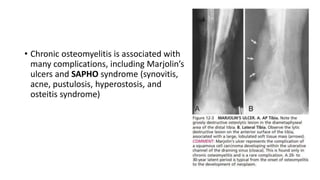
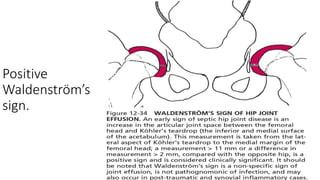
Here are the answers to your questions:
1. Most common site of osteomyelitis - Metaphysis of long bones, especially distal femur and proximal tibia.
2. Most common organism causing osteomyelitis - Staphylococcus aureus.
3. Earliest radiographic and MRI findings of acute osteomyelitis - Soft tissue swelling and loss of fascial planes seen within 24-48 hours on radiographs. Bone marrow edema seen as low signal on T1 and high signal on T2/STIR sequences in MRI.
4. What is sequestrum - Avascular/necrotic bone fragment formed due to osteonecrosis in chronic osteomyelitis