Embed presentation
Downloaded 74 times








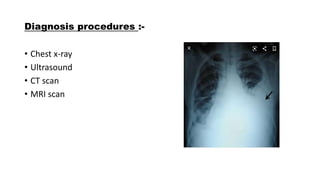


This document discusses haemothorax, which is the presence of blood in the pleural space. It can be caused by trauma, medical issues like pulmonary embolism, or iatrogenically. Clinical presentation includes chest pain, dyspnea, and reduced breath sounds on the affected side. Diagnosis involves chest x-ray, CT scan, or ultrasound. Treatment depends on the cause but typically involves insertion of a chest tube for drainage. Complications can include clot retention, infection, or effusion. Physiotherapy may include deep breathing exercises, mobilization, and assisted coughing to improve ventilation and clear secretions.











