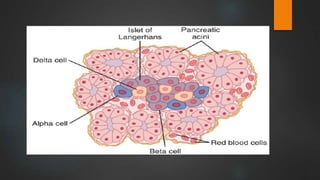
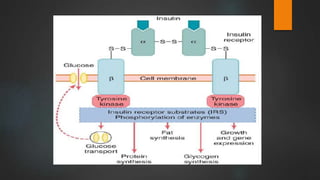
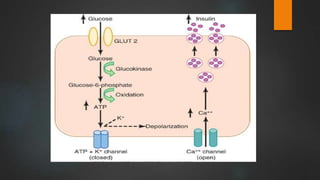
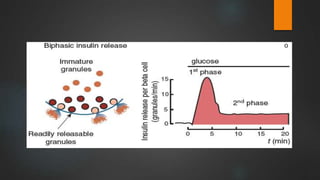
The document discusses the pancreas and insulin. It notes that the endocrine function of the pancreas is performed by clusters of cells called islets of Langerhans, which contain four main cell types that secrete different hormones. It focuses on insulin, describing its source in beta cells, chemistry, levels in plasma, synthesis, metabolism, actions in regulating carbohydrate, protein and fat metabolism, and how its secretion is regulated primarily by blood glucose levels.