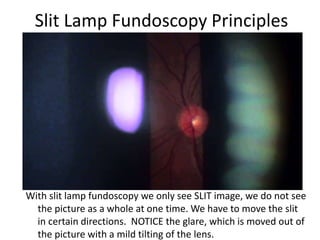
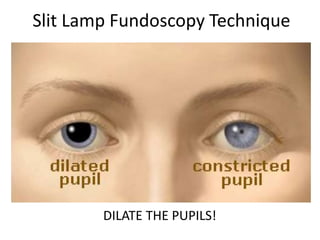
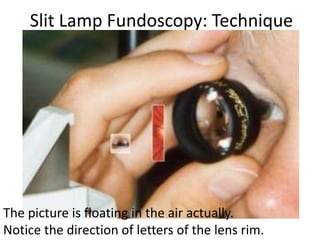
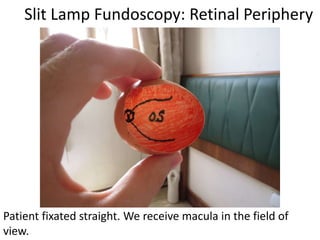
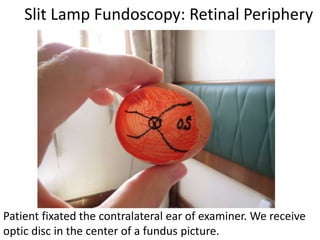
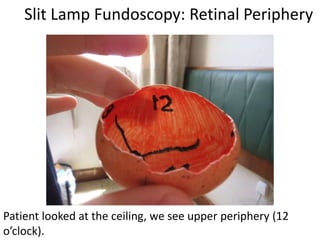
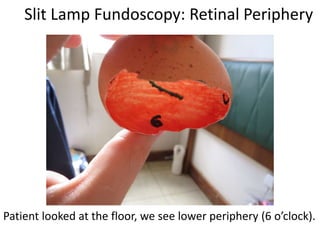
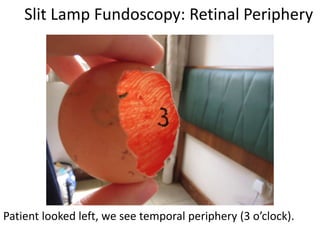
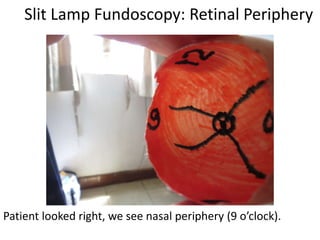
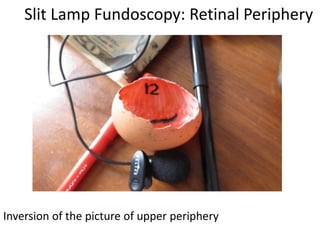
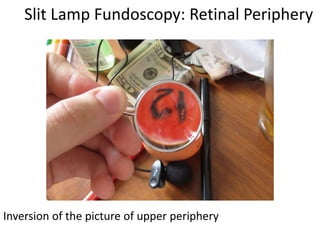
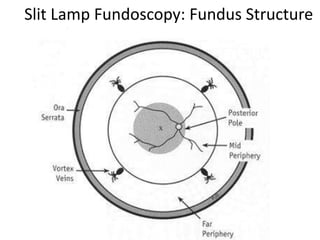
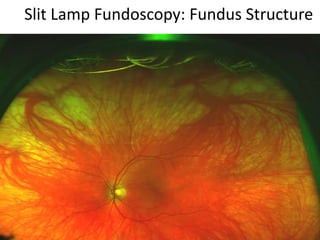
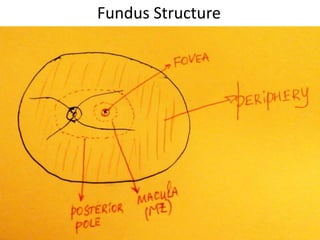
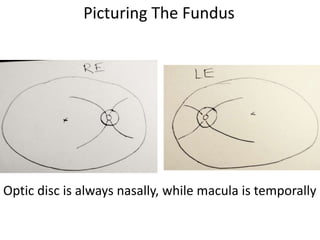
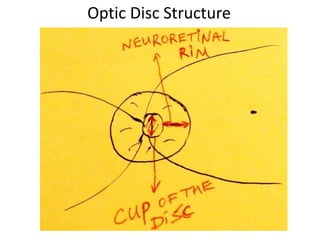
The document outlines the principles and techniques of slit lamp fundoscopy, emphasizing the importance of pupil dilation and proper alignment during examination. It details examination steps, including setting up the slit lamp, using appropriate lenses, and understanding the inverted nature of the fundus image. Additionally, it provides guidance on caring for lenses and references various sources for further learning.