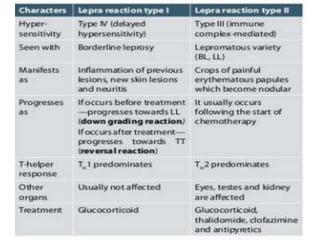
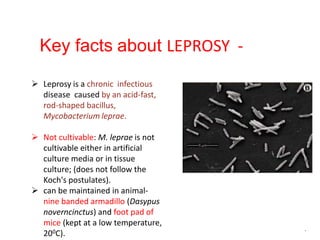
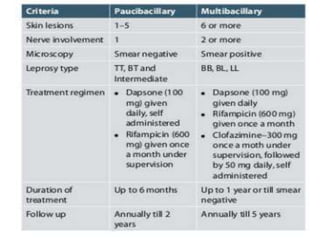
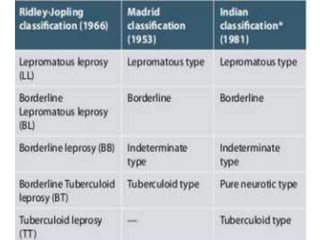
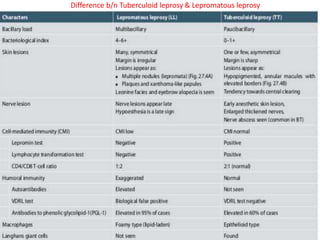
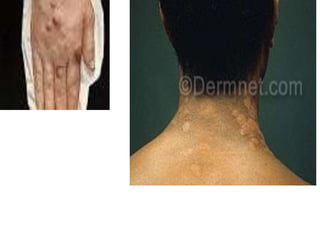
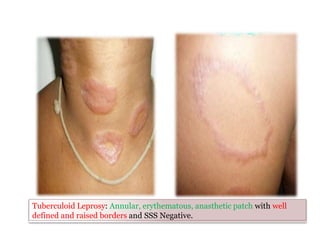
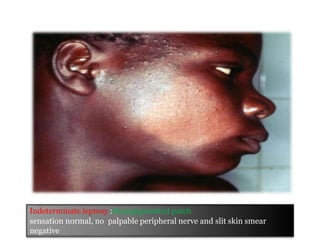
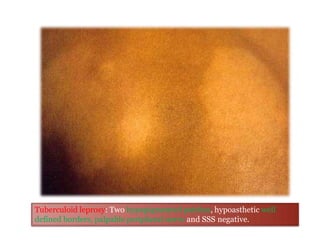
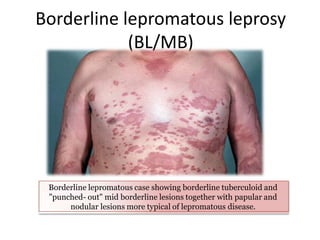
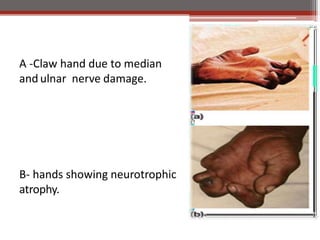
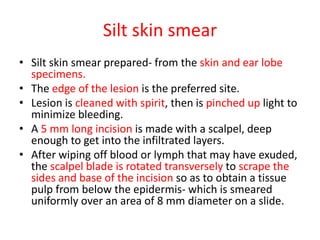
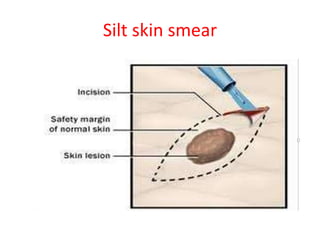
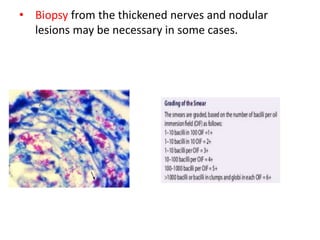
This document contains an MCQ discussion on leprosy. It begins with 13 multiple choice questions about leprosy, including topics like who discovered the causative bacteria, the generation time of Mycobacterium leprae, clinical presentations of leprosy, types of leprosy, treatment, and more. The document then provides explanations and key facts about leprosy, including that it is caused by Mycobacterium leprae, clinical features, types according to skin smear and clinical classification, signs and symptoms, pathogenesis, diagnosis including skin smear microscopy, and treatment with multidrug therapy.