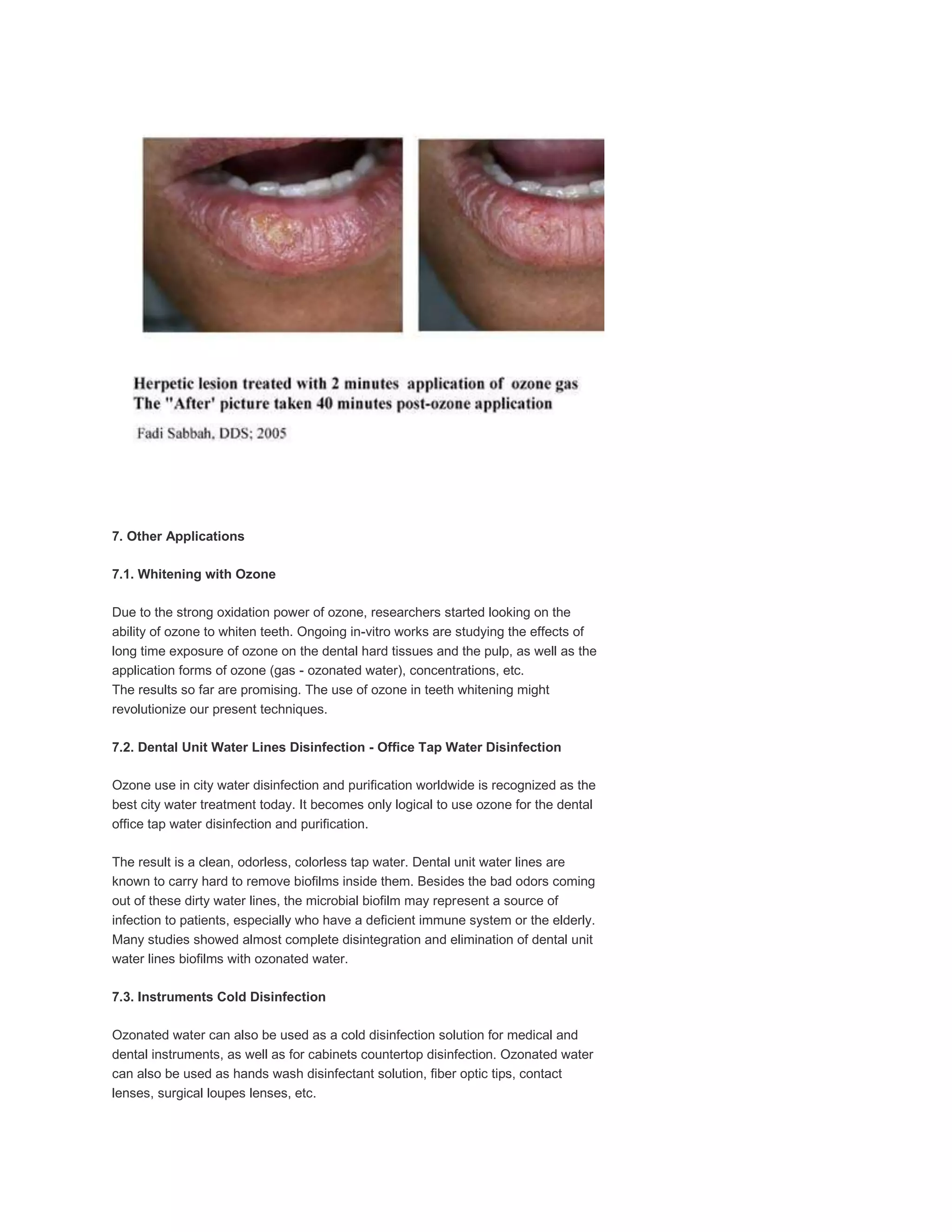
This document discusses the use of ozone therapy in various dental applications and procedures. Some key points:
- Ozone has undisputed disinfectant power and is gaining widespread use in dentistry as an antiseptic and disinfectant.
- Research shows ozone may be able to arrest and reverse early tooth decay lesions without invasive treatment.
- Ozone can be used safely in dental procedures using a handpiece to deliver ozone gas directly to treatment sites.
- Applications discussed include treatment of tooth decay, root canals, gum disease, extractions, implants, crowns and dentures. Ozone shows promise in these areas due to its disinfection properties and ability to reduce bacteria