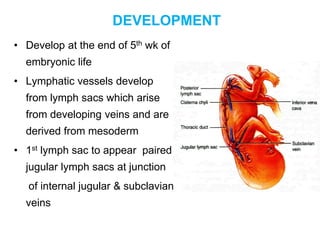
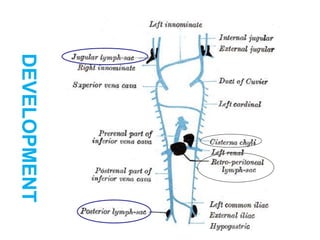
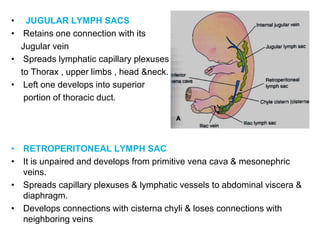
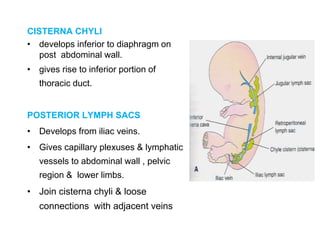
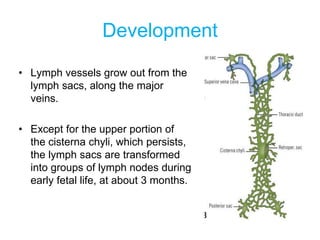
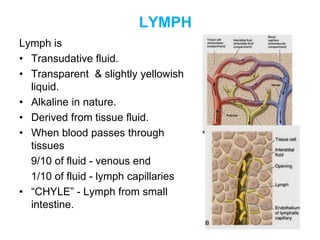
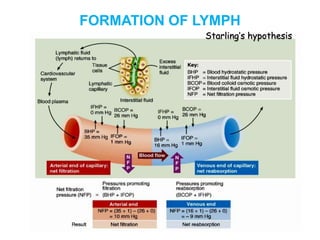
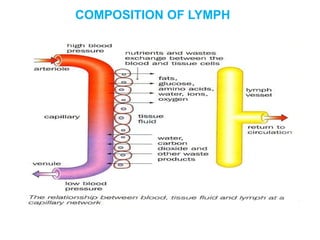
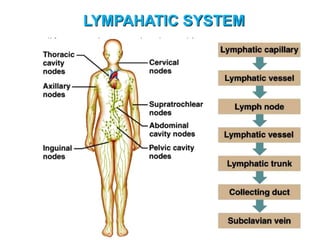
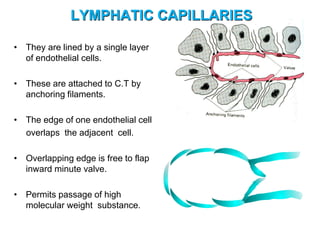
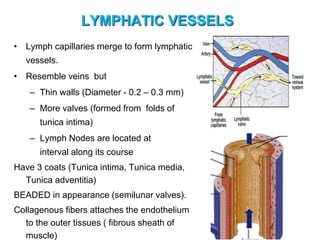
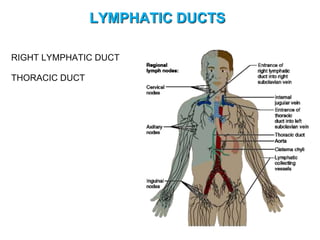
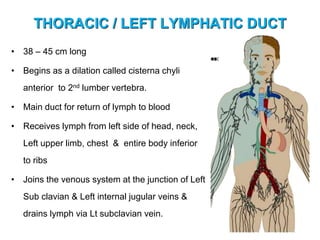
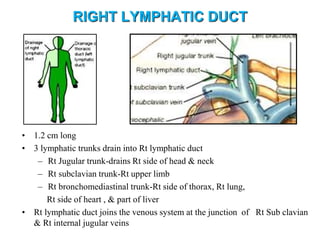
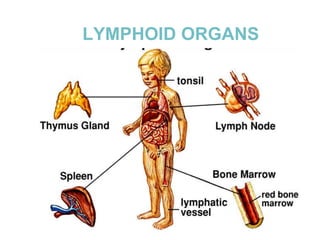
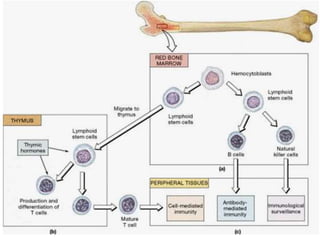
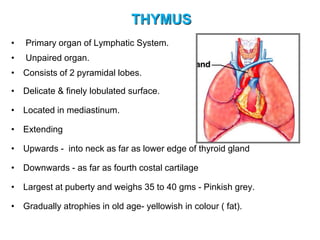
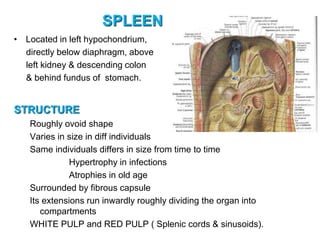
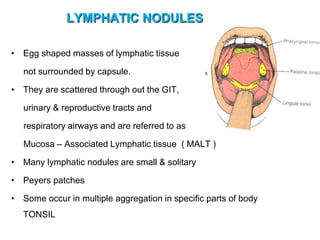
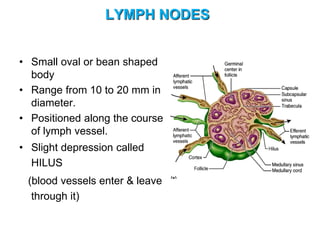
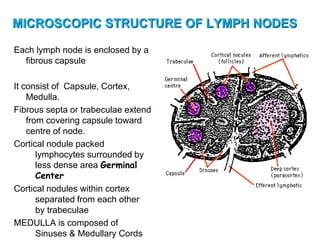
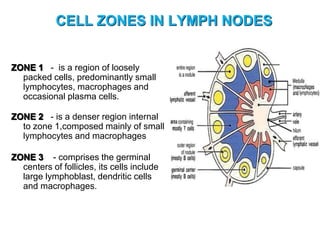
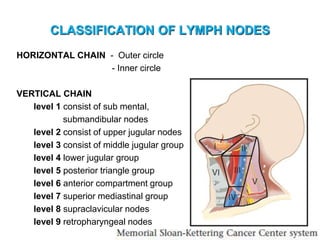
The document provides an overview of the lymphatic system, including its history, development, components, and functions. It discusses how the lymphatic system developed from lymph sacs in the embryo and transformed into nodes. The key components are lymphatic capillaries that collect fluid from tissues, vessels that connect to nodes, ducts like the thoracic duct that return lymph to blood circulation, and lymphoid organs like the thymus, bone marrow, spleen and nodes that help fight infection. The lymphatic system works to remove excess fluid, distribute nutrients, and fight pathogens throughout the body.