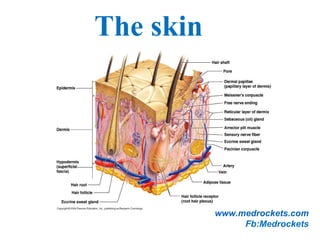
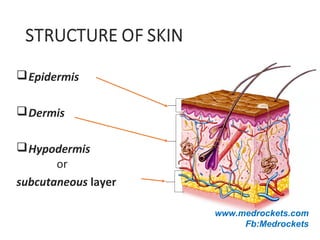
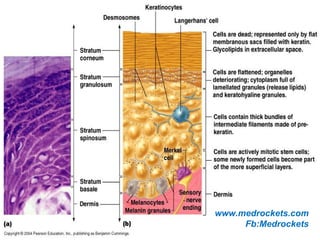
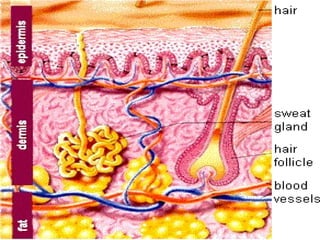
The skin has three main layers - the epidermis, dermis, and hypodermis. The epidermis is made of stratified squamous epithelium. It has several sublayers including the basal, spinous, granular, and stratum corneum layers. The dermis lies beneath the epidermis and contains collagen, elastin, and ground substance. It has two layers - a papillary and reticular layer. Blood vessels, nerves, hair follicles and sweat glands are found in the dermis. The hypodermis or subcutaneous layer lies beneath the dermis and contains fat.