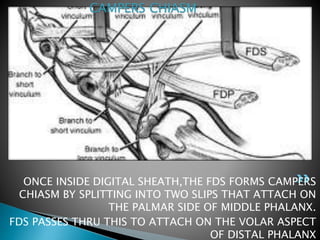
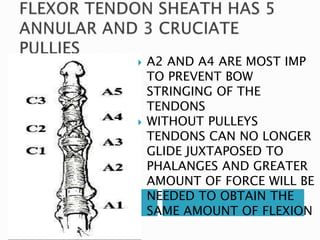
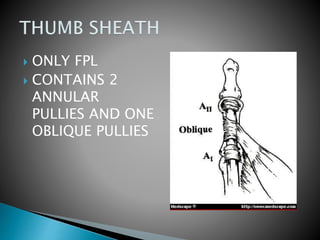
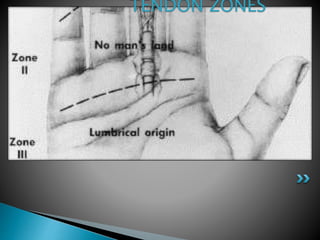
This document discusses flexor tendon injuries and repairs in the hand. It covers tendon anatomy, zones of injury, types of repairs, and postoperative rehabilitation protocols. Flexor tendon injuries most commonly occur in males aged 15-30 years old. There are two main postoperative protocols - passive flexion protocol with splinting for 6-9 weeks or early active tension protocol with splinting for 4 weeks and early active exercises. Precise surgical technique and strict adherence to rehabilitation are needed for successful results.