Lecture 21 adrenal glands diseases - pathology
- 1. 576 Adrenal Glands (Suprarenal Glands) Lecture 21
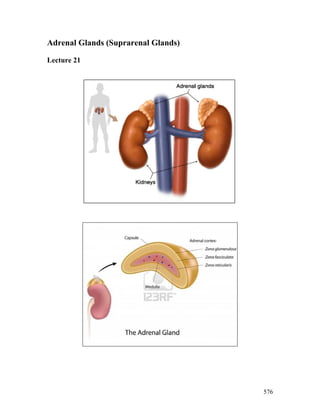
- 2. 577 Anatomy of adrenal glands also known as suprarenal glands their name indicates that position (ad-, "near" or "at" + renes, "kidneys"; and as concerns supra-, meaning "above") located in the retroperitoneum situated 'on' top of the kidneys one on each side Left and right-sided glands; Left gland is crescentic and Right gland is pyramidal in adults; each is 5 x 3 x 1 cm Are composite of two Regions: Adrenal Cortex -outer region Adrenal Medulla-inner region Normal weight 4-6 grams each after dissection of fat Adrenal Cortex The normal adrenal has a golden yellow cortex. This bright yellow reflects the lipid nature of the steroid hormones synthesized by the cortex. During severe stress, the cortex becomes lipid depleted and the normally yellow cortex becomes pale and thinned. The central medulla has a dark brown color. It has complete fibrous capsule, which may merge with capsule of kidney (either gland), and liver (right sided gland) Adrenal Medulla Because the sympathetic nervous system also secretes epinephrine and norepinephrine, adrenal medullary function is not essential for life, but adrenal cortical function is essential for life. They are chiefly responsible for releasing hormones in conjunction with stress through the synthesis of corticosteroids and catecholamines, including cortisol and adrenaline (epinephrine), respectively.
- 3. 578 Adrenal gland-physiology 1) The Adrenal cortex: represent outer portion, comprises 90% of the adrenal gland. synthesizes and secretes corticosteroids (mineralocorticoids, glucocorticoids ) and sex hormones, all derived from cholesterol Subdivided into three zones: 1. Zona glomerulosa (outer): make up 15% of cortex. produces mineralocorticoids (aldosterone-increases sodium and water absorption and potassium secretion) 2. Zona fasciculata (middle): make up 75% of cortex. produces glucocorticoids, some sex hormones 3. Zona reticularis (inner): make up 10% of cortex. produces estrogens and androgens, some glucocorticoids 2) Adrenal medulla: is composed of chromaffin cells which secret catecholamines Hypothalamic-Pituitary-Adrenal axis (HPA axis)
- 4. 579 Adrenal Cortical Function Regulation Hypothalamic corticotropin-releasing hormone (CRH) enters hypophyseal portal system, reaches anterior pituitary gland, stimulates release of ACTH ACTH travels in blood to adrenal cortex, is bound to cortical cell membranes, activates intracytoplasmic cyclases that form cAMP and GMP; both cortisol and ACTH inhibit release of CRH, and cortisol also inhibits secretion of ACTH ACTH normally is secreted episodically, with more and longer episodes in early morning, and nadir in evening; this pattern causes circadian rhythm for cortisol seen in normals Volume changes affect renin-angiotensin system, leading to aldosterone secretion ACTH, potassium ions and aldosterone-stimulating factor also regular aldosterone synthesis. Adrenal Cortical Hormones Production & Transport Adrenocortical cells synthesize and secrete Steroids from Cholesterol. While cholesterol can be synthesized in many body tissues, further differentiation into steroid hormones takes place only in the adrenal cortex and in its embryological cousins, the ovaries and the testes. Cortisol binds largely to corticosteroid binding globulin and to a lesser extent to Albumin. Aldosterone circulates mostly bound to albumin. The main site for metabolism of the adrenal cortical hormones is the liver where they undergo a number of metabolic conversions before being conjugated and made water soluble. They are then eliminated in either urine or bile. Hormones of the adrenal cortex 1) Mineralocorticoids: The mineralocorticoids play an essential role in regulating potassium and sodium levels and water balance. Aldosterone hormone –increases the reabsorption of sodium ions and water and the release (secretion) of potassium in the kidney This increases blood volume and, therefore, increases blood pressure. Drugs that interfere with the secretion or action of aldosterone are in use as antihypertensives. One example is spironolactone, which lowers blood pressure by blocking the aldosterone receptor. Aldosterone secretion is regulated by the rennin-angiotensin mechanism and by blood levels of potassium. levels of aldosterone sodium retention by the distal tubules of the kidney while urinary losses of potassium. At the same time, aldosterone tends to decrease the acidity of body fluids.
- 5. 580 2) Corticosteroid hormones: Hydrocortisone hormone (Cortisol) Corticosterone Cortisol (Hydrocortisone hormone) 1. Cortisol (hydrocortisone) is the major human glucocorticoid. 2. It also serves as a mineralocorticoid but is considerably less effective than aldosterone. 3. Metabolic Effects of Cortisol: stimulates glucose production by the liver ( Increase Blood Sugar) promotes protein breakdown causes mobilization of fatty acids It suppresses the immune system by "muting" the white blood cells It decreases bone formation. As body proteins are broken down, amino acids are mobilized and transported to the liver, where they are used in the production of glucose (gluconeogenesis). Mobilization of fatty acids converts cell metabolism from the use of glucose for energy to the use of fatty acids. As glucose production by the liver increases and peripheral glucose use decreases, a moderate resistance to insulin develops. In persons with diabetes and those who are diabetes prone, this has the effect of raising the blood glucose level. 4. Cortisol, along with more potent and longer-acting synthetic derivatives like prednisone, methylprednisolone, and dexamethasone exerts powerful anti- inflammatory effects (Treatment of rheumatoid arthritis, disseminated lupus erythematosus, and multiple sclerosis.) 5. If, however, the inflammation has a bacterial or viral origin, the steroids may do more harm than good because the spread of the infection is facilitated while the signs of inflammation are masked. 6. Finally, corticosteroids in large doses impair the functioning of the immune system so that the production of harmful antibodies, such as those produced in allergic diseases, may be suppressed. 7. It is important to note that these beneficial effects are offset by serious side effects of large-dose, long-term corticosteroid therapy, effects that closely mimic many of the symptoms of Cushing's syndrome. 8. Chronic suppression causes atrophy of the adrenal gland, and the : o abrupt withdrawal of drugs can cause acute adrenal insufficiency. o Recovery to a state of Normal adrenal function may be prolonged, requiring 12 months or more.
- 6. 581 3) Adrenal androgens: 1. Adrenal androgens are not as potent as testosterone, the major steroid secreted by the testis, but a number of them, including androstenedione, dehydroepiandrosterone (DHEA), and its sulfate (DHEAS) may be converted to stronger androgens such as testosterone. 2. These sex hormones probably exert little effect on normal sexual function. Contribute to the pubertal growth of body hair, particularly pubic and axillary hair in women. Tests of Adrenal Function Blood levels of cortisol, aldosterone, and ACTH can be measured using immunoassay methods. A 24 hour urine specimen measures the excretion of 17 ketosteroids, 17 ketogenic steroids, and 17 hydroxycorticosteroids. Theses metabolic end- products of the adrenal hormones and the male androgens provide information about alterations in the biosynthesis of the adrenal cortical hormones. The 24 hour urinary free cortisol is an excellent screening test for Cushing’s syndrome. Suppression and stimulation tests afford a means of assessing the state of the HPA feedback system. For example, a test dose of ACTH can be given to assess the response of the adrenal cortex to stimulation. Similarly, administration of dexamethasone, a synthetic glucocorticoid drug, provides a means of measuring negative feedback suppression of ACTH. Adrenal Medulla Catecholamines stored in large vesicles within chromaffin cells of the adrenal medulla The functional unit of the adrenal medulla is the chromaffin cell, which functions as a neuroendocrine cell. In response to stimulation, chromaffin cells secrete the hormones epinephrine (adrenaline 80%) and norepinephrine (noradrenalin 20%) directly into the blood The medulla is involved in extreme stress and, within this context, epinephrine and norepinephrine both work with cortisol from the adrenal cortex. Epinephrine and norepinephrine are important mainly in crisis situations. Catecholamines Biosynthesis : 1. Tyrosine is precursor for the synthesis of catecholamines. 2. The catecholamine are produced in response to fight, fright and flight (3F). These include emergencies like shock, cold, fatigue, emotional condition like anger.
- 7. 582 Fight or Flight Response When a woman sees the snake, she becomes afraid and an alarm button in her body is pushed. Her brain sends a lightening-fast command to her adrenal glands. Hormones of the adrenal Medulla
- 8. 583 Function of Cortisol in Stress Corticosteroids withdrawal syndrome Steroid withdrawal syndrome, or rebound effect is the body's exaggerated response to removal of the drug. It can occur if corticosteroid drugs are not discontinued gradually. Tapering the drug gives the adrenal glands time to return to their normal patterns of secretion and thus minimizes corticosteroid withdrawal symptoms. Withdrawal symptoms are: (weakness, fatigue, decreased appetite, weight loss, nausea, vomiting, diarrhea, abdominal pain) can mimic many other medical problems. Another possible complication to stopping steroids too quickly can result in adrenal crisis (a life-threatening state caused by insufficient levels of cortisol).
- 9. 584 Glucocorticoid effects on immune cells Summary of Adrenocortical Hormones Function
- 10. 585 Adrenal Cortex Disorders Adrenal Cortical Insufficiency: I. Acute Adrenal Cortical Insufficiency Waterhouse-Friderichsen syndrome It is adrenal gland failure due to bleeding into the adrenal gland. It is caused by severe bacterial infection (most commonly the meningococcus (Neisseria meningitidis) which invades the blood stream. It is characterized by acute adrenal gland insufficiency and profound shock. It is fatal if not treated immediately. Bleeding into the skin (petechiae and purpura) usually occurs and the tissue may die (become necrotic or gangrenous). If the patient survives, the areas heal with scarring. Treatment of shock, toxemia and bacteremia and the administration of adrenocortical hormone substitution therapy.
- 11. 586 II. Chronic Adrenal Cortical Insufficiency: Primary adrenocortical insufficiency or Addison’s disease is caused by destruction of the adrenal gland. Secondary adrenocortical insufficiency due to: ACTH deficiency is most commonly a result of exogenous glucocorticoid therapy. Pituitary or hypothalamic tumors are the most common causes of naturally occurring pituitary ACTH hyposecretion. Secondary adrenal insufficiency is usually chronic, and the manifestations may be nonspecific. However, acute crisis can occur in undiagnosed patients or in corticosteroid-treated patients who do not receive increased steroid dosage during periods of stress. The clinical features of secondary adrenal insufficiency differ from those of primary adrenocortical insufficiency in that: o Pituitary secretion of ACTH is deficient and hyperpigmentation is therefore not present. o In addition, mineralocorticoid secretion is usually normal. Thus, the clinical features of ACTH and glucocorticoid deficiency are nonspecific.
- 12. 587 Primary Adrenal Cortical insufficiency: Addison’s disease In 1855, Thomas Addison, an English physician, provided the first detailed clinical description of primary adrenal insufficiency. in which adrenal cortical hormones and ACTH because of lack of feedback inhibition. It is a relatively rare disorder in which all the layers of the adrenal cortex are destroyed. Addison’s disease, like type 1 diabetes mellitus, is a chronic metabolic disorder that requires lifetime hormone replacement therapy. The adrenal cortex has a large reserve capacity, and the manifestations of adrenal insufficiency usually do not become apparent until approximately 90% of the gland has been destroyed.
- 13. 588 Causes of Addison’s disease: o Autoimmune destruction is the most common cause o Before 1950, tuberculosis was the major cause o Rare causes include metastatic carcinoma, fungal infection (particularly histoplasmosis), cytomegalovirus infection, amyloid disease, and hemochromatosis. o Bilateral adrenal hemorrhage may occur in persons taking anticoagulants, during open heart surgery, and during birth or major trauma. o Acquired immunodeficiency syndrome (AIDS), in which the adrenal gland is destroyed by a variety of opportunistic infectious agents. o Addison’s disease, like type 1 diabetes mellitus, is a chronic metabolic disorder that requires lifetime hormone replacement therapy. Pathophysiology of Addison’s disease: related primarily to 1) Mineralocorticoid deficiency, 2) Glucocorticoid deficiency, 3) Hyperpigmentation. Mineralocorticoid deficiency Causes urinary losses of sodium, chloride, and water, along with excretion of potassium. The result is hyponatremia, loss of extracellular fluid, cardiac output, and hyperkalemia. There may be an abnormal appetite for salt. Orthostatic hypotension is common. Dehydration, weakness, and fatigue are common early symptoms. If loss of sodium and water is extreme cardiovascular collapse and shock. Glucocorticoid deficiency Glucocorticoid deficiency contributes to hypotension and causes severe insulin sensitivity and disturbances in carbohydrate, fat, and protein metabolism. In the absence of cortisol, insufficient carbohydrate is formed from protein; hypoglycemia and diminished liver glycogen result. Weakness follows, due in part to deficient neuromuscular function. Resistance to infection, trauma, and other stress is diminished. Myocardial weakness and dehydration reduce cardiac output, and circulatory failure can occur.
- 14. 589 Hyperpigmentation Decreased blood cortisol results in increased pituitary ACTH production and increased blood β-lipotropin, which has melanocyte-stimulating activity and, together with ACTH, causes the hyperpigmentation of skin and mucous membranes characteristic of Addison's disease. Thus, adrenal insufficiency secondary to pituitary failure does not cause hyperpigmentation. The skin looks bronzed or suntanned in exposed and unexposed areas, and the normal creases and pressure points tend to become especially dark. The gums and oral mucous membranes may become bluish-black. Hyperpigmentation occurs in more than 90% of persons with Addison’s disease β-lipotropin a prohormone synthesized by cells of the adenohypophysis; it promotes fat mobilization and skin darkening by stimulation of melanocytes and is the precursor of the endorphins. Patient with Addison's
- 15. 590 Diagnosis of Chronic Adrenal Cortical Insufficiency
- 16. 591 Treatment of Addison’s disease: oral replacement therapy, with higher doses being given during periods of stress. The pharmacologic agent that is used should have both glucocorticoid and mineralocorticoid activity. Mineralocorticoids are needed only in primary adrenal insufficiency. Hydrocortisone usually is the drug of choice. In mild cases, hydrocortisone alone may be adequate. Because persons with the disorder are likely to have episodes of hyponatremia and hypoglycemia, they need to have a regular schedule for meals and exercise. Persons with Addison’s disease also have limited ability to respond to infections, trauma, and other stresses. Such situations require immediate medical attention and treatment. All persons with Addison’s disease should be advised to wear a medical alert bracelet or medal.
- 17. 592 Cushing’s syndrome Pathophysiology Cushing's syndrome refers to excess cortisol of any etiology. One of the most common causes of Cushing's syndrome is a cortisol secreting adenoma in the cortex of the adrenal gland (Adrenal form). The adenoma causes cortisol levels in the blood to be very high, and negative feedback on the pituitary from the high cortisol levels causes ACTH levels to be very low. Cushing's disease refers only to hypercortisolism secondary to excess production of ACTH from a pituitary gland adenoma (Pituitary form). This causes the blood ACTH levels to be elevated along with cortisol from the adrenal gland. The ACTH levels remain high because a tumor causes the pituitary to be unresponsive to negative feedback from high cortisol levels. Ectopic Cushing’s form: Caused by a nonpituitary ACTH- secreting tumor. o Certain extrapituitary malignant tumors such as small cell carcinoma of the lung may secrete ACTH or rarely CRH and produce Cushing’s syndrome. o Cushing’s syndrome also can result from long-term therapy with one of the potent pharmacologic preparations of glucocorticoids; this form is called iatrogintic Cushing’s syndrome.
- 18. 593 Cushing’s syndrome forms Manifestations of Cushing’s syndrome: Represent an exaggeration of the many actions of cortisol. Altered fat metabolism causes a peculiar deposition of fat characterized by a protruding abdomen; subclavicular fat pads or “buffalo hump” on the back; and a round, plethoric “ moon face” There is muscle weakness, and the extremities are thin because of protein breakdown and muscle wasting. In advances cases, the skin over the forearms and legs becomes thin, having the appearance of parchment. Purple striae, or stretch marks, from stretching of the catabolically weakened skin and subcutaneous tissues are distributed over the breast, thighs, and abdomen.
- 19. 594 Osteoporosis may develop because of destruction of bone proteins and alterations in calcium metabolism, resulting in back pain, compression factures of the vertebrae, and rib fractures. As calcium is mobilized from bone, renal calculi may develop. Derangements in glucose metabolism are found in approximately 75% of patients, with clinically overt diabetes mellitus occurring in approximately 20%. The glucocorticoids possess mineralocorticoid properties; this causes hypokalemia as a result of excessive potassium excretion and hypertension resulting from sodium retention. Inflammatory and immune responses are inhibited, resulting in increased susceptibility to infection. Cortisol increase gastric acid secretion, which may provoke gastric ulceration and bleeding. An accompanying increase in androgen levels causes hirsutism, mild acne, and menstrual irregularities in women. Excess levels of the glucocorticoids may give rise to extreme emotional liability, ranging from mild euphoria and absence of normal fatigue to grossly psychotic behavior. Cushing’s syndrome Manifestations Summary Circadian Rhythm of Cortisol Secretion It is factor which influences cortisol secretion. This circadian, or diurnal, rhythm: is the cyclic release of cortisol occurring throughout a 24-hr period as a result of intrinsic endocrine function. o Minimal secretion of cortisol occurs just before and in the initial hours of sleep; o Maximal secretion of cortisol occurs just before and in the initial hours of wakefulness. o During the rest of the day; intermittent secretion of cortisol occur.
- 20. 595 Diagnosis of Cushing’s syndrome: Laboratory Tests Cortisol levels rise and fall during the day. Highest levels occur at about 6 to 8 a.m. and lowest levels at about midnight. One of the prominent features of Cushing’s syndrome is loss of the diurnal pattern of cortisol secretion. 1) 24-hour Urine Cortisol (or UFC urine free cortisol) Urinary free cortisol is a measurement of the cortisol in the urine that is not attached to other substances. Free cortisol represents the active form of the hormone. The urine measurement directly reflects the blood level of cortisol ( 24- hour UFC associated with Plasma Cortisol) The normal range is 10 to 100 mcg/24 h. 2) Cortisol level Cortisol levels are often measured to evaluate the pituitary and adrenal function. Measuring cortisol at 11 PM, when normally levels are at their lowest. This can be done on saliva or in the blood. If these tests indicate that cortisol levels are not varying normally and are consistently high, other testing is done to determine the reason for the increased levels. Normal values in serum at 8 a.m.are 6 to 23 mcg/dl.
- 21. 596 3) Dexamethasone Suppression Test Dexamethasone is a synthetic steroid similar to cortisol, which suppresses ACTH secretion in normal people. Thus Dexamethasone suppression test measures the response of the adrenal glands to ACTH. A normal response to dexamethasone is suppression of cortisol secretion. If there is not a normal response on the low-dose test, abnormal secretion of cortisol is likely (Cushing's Syndrome).. MRI or CT scans afford a means for location adrenal or pituitary tumors. Treatment of Cushing’s syndrome: Untreated, Cushing’s syndrome produces serious morbidity and even death. The goal of treatment for Cushing’s syndrome is to remove or correct the source of hypercortisolism without causing any permanent pituitary or adrenal damage. Transsphenoidal removal of a pituitary adenoma or a hemihypohysectomy is the preferred method of treatment. This allows removal of only the tumor, rather than the entire pituitary gland. After successful removal, the person must receive cortisol replacement therapy for 6 to 12 months or until adrenal function returns . Patients also may receive pituitary radiation therapy, but the full effects of treatment may not be realized for 3 to 12 months. Summary of Cushing’s syndrome:
- 22. 597 Cushing’s syndrome Cushing’s syndrome (Manifestations) • Striae on the leg • Axillary and lower abdominal Striae
- 23. 598 Cushing’s syndrome (Manifestations) • Buffalo Hump( lump of fat on the back of the neck) • Moon face; Puffy face; Facial edema(round, red, and full)
- 24. 599
- 25. 600 Disorders of Pituitary Gland Disorders of the anterior pituitary gland Alterations of growth hormone secretion Growth hormone is a polypeptide that is synthesized and secreted by the acidophilic cells of the anterior pituitary gland. Growth hormone stimulates the growth of cartilage, long bones, muscle and organs during childhood development. Growth hormone hyposecretion In children and adolescents, GH secretion occurs in a pulsatile fashion at night and during sleep. Daytime levels of GH are very low and not indicative of overall GH release. Causes: o congenital defect o acquired as a result of injury or tumor growth. o seen in congenital conditions such as Turner syndrome and Down syndrome. o idiopathic. Manifestations o In children: short stature (dwarfism). o In adults: Muscle weakness and obesity. Treatment: GH replacement therapy To evaluate GH secretion in a particular patient it is important to take samples throughout a 24-hour period.
- 26. 601 Turner syndrome (also called X0 syndrome) is a a condition in which a female is partly or completely missing an X chromosome of their two X chromosome copies; they have a total of 45 chromosomes including one X chromosome (45,X), instead of the usual two copies (46,XX) Signs and symptoms: short and webbed neck, low-set ears, low hairline at the back of the neck, short stature, and swollen hands and feet are seen at birth. Typically they are without menstrual periods. Infertility and heart defects. Down's syndrome (trisomy 21), is a genetic disorder caused by the presence of all or part of a third copy of chromosome 21. Signs & symptoms : physical growth delays, characteristic facial features, and mild to moderate intellectual disability. Growth hormone hypersecretion 1-Gigantismresults from the excess production of GH before fusion of the epiphyseal plates of the long bones (around puberty). o Manifestations: Extremely tall stature due to excessive growth of the long bones. 2- Acromegaly GH excess occurs after fusion of the epiphyseal plates of the long bones. o Manifestations: o Overgrowth of connective tissues , o Bones grow more in width than in length patients presented with thickening and deformation of the hands, face, skull and feet. o Patients also tend to have very oily skin. o Central nervous system disturbances (headache, vision changes) and abnormalities may occur. o Cardiovascular disease in the form of hypertension and coronary artery disease represents a significant source of mortality in these patients. Treatment o Surgical removal of tumor. o Radiation therapy of the tumor if surgery is not feasible.
- 27. 602 Disorders of the posterior pituitary A- Syndrome of inappropriate ADH (SIADH) (Increased Production of ADH) Caused by pituitary tumors or injury or transiently due to physiologic stress. Manifestations o Excessive fluid retention o Generalized edema (Weight gain). o Increased in serum sodium level. Treatment o Fluid restriction. o Diuretics. o Removal of tumor if present
- 28. 603 B-Diabetes insipidus (Decreased production of ADH) Etiology: Decreased ADH is due to defects in the hypothalamus/ pituitary axis or from a tumor or trauma. Manifestations o Polyuria: Excessive production of very dilute urine. o Polydipsia: Excessive thirst. o Dehydration: Increased plasma osmolarity. o Hypotension and reflex tachycardia. Treatment o Administration of ADH and ADH analogues like lypressin and desmopressin o ADH itself is administered by S.C. or I.M. injection, whereas lypressin and desmopressin are administered as an intranasal spray. o An oral form of desmopressin is also now available.
