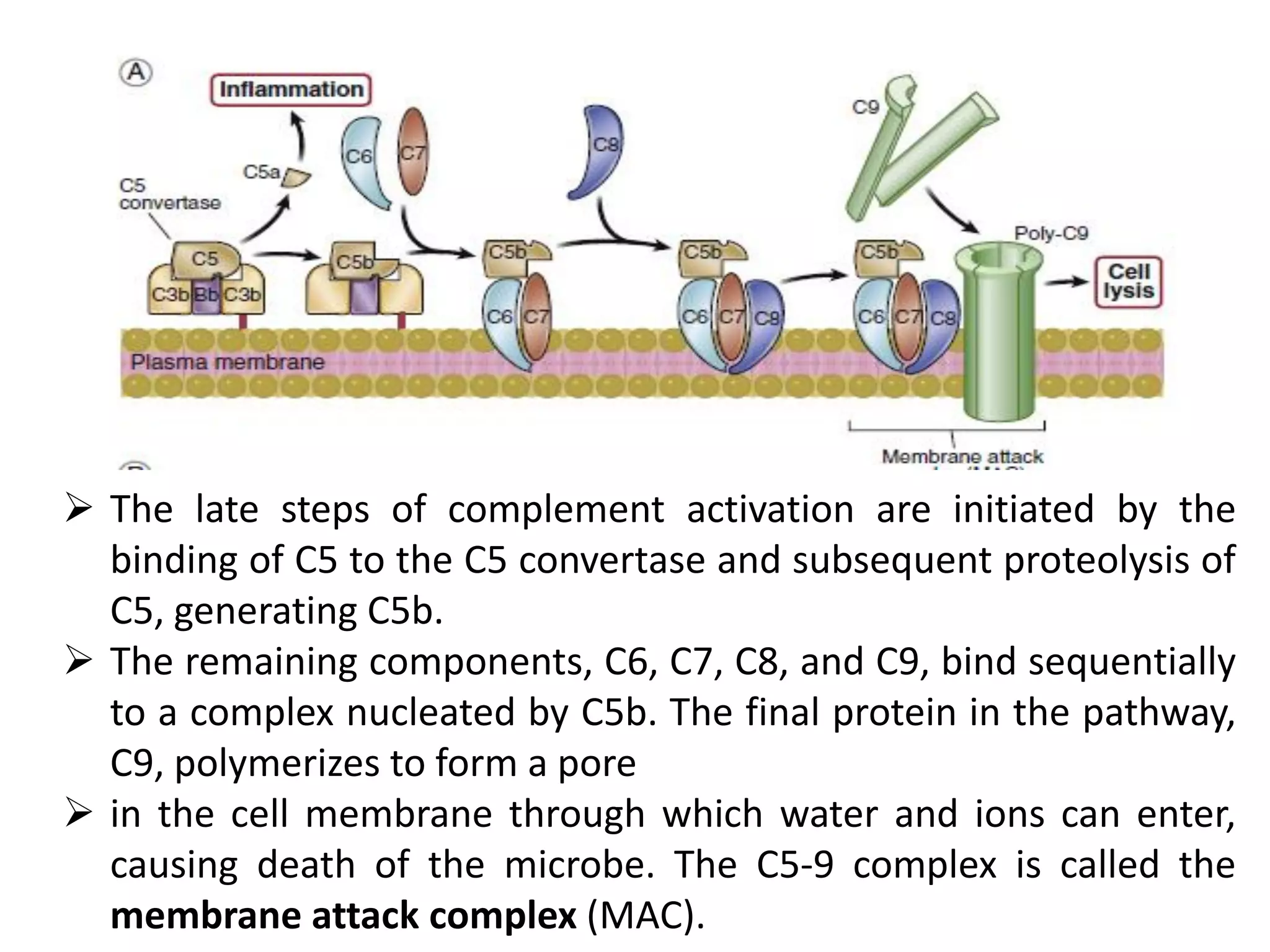
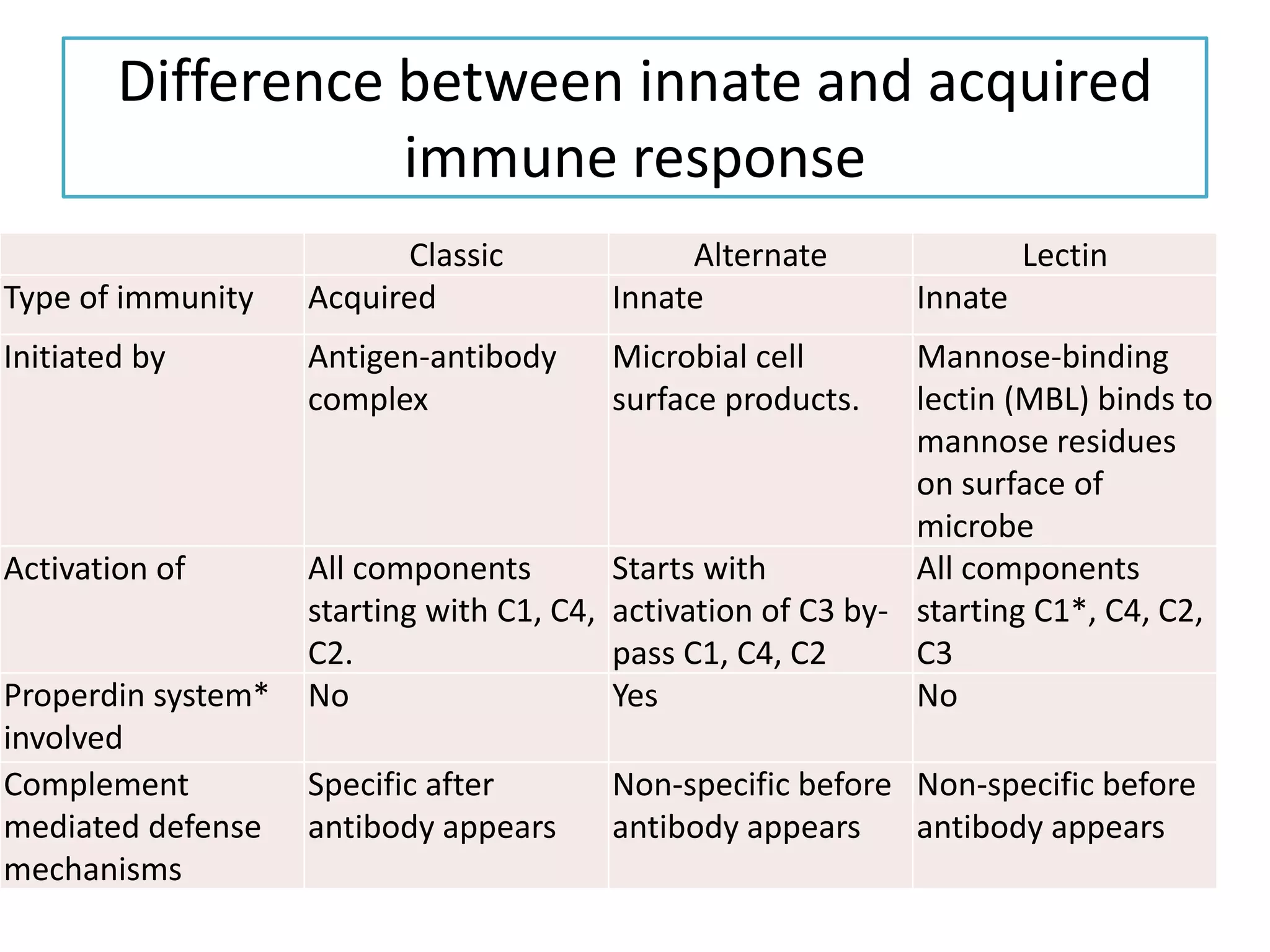
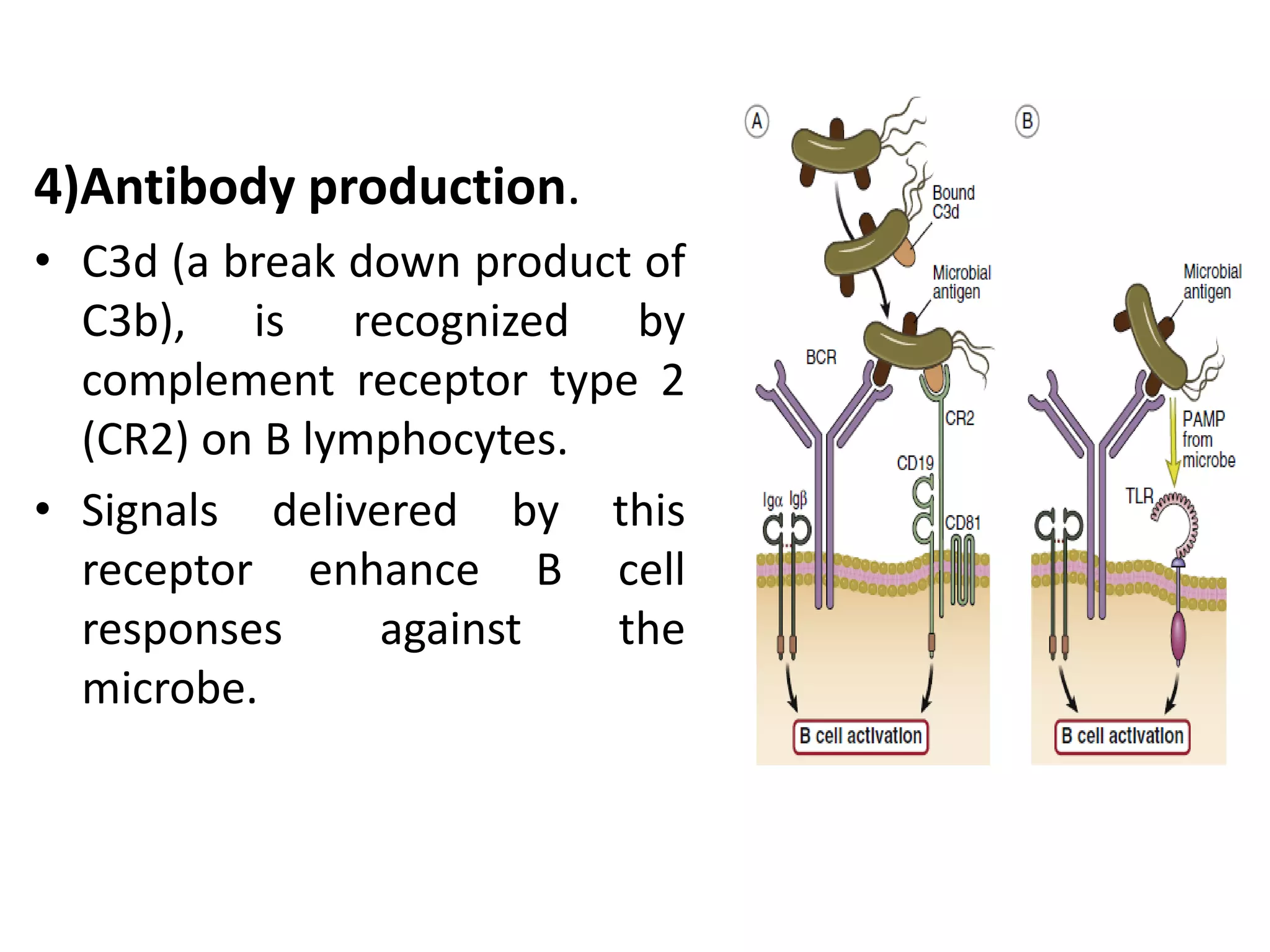
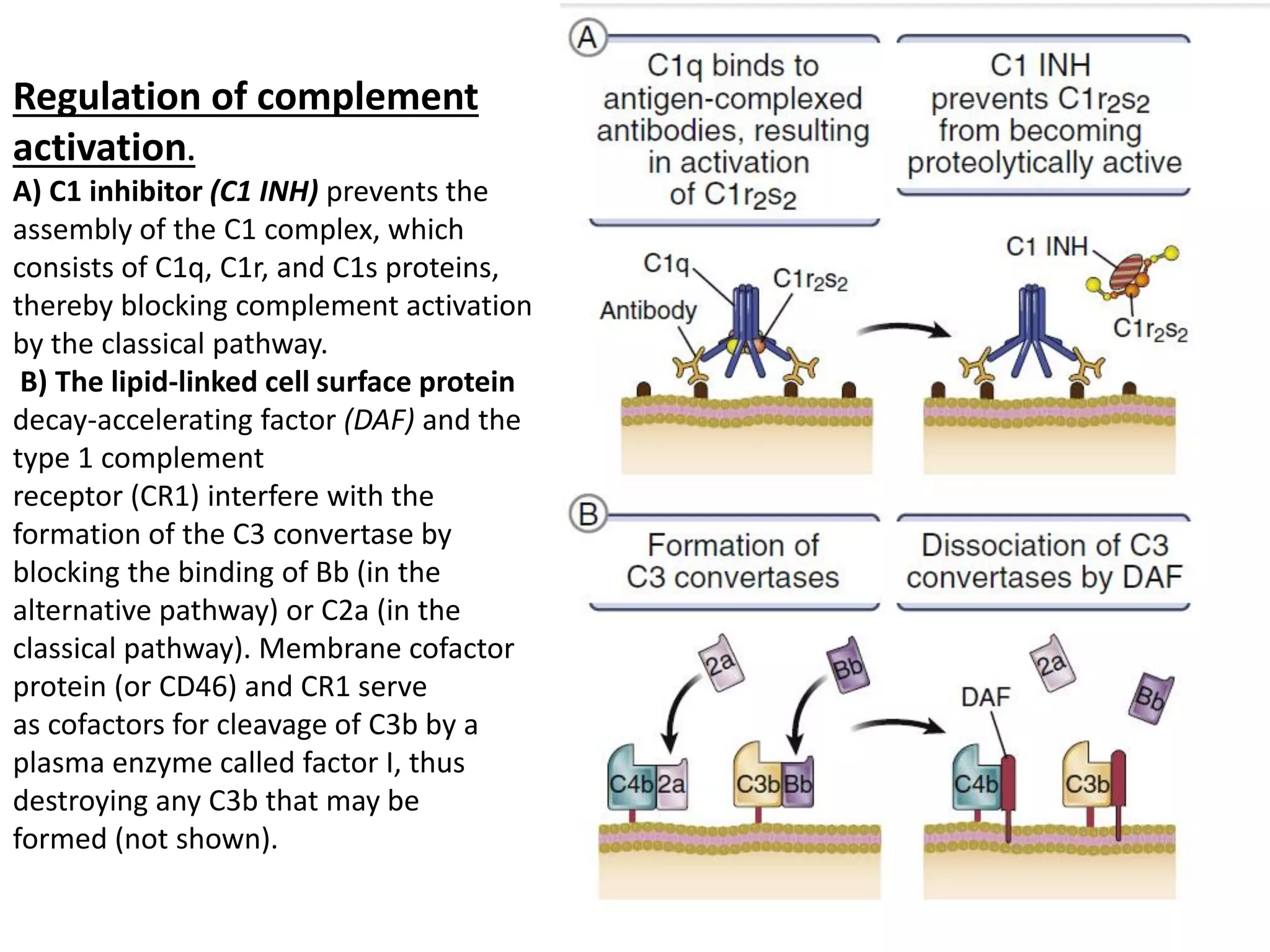
Innate immunity is the body's first line of defense against pathogens. It includes mechanical, chemical, and biological barriers that block pathogen entry. If a pathogen breaches these barriers, the innate immune system responds through cells and proteins. Key components of the innate response are phagocytic cells, complement proteins, acute phase proteins, cytokines, and inflammation. The complement system helps eliminate pathogens through opsonization, cell lysis, and inflammation. Innate immunity provides non-specific protection and helps activate the adaptive immune response.