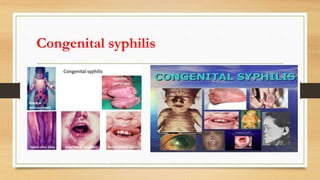
This document discusses syphilis, a sexually transmitted disease caused by the spirochete Treponema pallidum. It defines syphilis and describes the causative organism. It discusses the modes of transmission for acquired and congenital syphilis. The clinical stages of syphilis are outlined including primary, secondary, latent, and tertiary syphilis. The diagnosis, treatment, and prognosis of syphilis are summarized. Congenital syphilis is also described. References are provided.






















![REFERENCES
• Cooley LA1, Pearl ML, Flynn C, Ross C, Hart-Cooper G, Elmore K, et al. Low viral suppression and high HIV diagnosis rate among men who have sex with men with
syphilis--Baltimore, Maryland. Sex Transm Dis. 2015 Apr. 42(4):226-31.
• Su JR, Weinstock H. Epidemiology of co-infection with HIV and syphilis in 34 states, United States—2009. Proceedings of the 2011 National HIV Prevention Conference,
August 13-17, 2011.
• HARRISON LW. The Oslo study of untreated syphilis, review and commentary. Br J Vener Dis. 1956 Jun. 32(2):70-8.
• ROCKWELL DH, YOBS AR, MOORE MB Jr. THE TUSKEGEE STUDY OF UNTREATED SYPHILIS; THE 30TH YEAR OF OBSERVATION. Arch Intern
Med. 1964 Dec. 114:792-8.
• McClure EM, Goldenberg RL. Infection and stillbirth. Semin Fetal Neonatal Med. 2009 Aug. 14(4):182-9.
• Kupka R, Kassaye T, Saathoff E, Hertzmark E, Msamanga GI, Fawzi WW. Predictors of stillbirth among HIV-infected Tanzanian women. Acta Obstet Gynecol Scand.
2009. 88(5):584-92.
• Dismukes WE, Delgado DG, Mallernee SV, Myers TC. Destructive bone disease in early syphilis. JAMA. 1976 Dec 6. 236(23):2646-8.
• Sule RR, Deshpande SG, Dharmadhikari NJ, Joshi VR. Late cutaneous syphilis. Cutis. 1997 Mar. 59(3):135-7.
• [Guideline] U.S. Preventive Services Task Force. Screening for Syphilis Infection. Recommendation Statement. 2004.
• Workowski KA, Bolan GA. Centers for Disease Control and Prevention Sexually Transmitted Diseases Treatment Guidelines. MMWR. June 5, 2015. 64(RR3):1-137.](https://image.slidesharecdn.com/syphilislecturepp-180719075049/85/Syphilis-lecture-PP-30-320.jpg)
![REFERENCES
• GP. Serologic screening for syphilis. Rationale, cost, and realpolitik. Sex Transm Dis. 1996 Jan-Feb. 23(1):45-50.
• Young H. Syphilis. Serology. Dermatol Clin. 1998 Oct. 16(4):691-8.
• Binnicker MJ, Jespersen DJ, Rollins LO. Direct comparison of the traditional and reverse syphilis screening algorithms in a population with a
low prevalence of syphilis. J Clin Microbiol. 2012 Jan. 50(1):148-50.
• [Guideline] Workowski KA, Berman SM. Sexually transmitted diseases treatment guidelines, 2006. MMWR Recomm Rep. 2006 Aug 4. 55:1-94.
• U.S. Preventive Services Task Force. Screening for syphilis infection in pregnancy: U.S. Preventive Services Task Force reaffirmation
recommendation statement. Ann Intern Med. 2009 May 19. 150(10):705-9.
• Ghanem KG. Management of Adult Syphilis: Key Questions to Inform the 2015 Centers for Disease Control and Prevention Sexually
Transmitted Diseases Treatment Guidelines. Clin Infect Dis. 2015 Dec 15. 61 Suppl 8:S818-36.
• [Guideline] Workowski KA, Berman S. Sexually transmitted diseases treatment guidelines, 2010. MMWR Recomm Rep. 2010 Dec 17. 59:1-110.
• Ghanem KG, Workowski KA. Management of adult syphilis. Clin Infect Dis. 2011 Dec. 53 Suppl 3:S110-28.](https://image.slidesharecdn.com/syphilislecturepp-180719075049/85/Syphilis-lecture-PP-31-320.jpg)
