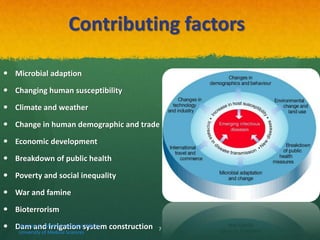
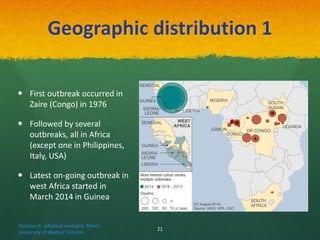
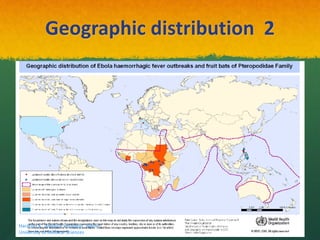
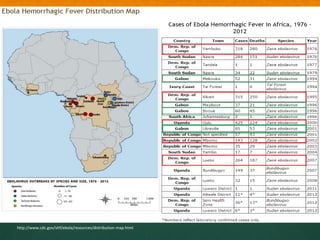
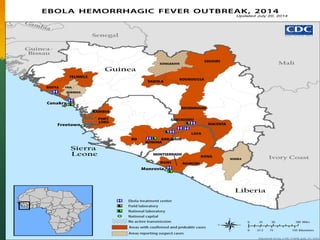
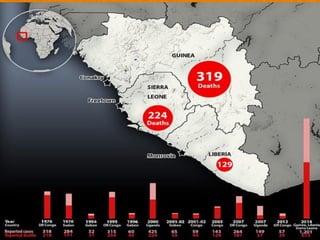
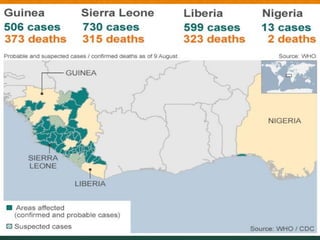
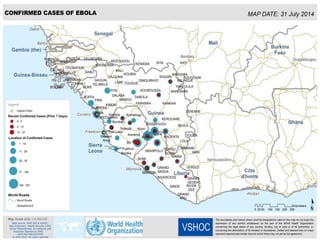
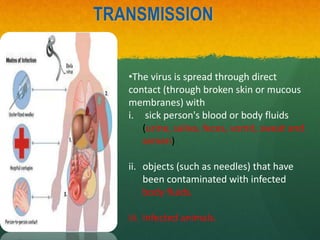
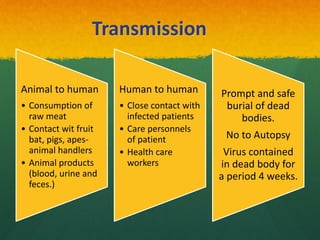
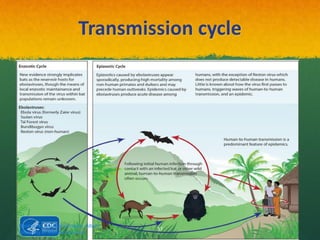
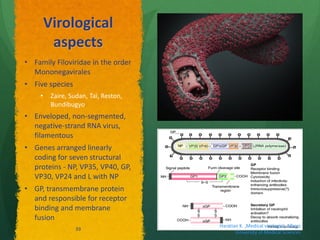
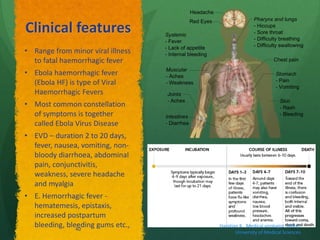
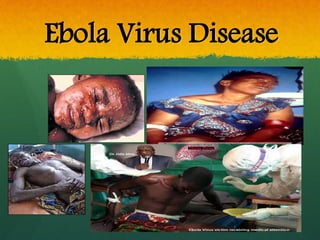
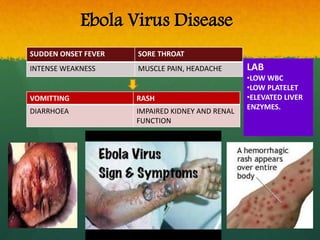
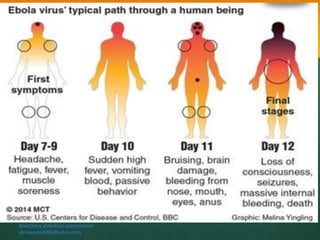
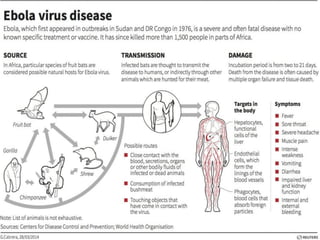
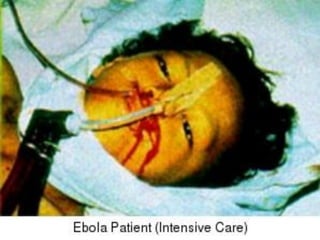
The document discusses Ebola virus disease (EVD) and its threat to public health. It begins with definitions of emerging infectious diseases and re-emerging infectious diseases from the WHO. It then discusses EVD specifically, noting that it is caused by the Ebola virus, which was first identified in outbreaks in Africa in the 1970s. The document outlines the epidemiology of EVD, including its transmission from fruit bats to humans, high fatality rate, and recent outbreak in West Africa. It also summarizes the virological characteristics of Ebola virus and clinical symptoms of EVD, which can range from mild symptoms to severe hemorrhagic fever.