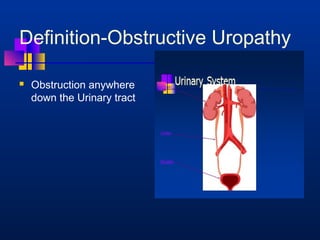
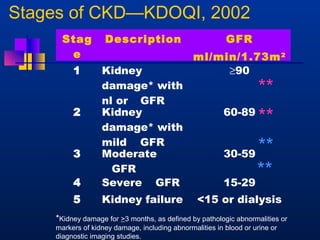
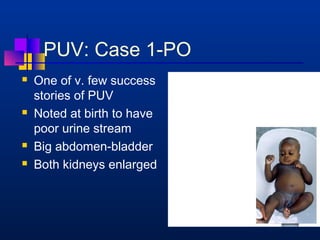
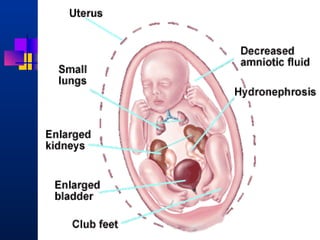
This document provides an overview of chronic kidney disease (CKD) and obstructive uropathy. It defines CKD and obstructive uropathy, discusses the stages of CKD, and outlines the mechanisms by which obstructions can lead to CKD, including both mechanical and non-mechanical obstructions. Specific conditions that can cause obstructions are presented such as posterior urethral valves. Management approaches including surgical and medical treatments are discussed, with an emphasis on long-term monitoring and care to preserve renal function and slow CKD progression.