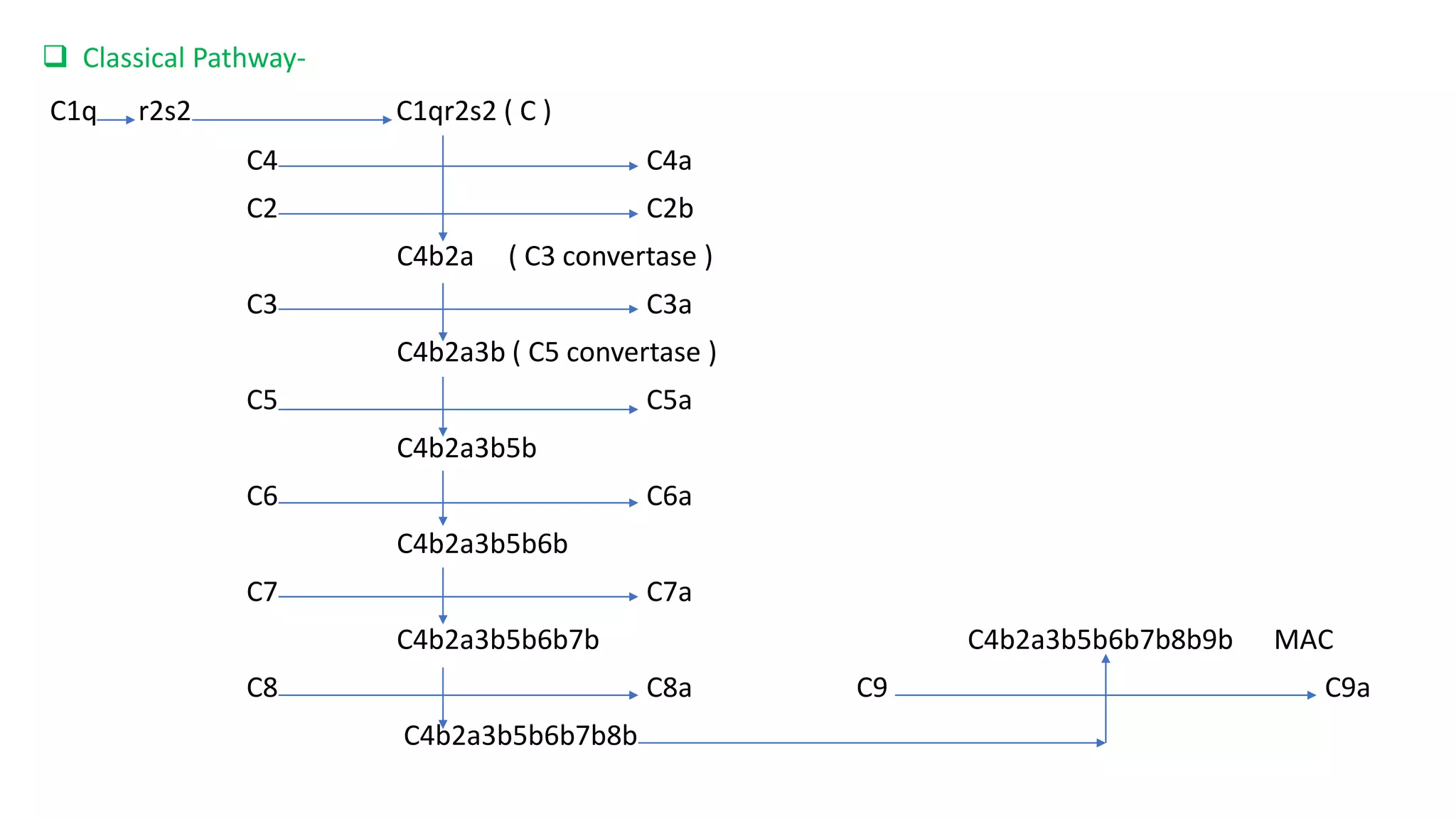
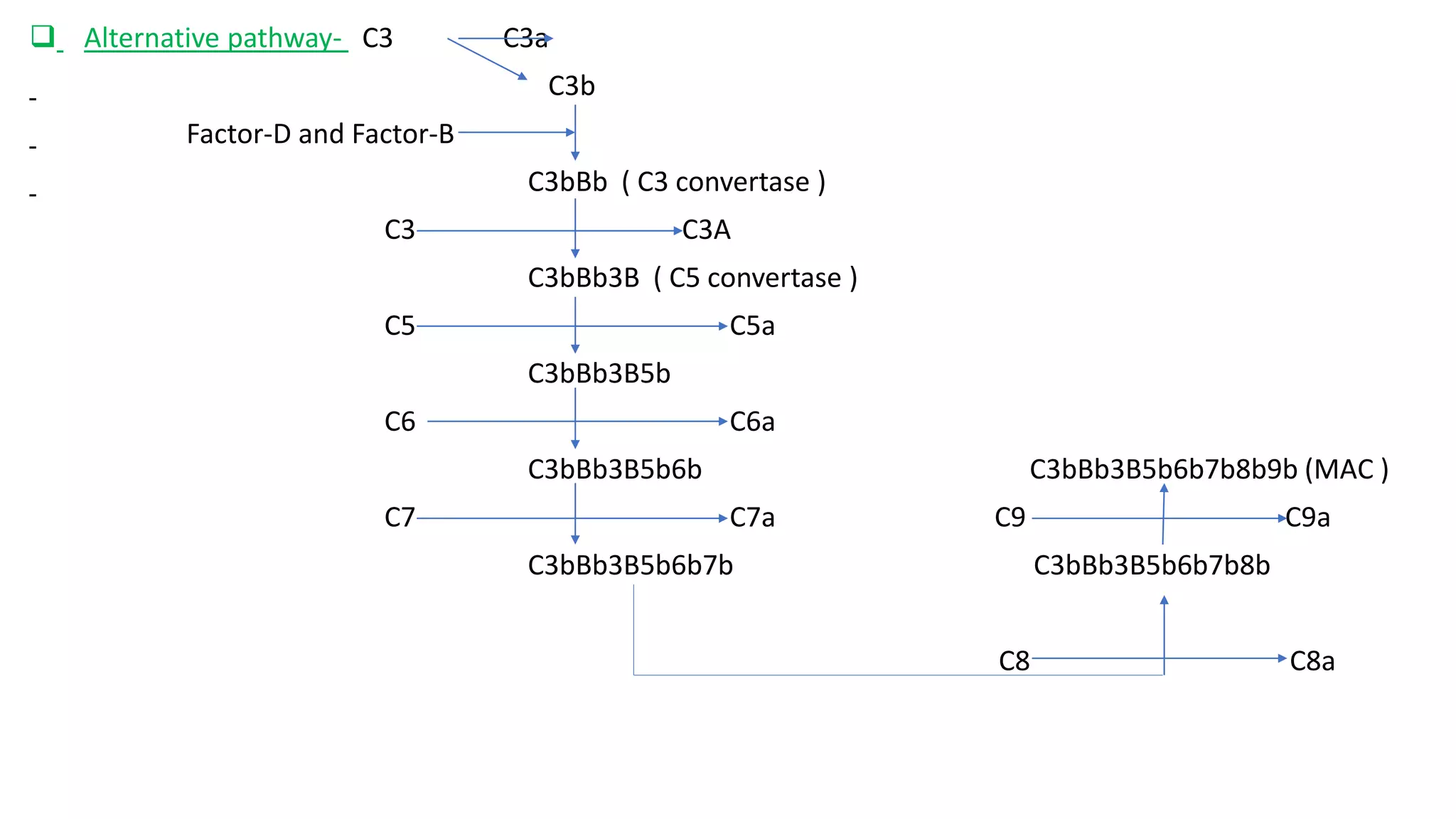
The document discusses the complement system and inflammation. It defines the complement system as part of the immune system that enhances the ability of antibodies and phagocytes to clear pathogens and damaged cells. The complement system consists of proteins that are activated in a cascade to stimulate phagocytes, promote inflammation, and attack cell membranes. Inflammation is defined as the body's immune response to harmful stimuli and is characterized by symptoms like redness, swelling, heat, and pain that help remove pathogens and begin the healing process. Chronic inflammation can potentially lead to diseases if not resolved.