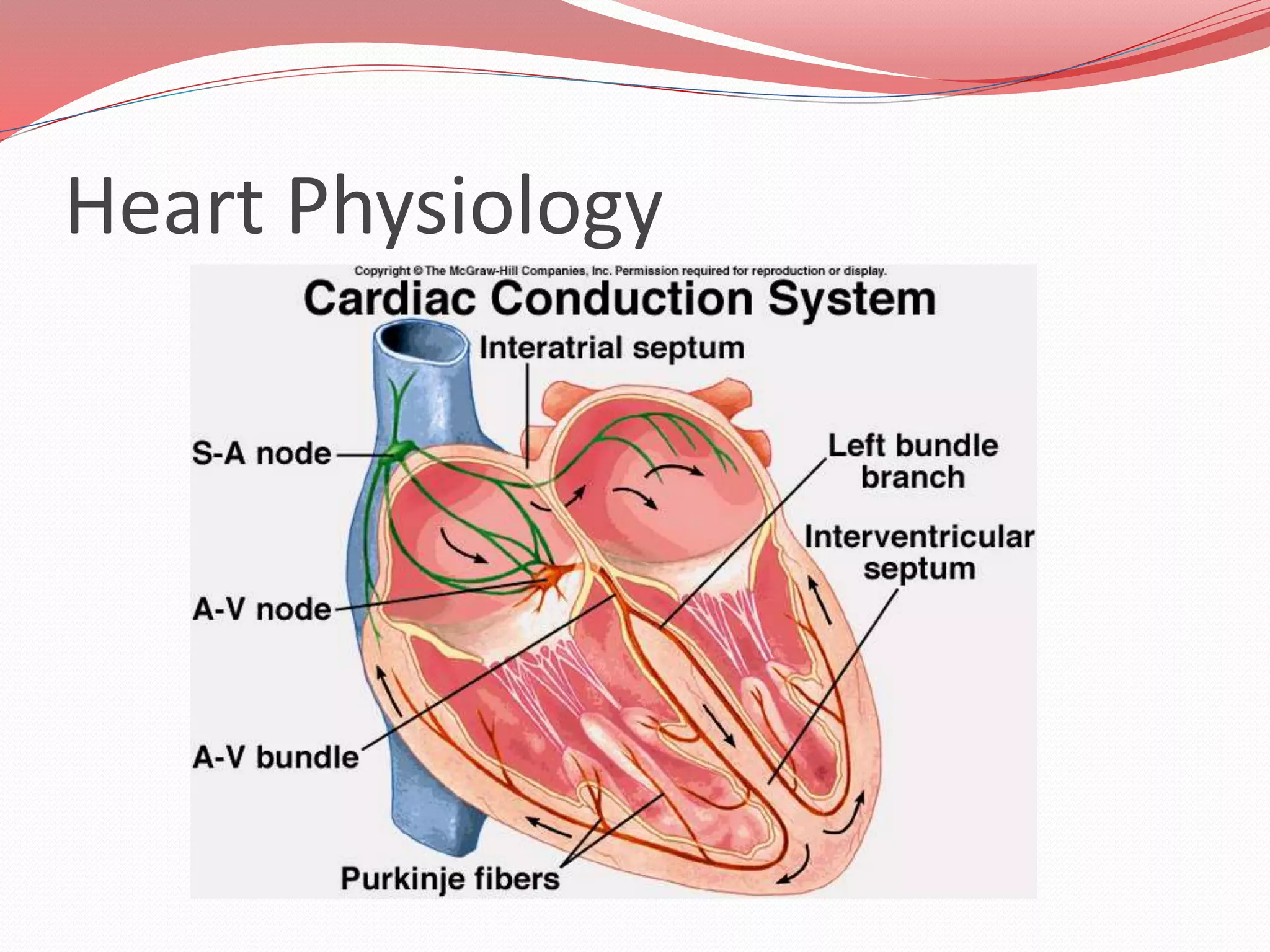
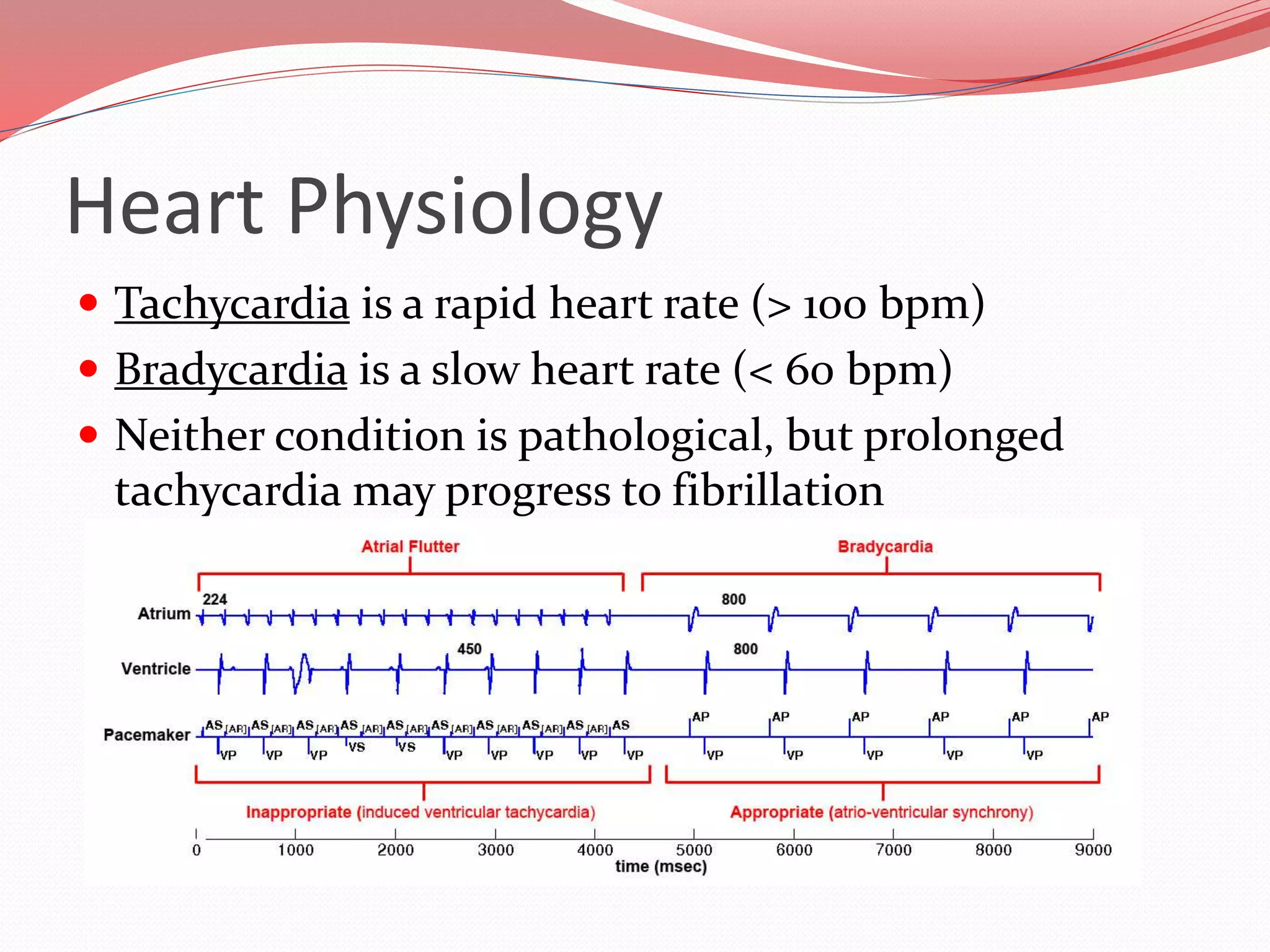
The document discusses the cardiovascular system and heart. It describes how the cardiovascular system transports blood throughout the body using the heart as a pump. It then provides details on the structure and layers of the heart, how it functions as a double pump with two circuits (pulmonary and systemic), and the roles of the heart valves and chambers. It also discusses heart physiology including the conduction system that regulates heartbeat, conditions like tachycardia and fibrillation, and the purpose of pacemakers.