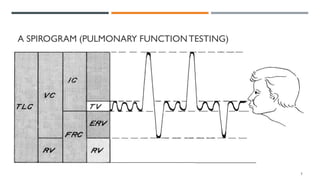
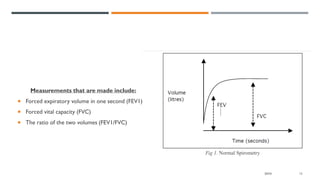
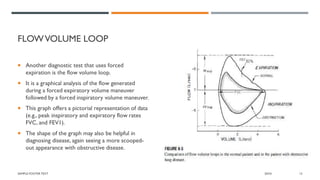
This document provides an overview of pulmonary function tests (PFTs). It discusses the basics of PFTs, including comparing observed results to predicted values and categorizing tests as volumes, flows, or diffusion studies. Specific tests are described, such as spirometry, flow-volume loops, closing volumes, and maximal voluntary ventilation. Lung volumes, capacities, and the components of a spirogram are defined. The document also covers indications, contraindications, and procedures for PFTs.