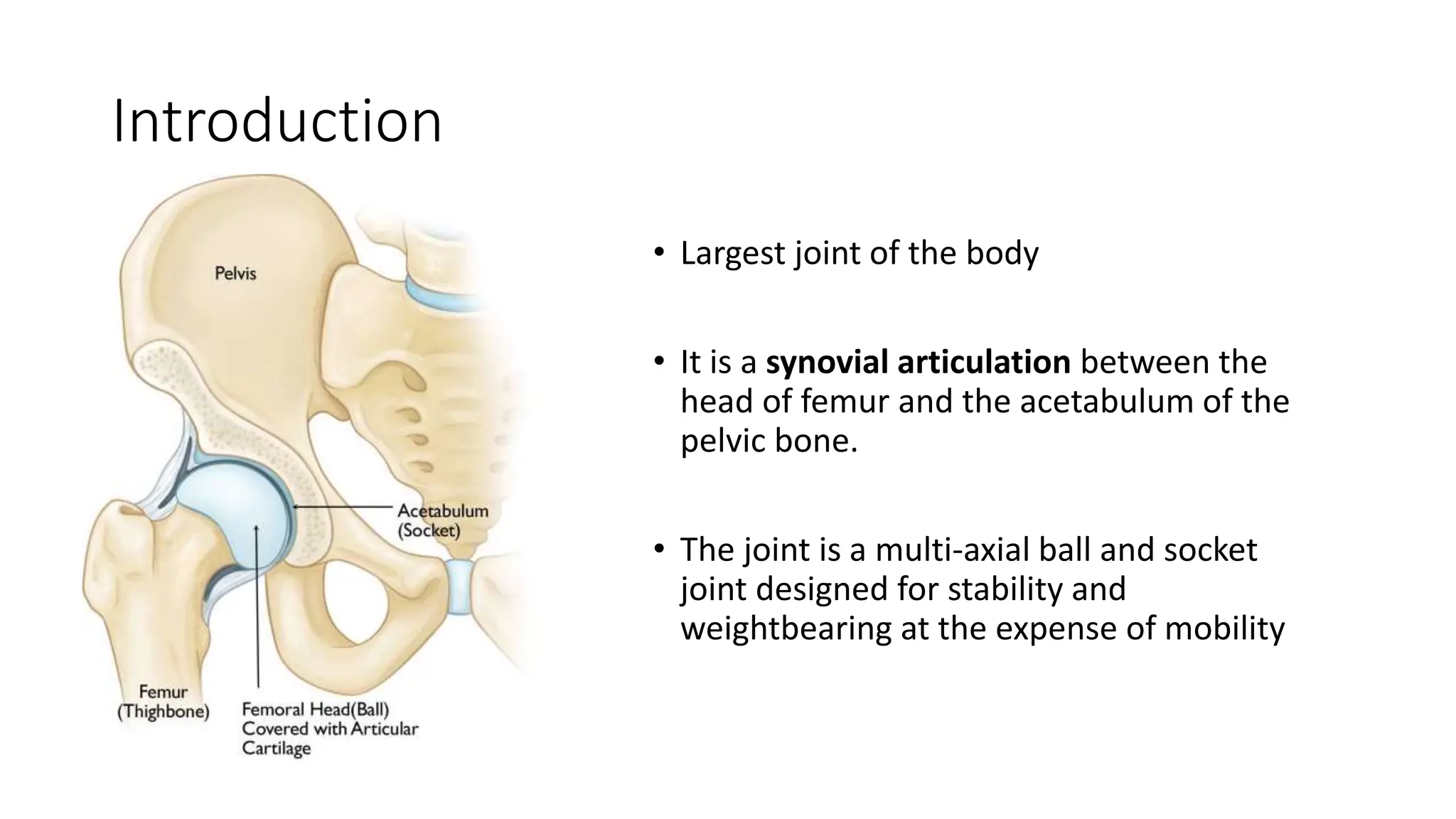
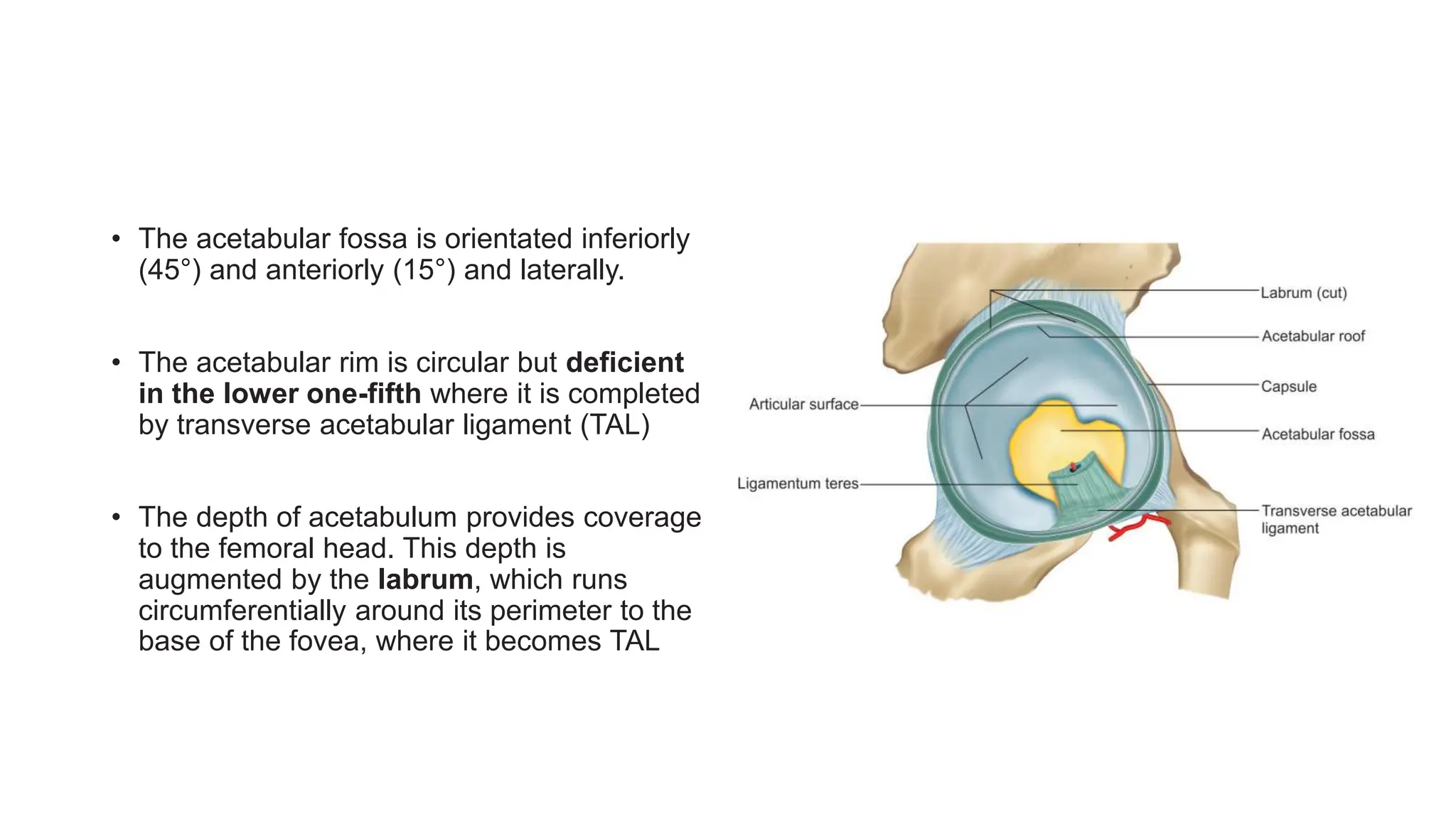
This document discusses surgical hip approaches. It provides details on the anatomy of the hip joint and various ligaments and muscles. It then describes several common surgical approaches including the anterior, anterolateral, and posterior approaches. The anterior approach involves an internervous plane between the sartorius and tensor fascia lata muscles. The anterolateral approach is between the tensor fascia lata and gluteus medius muscles. The posterior approach is either between the gluteus medius and maximus or through splitting of the gluteus maximus. Each approach aims to provide adequate exposure while minimizing damage to surrounding structures.