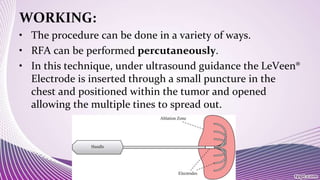
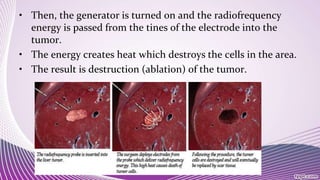
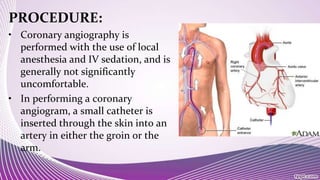
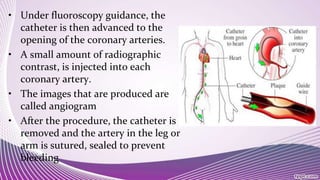
Interventional cardiology and radiology use minimally invasive techniques guided by imaging to diagnose and treat diseases. Some common procedures include radiofrequency ablation to treat cancers, coronary angioplasty and stent placement to open blocked arteries, transjugular intrahepatic portosystemic shunt placement to reduce portal hypertension, and coronary angiography to image heart arteries using contrast dye. These procedures use catheters and stents along with imaging like fluoroscopy to precisely deliver treatments to diseased areas while minimizing patient trauma.