1. Respiration includes ventilation, gas exchange, and oxygen utilization. Ventilation is the mechanical process of breathing that moves air in and out of the lungs. Gas exchange occurs through diffusion of oxygen and carbon dioxide between the alveoli and blood.
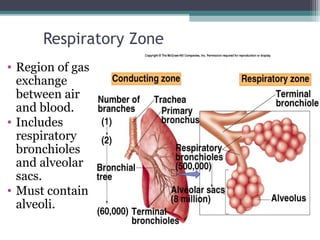
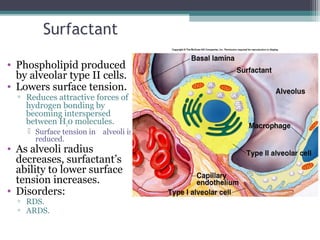
2. The lungs contain over 300 million alveoli which provide a large surface area for gas exchange. Each alveolus is lined by fluid and surfactant that helps reduce surface tension to facilitate breathing.
3. During inspiration, contraction of the diaphragm and intercostal muscles increases the thoracic cavity volume, lowering pressure and drawing air into the lungs. Expiration is passive as the lungs and chest wall recoil, increasing pressure to push


![Ventilation
• Mechanical process that moves
air in and out of the lungs.
• [O2]of air is higher in the lungs
than in the blood, O2 diffuses
from air to the blood.
• C02 moves from the blood to
the air by diffusing down its
concentration gradient.
• Gas exchange occurs entirely
by diffusion:
▫ Diffusion is rapid because of the
large surface area and the small
diffusion distance.
Insert 16.1](https://image.slidesharecdn.com/chp16respiratoryphysiology-151008142007-lva1-app6892/85/Respiratory-physiology-3-320.jpg)

















![Anatomical Dead Space
• Not all of the inspired air reached the alveoli.
• As fresh air is inhaled it is mixed with air in
anatomical dead space.
▫ Conducting zone and alveoli where [02] is lower than
normal and [C02] is higher than normal.
• Alveolar ventilation = F x (TV- DS).
▫ F = frequency (breaths/min.).
▫ TV = tidal volume.
▫ DS = dead space.](https://image.slidesharecdn.com/chp16respiratoryphysiology-151008142007-lva1-app6892/85/Respiratory-physiology-23-320.jpg)





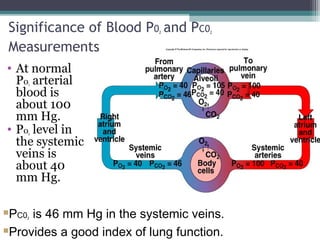
![Partial Pressures of Gases in Blood
• When a liquid or gas (blood and alveolar air)
are at equilibrium:
▫ The amount of gas dissolved in fluid reaches a
maximum value (Henry’s Law).
• Depends upon:
▫ Solubility of gas in the fluid.
▫ Temperature of the fluid.
▫ Partial pressure of the gas.
• [Gas] dissolved in a fluid depends directly on
its partial pressure in the gas mixture.](https://image.slidesharecdn.com/chp16respiratoryphysiology-151008142007-lva1-app6892/85/Respiratory-physiology-29-320.jpg)






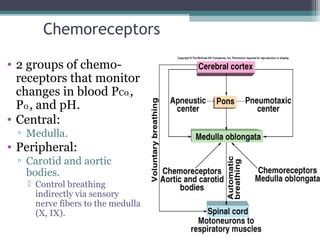


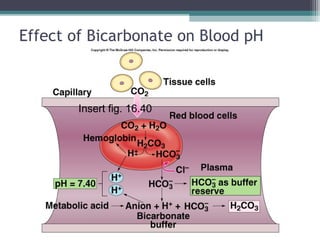
![Chemoreceptor Control (continued)
• Peripheral chemoreceptors:
▫ Are not stimulated directly by changes in arterial
PC02.
• H20 + C02 H2C03 H+
• Stimulated by rise in [H+
] of arterial blood.
▫ Increased [H+
] stimulates peripheral
chemoreceptors.](https://image.slidesharecdn.com/chp16respiratoryphysiology-151008142007-lva1-app6892/85/Respiratory-physiology-42-320.jpg)
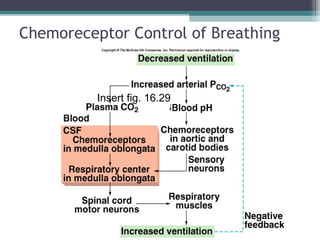

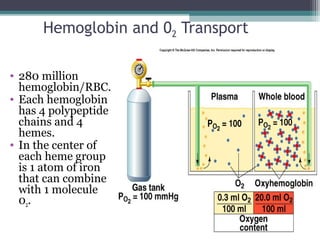


![Hemoglobin (continued)
• Oxygen-carrying capacity of blood determined by
its [hemoglobin].
▫ Anemia:
[Hemoglobin] below normal.
▫ Polycythemia:
[Hemoglobin] above normal.
▫ Hemoglobin production controlled by erythropoietin.
Production stimulated by PC02 delivery to kidneys.
• Loading/unloading depends:
▫ P02 of environment.
▫ Affinity between hemoglobin and 02.](https://image.slidesharecdn.com/chp16respiratoryphysiology-151008142007-lva1-app6892/85/Respiratory-physiology-49-320.jpg)
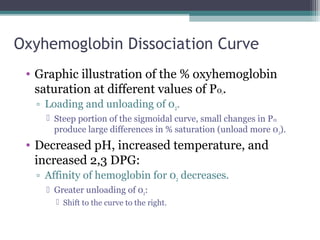
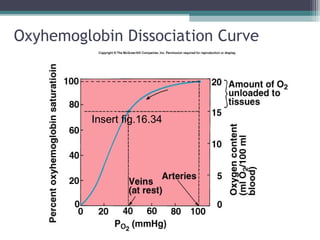
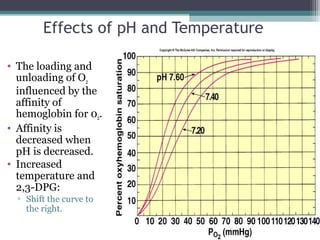
![Effect of 2,3 DPG on 02 Transport
• Anemia:
▫ RBCs total blood [hemoglobin] falls, each RBC
produces greater amount of 2,3 DPG.
Since RBCs lack both nuclei and mitochondria,
produce ATP through anaerobic metabolism.
• Fetal hemoglobin (hemoglobin f):
▫ Has 2 γ-chains in place of the β-chains.
Hemoglobin f cannot bind to 2,3 DPG.
Has a higher affinity for 02.](https://image.slidesharecdn.com/chp16respiratoryphysiology-151008142007-lva1-app6892/85/Respiratory-physiology-53-320.jpg)

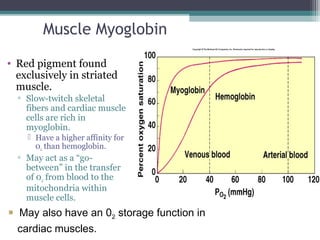
![Chloride Shift at Systemic Capillaries
• H20 + C02 H2C03 H+
+ HC03
-
• At the tissues, C02 diffuses into the RBC; shifts
the reaction to the right.
▫ Increased [HC03
-
] produced in RBC:
HC03
-
diffuses into the blood.
▫ RBC becomes more +.
Cl-
attracted in (Cl-
shift).
▫ H+
released buffered by combining with
deoxyhemoglobin.
• HbC02 formed.
▫ Unloading of 02.](https://image.slidesharecdn.com/chp16respiratoryphysiology-151008142007-lva1-app6892/85/Respiratory-physiology-57-320.jpg)
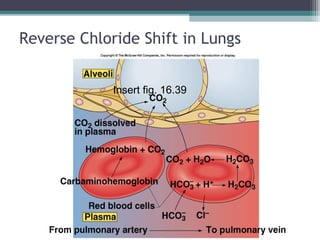
![At Pulmonary Capillaries
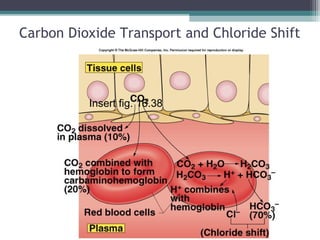
• H20 + C02 H2C03 H+
+ HC03
-
• At the alveoli, C02 diffuses into the alveoli;
reaction shifts to the left.
• Decreased [HC03
-
] in RBC, HC03
-
diffuses into
the RBC.
▫ RBC becomes more -.
Cl-
diffuses out (reverse Cl-
shift).
• Deoxyhemoglobin converted to
oxyhemoglobin.
▫ Has weak affinity for H+
.
• Gives off HbC02.](https://image.slidesharecdn.com/chp16respiratoryphysiology-151008142007-lva1-app6892/85/Respiratory-physiology-59-320.jpg)