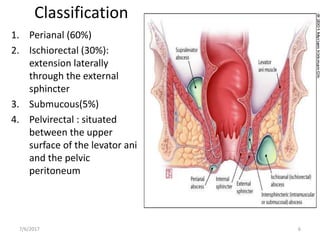
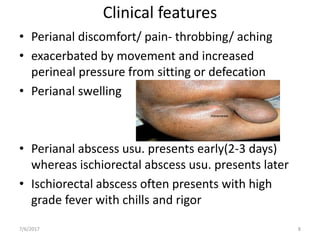
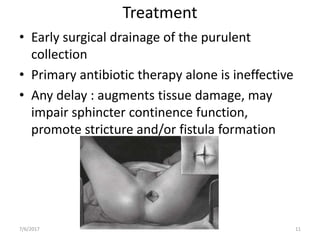
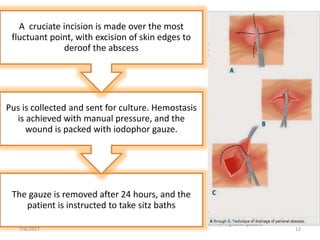
This document presents a case study and overview of anorectal abscesses. It begins with the case of a 28-year-old male presenting with a swelling in his right buttock. On examination, he was found to have an ischiorectal abscess, which was drained surgically. The document then discusses anorectal abscesses in general, classifying them and covering their typical etiology, clinical features, investigations, and primary treatment of surgical drainage and antibiotics. The key points are that anorectal abscesses usually cause throbbing pain and anal swelling, can be classified based on their anatomy, and are generally treated by draining the pus surgically along with supportive care.