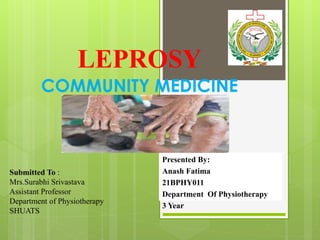
Leprosy Department of Physiotherapy, SHUATS, Prayagraj
- 1. Submitted To : Mrs.Surabhi Srivastava Assistant Professor Department of Physiotherapy SHUATS Presented By: Anash Fatima 21BPHY011 Department Of Physiotherapy 3 Year
- 2. Contents Introduction about Leprosy Incidence of Leprosy Risk Factors Mode of transmission Immunology of leprosy Pathogenesis Classification of leprosy Signs and Symptoms Complications Diagnosis Treatment References
- 3. LEPROSY
- 4. INTRODUCTIO N Leprosy, also known as Hansen's disease, is a chronic infectious disease caused by Mycobacterium leprae an acid fast, rod shaped bacillus. It mainly affects the skin, peripheral nerves, and mucosa of the respiratory tract etc. Leprosy was renamed Hansen’s disease after Norwegian Scientist Gerhard Henrik Armauer Hansen, who in 1873 discovered the slow-growing bacterium now known as Mycobacterium leprae as the cause of the illness. Leprosy is known to occur at all ages ranging from early childhood to old age. Leprosy is curable and treatment during early stages can prevent disability.
- 5. INCIDENCE Leprosy is a neglected tropical disease (NTD) which still occurs in more than 120 countries, with more than 2,00,000 new cases reported every year. More prevalent in countries like India, China, Nepal, Brazil, Indonesia, Myanmar, Madagascar and Nigeria. India still makes up 58.8% of the world's leprosy cases. More commonly in states of Tamil Nadu, Bihar, Puducherry, Andhra Pradesh, Odisha, West Bengal and Assam.
- 6. According to the World Health Organization, approximately 2,08,000 people have leprosy (Hansen's disease) around the globe, with most cases found in Asia and Africa. In the United States, about 100 people receive a leprosy (Hansen's disease) diagnosis every year.
- 7. RISK FACTORS Close Contact- Close contacts with leprosy patients increases the risk of contracting the disease. Armadillo Contact -Armadillo's serve as a reservoir for disease, and armadillo contact increases the risk of transmission of disease. Genetic Risk Factors Immunosuppression
- 8. Endemic Regions -People living in endemic regions along with poor hygiene and poor nutritional status are at increased risk of contracting leprosy Age Poverty Incubation Period The latent period of the disease is variable and is unusually long. It can last from a few weeks to up to 20 years. However, the average incubation period of the disease is 2-7 years. Moreover, it has been observed that patients with paucibacillary (PB) leprosy have a shorter incubation period.
- 9. MODE OF TRANSMISSION Direct contact with untreated patient who shed numerous bacilli from Nasal secretion Damaged skin Mucous membrane of mouth Hair follicles The disease is not spread through casual contact with a person who has leprosy like shaking hands or hugging, sharing meals or sitting next to each other. Materno-foetal transmission across the placenta From infected Armadillo Contact.
- 10. IMUNNOLOGY OF LEPROSY The immune response in leprosy is T-cell Mediated (CMI) delayed Hypersensitivity type IV. Person with ‘GOOD’ CMI response (NORMAL CD4-T HELPER CELLS) develops milder & localised form of the disease (Tuberculoid Leprosy) with less bacterial load. Whereas, in persons with ‘WEAK OR ABSENT’ CMI (LOW CD4-T HELPER CELLS), develop disseminated wide spread disease (Lepromatous Leprosy) with high bacterial load.
- 11. PATHOGENESIS Bacilli enter the body usually through respiratory system After entering the body, bacilli migrate towards the neural tissue and enter Schwann cells. Can also be found in macrophages, muscle cells and endothelial cells of blood vessels. Slow multiplication inside cells & tissues with lower temperature (about 12 – 14 days for one bacterium to divide into two) Further progress depends on the immunological status of the infected person.
- 12. Effect of strong cell mediated immunity Granuloma formation in cutaneous nerve Inflammation within the epineurium causes compression and destruction of unmyelinated sensory and autonomic fibers. Myelinated motor fibers are the last to get affected producing motor impairment. Severe inflammation may result in caseous necrosis within the nerve. Sensory loss – 30% of sensory fibers are destroyed M. leprae may escape from nerve to adjacent skin at any time and cause classical skin lesion(s).
- 13. Effect of depressed Cell Mediated Immunity Bacilli multiply unchecked in schwann cells and destroy the nerve. Bacilli liberated by infected and destroyed cells are engulfed by histiocytes. Wandering macrophages - travel to other tissues, through blood, lymph or tissue fluid.
- 14. M.Laprae bacteria Enter through respiratory tract Good CMI response Schwann cells in cooler places(cutaneous nerves and peripheral nerve trunks of limbs and face) bacilli multiply in the Schwann cells DISSEMINATED DISEASE (BB,BL,LL) Weak CMI response No Signs and Symptoms Signs and Symptoms: Skin, Nerve Leisons (IL,TT,BT)
- 15. CLASSIFICATION OF LEPROSY According to WHO, leprosy can be classified on the basis of clinical manifestations and skin smear results. In the classification based on skin smears, patients showing negative smears at all sites are said to have paucibacillary leprosy (PB). While those showing positive smears at any site are said to have multibacillary leprosy (MB).
- 17. Indeterminate leprosy (IL) Shows as a hypopigmented or erythematous macule with little to no sensation. Bacilli are not usually found in this biopsy. If the lesion shows not to be fully developed, it should develop into another type within the leprosy spectrum. Borderline lepromatous leprosy (BL) Lesions, in this case, include erythematous macules, nodules, or papules that show no distinct pattern of appearance on the body. Though normal patches of skin can be found, the delineation of the lesions is not clear and spread out. Larger sized lesions are shown to have a disproportionate distribution
- 18. Tuberculoid leprosy (TT) This presents with large hypopigmented or erythematous lesions with clear demarcation and raised margins. Plaque presentation was shown to be scaly. Borderline tuberculoid (BT) BT is defined as macules with a “target” appearance in lesions. In this specific disease, the number of lesions is higher than TT and usually shows on one side of the body. When referencing the previously mentioned WHO classification, these types of lesions are considered “paucibacillary.”
- 19. Significantly progressed cases present with body hair loss along with nodular enlargement of earlobes. Mucosal invasion can resemble stuffiness, similar to the common cold. A perforated septum or collapse could occur unless treatment is readily sought after. Also, asymptomatic presentation is possible with sporadic bacteremia during this disease. M. leprae, in this case, progresses with focal lesions in several organs. Some situations show organisms to be present in the liver or marrow after biopsies have been requested. Involvement with testicles and larynx is also possible. Lepromatous leprosy (LL)
- 20. SIGNS AND SYMPTOMS The disease can cause skin symptoms such as: A large, discolored lesion on the chest of a person with Hansen’s disease. Discolored patches of skin, usually flat, that may be numb and look faded (lighter than the skin around) Growths (nodules) on the skin Thick, stiff or dry skin Painless ulcers on the soles of feet Painless swelling or lumps on the face or earlobes Loss of eyebrows or eyelashes
- 21. Symptoms caused by damage to the nerves are: Numbness of affected areas of the skin Muscle weakness or paralysis (especially in the hands and feet) Enlarged nerves (especially those around the elbow and knee and in the sides of the neck) Eye problems that may lead to blindness (when facial nerves are affected)
- 22. Enlarged nerves below the skin and dark reddish skin patch overlying the nerves affected by the bacteria on the chest of a patient with Hansen’s disease. A large, discolored lesion on the chest of a person with Hansen’s disease.
- 23. COMPLICATIONS Muscle paralysis Trophic ulcer Testicular atrophy Amyloidosis Blindness Charcot joints Loss of eyebrows Keratitis Scleritis Loss of sensation with corneal ulceration with scarring .
- 24. DIAGNOSIS Lepromin skin test The lepromin skin test is used to determine what type of leprosy a person has. How the Test is Performed A sample of inactive (cannot cause infection) leprosy- causing bacteria is injected just under the skin, often on the forearm, so that a small lump pushes the skin up. The lump indicates that the antigen has been injected at the correct depth. The injection site is labeled and examined 3 days, and again 28 days later to see if there is a reaction. How to Prepare for the Test People with dermatitis or other skin irritations should have the test performed on an unaffected part of the body.
- 25. Normal Results o People who don't have leprosy will have little or no skin reaction to the antigen. People with a particular type of leprosy, called lepromatous leprosy, will also have no skin reaction to the antigen. What Abnormal Results Mean o A positive skin reaction may be seen in people with specific forms of leprosy, such as tuberculoid and borderline tuberculoid leprosy. People with lepromatous leprosy will not have a positive skin reaction.
- 26. TREATMENT Treatment Leprosy is a curable disease. The currently recommended treatment regimen consists of three drugs: Dapsone, Rifampicin and Clofazimine. The combination is referred to as multi-drug therapy (MDT). The duration of treatment is 6 months for PB and 12 months for MB cases. Prevention WHO recommends tracing household contacts along with neighborhood and social contacts of each patient, accompanied by the administration of a single dose of rifampicin as preventive chemotherapy.
- 27. LEONINE FACES