This document summarizes recent advances in understanding the structure and function of the wrist. It describes the anatomy of carpal bones and ligaments. The proximal row includes the scaphoid, lunate, and triquetrum bones connected by strong interosseous ligaments. The distal row includes the trapezium, trapezoid, capitate, and hamate bones. Motion occurs at both the mid-carpal joint between rows and the radiocarpal joint. The row theory, not column theory, best explains wrist kinematics. Ligament strength testing showed interosseous ligaments are stronger than capsular ligaments.







![486 L. K. RUBY
THE JOURNAL. OF BONE AND JOINT SURGERY
pathological anatomy of the wrist. Nonetheless. our with a critical review of the standard radiographs. sup-
knowledge is incomplete. so theme still is room for di- plemented by additional studies as indicated, allow the
vemsity of opinion regarding the diagnosis and treatment astute clinician to identify specific patterns of instability
of most of the presently recognized wrist instabilities. and to formulate an effective treatment program for the
A careful history and physical examination combined patient.
References
I . Berger, R. A., and Landsmeer, J. M. E.: ihe palmar radiocarpal ligaments: a study of adult and fetal human wrist joints. ]. I/and Sung..
ISA: 847-854. 1990.
2. Botte, M. J.; Cooney, W. P.; and Linscheid. R. L.: Arthroscopy of the wrist: anatomy and technique.]. Hand Sung.. 14A: 313-316, 1989.
3. Coone W. P., III; Linscheid, R. L.; and Dobyns, J. H.: Carpal instability: treatment of ligament injuries of the wrist. In Instructional
Coin.se Lectures, The A,nenican Acade,n of Ont/zopuedic Surgeons. Vol. 41, pp. 33-44. Park Ridge. Illinois. The American Academy of
tI)rthopaedic Surgeons. 1992.
4. Cooney, W. P., III; Garcia-Elias, M.; Dobyns, J. H.; and Linscheid, R. L.: Anatomy and mechanics of carpal instability. Sung. Rounds
Onthop., 9: 15-24. 1989.
5. Destot, E. A. J.: Injuries oft/u’ Wrist: a Radiological Studs’. London, Ernest Benn, 1925.
6. Dobyns, J. H.; Linscheid, R. L.; Macksoud, W. S.; and Siegert, J. J.: Carpal instability. nondissociative. Read at the Annual Meeting of
The American Academy of Orthopaedic Surgeons. San Francisco, California, Jan. 24, 1987.
7. Fisk, C. R.: Carpal instability and the fractured scaphoid. Ann. Ro% Co/I. Sung., 46: 63-76. 1970.
8. Gifford, W. W.; Bolton, R. H.; and Lambrinudi, C.: The mechanism of the wrist area with special reference to fractures of the scaphoid.
I/osp. Rep.. 92: 52-59. 1943.
9. Heck, C. V.; Hendryson, I. E.; and Carter, R. R.: Joint Motion: Method of Measuring and Recording. p. 14. Chicago. The American
Academy of Orthopaedic Surgeons. 1965.
10. Hixson, M. L., and Stewart, C.: Microvascular anatomy of the radioscapholunate ligament of the wrist. ]. I/and Sung., iSA: 279-
282. 199().
1 1 . Horn, S., and Ruby, L. K.: Attempted scapholunate arthrodesis for chronic scapholunate dissociation. ]. I/and Surg.. 16A: 334-339. 1991.
12. Horii, E.; Carcia-Elias, M.; An, K. N.; Bishop, A. T.; Cooney, W. P.; Linscheid, R. L.; and Chao, E. Y. S.: Effect on force transmission
across the carpus in procedures used to treat Kienh#{246}ck’s disease. ]. Hand Sung.. 15A: 393-4(X). 1990.
13. Horii, E.; Garcia-Elias, M.; An, K. N.; Bishop, A. T.; Cooney, W. P.; Linscheid, R. L.; and Chao, E. Y. S.: A kinematic study of
luno-triquetral dissociations.]. Ha,ul Sung.. l6A: 355-362. 1991.
14. Johnson, R. P., and Carrera, G. F.: Chronic capitolunate instability. ]. Bone and Joint Sung., 68-A: 1164-1 176. Oct. 1986.
I S. Lavernia, C. J.; Cohen, M. S.; and Taleisnik, J.: Treatment of scapholunate dissociation by ligamentous repair and capsulodesis. ]. hand
Sung., 17A:3S4-359. 1992.
16. Lichtrnan, D. M.; Schneider, J. R.; Swafford, A. R.; and Mack, G. R.: Ulnar midcarpal instability - clinical and laboratory analysis.
]. hlandSung.. 6:515-523, 1981.
17. Linscheid, R. L.,and Dobyns,J. H.: Carpal instability. Curn. Onthop., 3: 106-114, 1989.
18. Linscheid, R. L.; Dobyns, J. H.; Beabout, J. W.; and Bryan, R. S.: Traumatic instability of the wrist: diagnosis. classification. and
pathomechanics.]. Bone out/Joint Sung.. 54-A: 1612-1632. Dec. 1972.
I 9. Logan, S. E.; Nowak, M. D.; Gould, P. L.; and Weeks, P. NI.: Biomechanical behavior of the scapholunate ligament. Biomed. Sci.
I,istnuni., 22: 81-85. 1986.
20. McMurtry, R. Y.; Youm, V.; Flatt, A. E.; and Gillespie, T. E.: Kinematics of the wrist. II. Clinical applications. ]. Bone and Joint Sung..
60-A: 955-961. Oct. 1978.
2 1. Mayfield, J. K.; Johnson, R. P.; and Kilcoyne, R. F.: The ligaments of the human wrist and their functional significance. Anat. Rec., I 86:
417-428. 1976.
22. MikIc, Z. I). J.: Arthrography of the wrist joint: an experimental study.]. Bone andfoint Sung.. 66-A: 371-378. March 1984.
23. Munk, P. L.; Vellet, A. D.; Levin, M. F.; Steinbach, L. S.; and Helms, C. A.: Current status of magnetic resonance imaging of the wrist.
Ca,iwlian Ass,z. Radiol. .1., 43: 8- 18, 1992.
24. Navarro, A.: Aizales de In.stitute (IC Clinica Quimgica v Ciungia Experimental. Montevideo, Imprenta Artistica de Dornaleche Hnos. 1935.
25. Palmer, A. K., and Werner, F. W.: Biomechanics of the distal radioulnarjoint. C/in. Orthop.. 187: 26-35. 1984.
26. Pisano, S. M.; Peirner, C. A.; Wheeler, D. R.; and Sherwin, F.: Scaphocapitate intercarpal arthrodesis.J. Hauid Sung., l6A: 328-333. 1991.
27. Reagan. D. S.; Linscheid, R. L.; and Dobyns, J. H.: Lunotriquetral sprains. ]. Hand Sung., 9A: 502-514. 1984.
28. Roth, J. H., and Haddad, R. G.: Radiocarpal arthroscopy and arthrography in the diagnosis of ulnar wrist pain. Anthnoscopv. 2:
234-243. 1986.
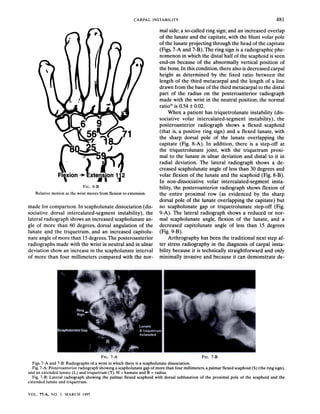
29. Ruby, L. K.; Cooney, W. P.. III; An, K. N.; Linscheid, R. L.; and Chao, E. Y. S.: Relative motion of selected carpal hones: a kinematic
analysis of the normal wrist.]. bland Sung.. 13A: 1-10. 1988.
30. Sarrafian, S. K.; Melarned, J. L.; and Goshgarian, G. M.: Study of wrist motion in flexion and extension. (‘lii,. On/top., 126: 153-159. 1977.
3 1 . Stanley, J. K., and Trail, I. A.: Carpal instability. ]. Bone (111(1 Joint Sung., 76-B(S): 691-7(X), 1994.
32. Taleisnik,J.:The ligamentsofthe wrist.]. hlandSung.. 1: 110-118. 1976.
33. Taleisnik, J., and Watson, H. K.: Midcarpal instability caused by malunited fractures of the distal radius. ]. bland Sung., 9A: 350-
357. 1984.
34. Trurnble, T.; Glisson, R. R.; Seaber, A. V.; and Urbaniak, J. R.: A biomechanical comparison of the methods for treating Kienb#{246}ck’s
disease. ]. bland Sung.. I I A: 88-93. 1986.
35. Trumble, T.; Glisson, R. R.; Seaber, A. V.; and Urbaniak, J. R.: Forearm force transmission after surgical treatment of distal radioulnar
joint disorders.]. 11(1,1(1 Sung., 12A: 196-202, 1987.
36. Viegas. S. F.; Patterson, R.; Peterson, P.; Roefs, J.; Tencer, A.; and Choi, S.: The effects of various load paths and different loads on the
load transfer characteristics of the wrist. ]. hand Sung., 14A: 458-465, 1989.](https://image.slidesharecdn.com/carpalinstability-140313053406-phpapp02/85/Carpal-instability-11-320.jpg)
![CARPAL INSTABILITY 487
37. Viegas, S. F.; Patterson, R. M.; Peterson, P. D.; Pogue, D. J.; Jenkins, D. K.; Sweo, T. D.; and Hokanson, J. A.: Ulnar-sided perilunate
instability: an anatomic and hiomechanic study.]. Hand Sung., iSA: 268-278, 1990.
38. Viegas, S. F.; Tencer, A. F.; Cantrell, J.; Chang, M.; Clegg, R.; Hicks, C.; O’Meara, C.; and Williamson, J. B.: Load transfer characteristics
of the wrist. Part I. The normal joint.]. Hand Sung.. 12A: 971-978. 1987.
39. Watson. H. K., and Ballet, F. L.: The SLAC wrist: scapholunate advanced collapse pattern of degenerative arthritis. ]. bland Sung.. 9A:
358-365. 1984.
40. Watson, H. K.; Ashmead, D., IV; and Makhlouf, M. V.: Examination ofthe scaphoid.]. bland Sting., 13A: 657-660. 1988.
41. Watson, H. K.; Ottani, L.; Pitts, E. C.; and Handal, A. G.: Rotary subluxation of the scaphoid: a spectrum of instability. ]. hand Sting.,
18-B: 62-64, 1993.
42. Weber, E. R.: Concepts governing the rotational shift of the intercalated segment of the carpus. Ontliop. C/in. North A,nenica. 15:
193-207. 1984.
43. Weil, C.. and Rub L. K.: The dorsal approach to the wrist revisited.]. Hand Sung., I IA: 91 1-912. 1986.
44. Zinberg. E. M.: Coren, A. B.; Levinsohn, E. M.; and Palmer, A. K.: The triple injection wrist arthrogram labstract]. ]. biwul Sung.. 13A:
308. 1988.
Vol.. 77-A. NO. 3. MARCEl 995](https://image.slidesharecdn.com/carpalinstability-140313053406-phpapp02/85/Carpal-instability-12-320.jpg)