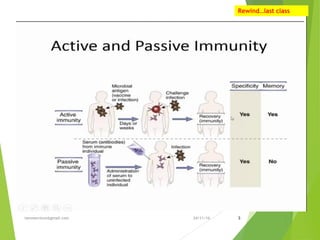
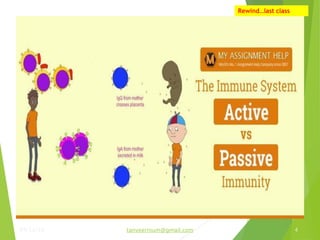
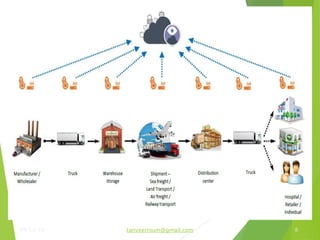
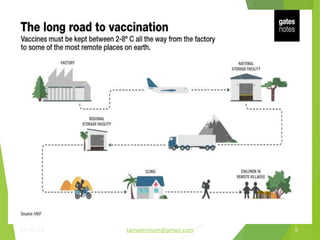
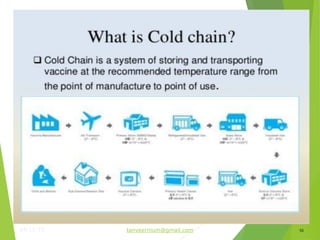
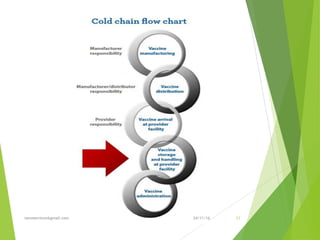
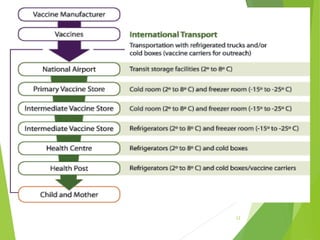
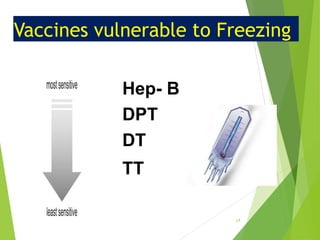
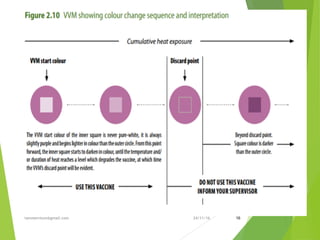
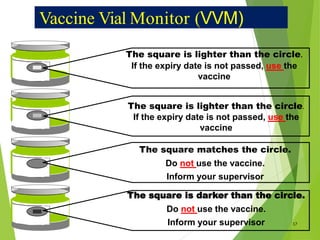
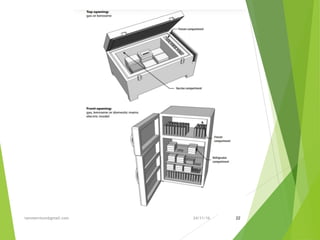
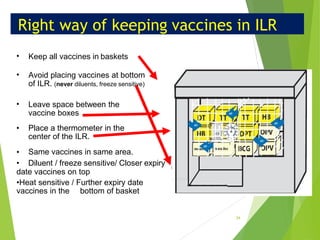
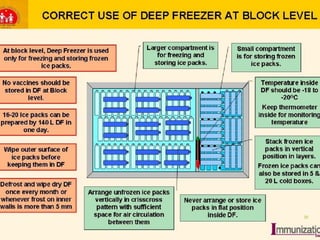
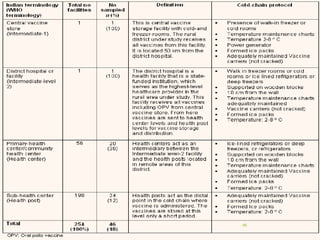
The document discusses the types and functions of antibodies and the importance of vaccines in disease prevention. It emphasizes the cold chain system for vaccine storage and transport to maintain efficacy, detailing temperature sensitivity and equipment used. Additionally, it provides guidelines for proper storage and handling of vaccines to prevent potency loss.