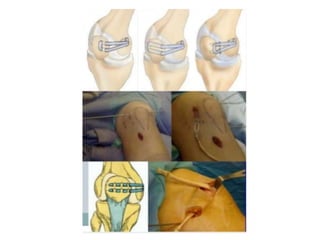
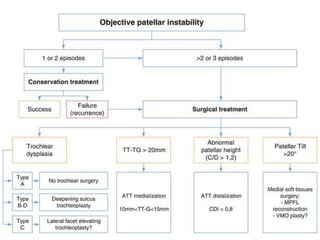
The document provides information on recurrent patellar dislocation, including:
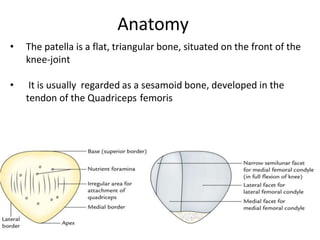
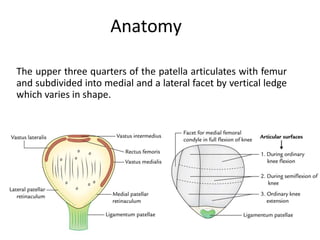
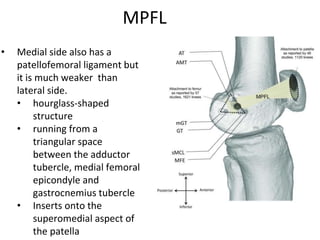
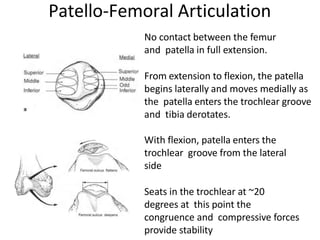
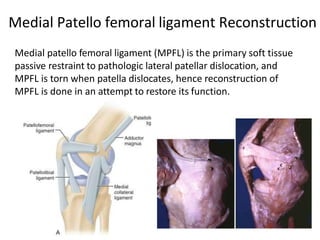
- Anatomy of the patella and its attachments
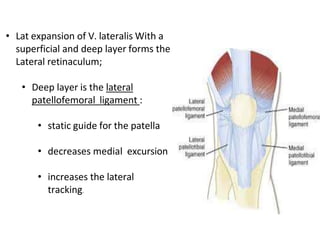
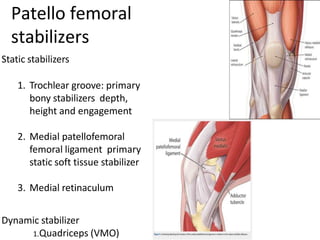
- Static and dynamic stabilizers of the patella
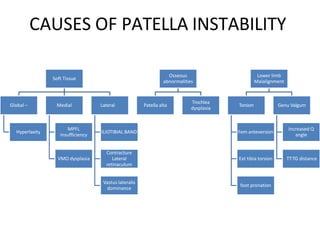
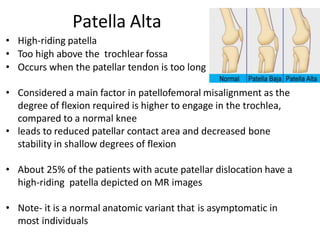
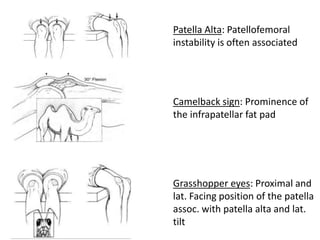
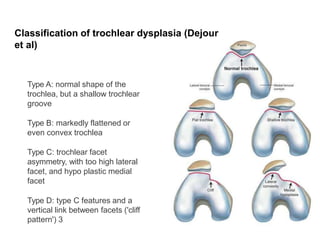
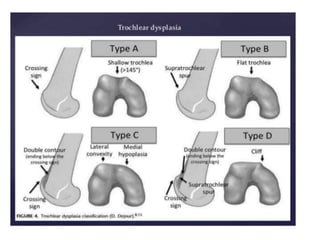
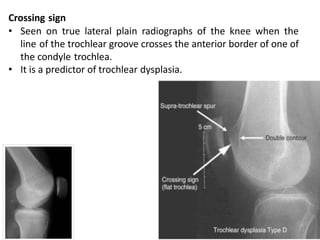
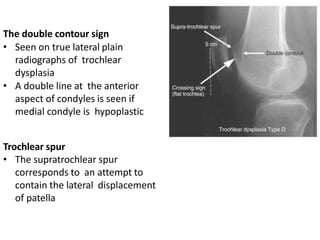
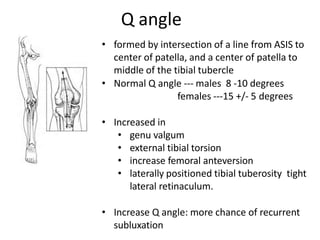
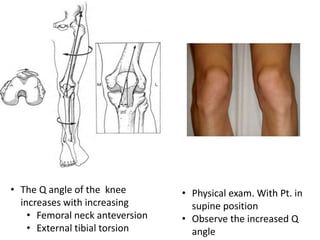
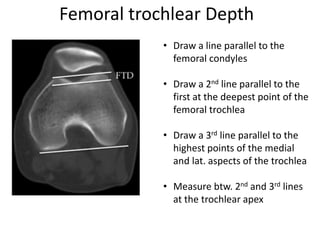
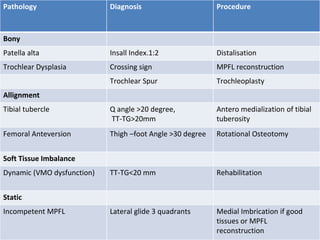
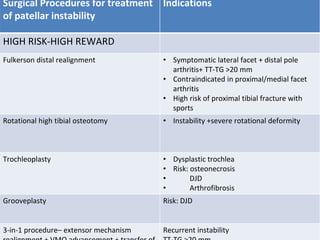
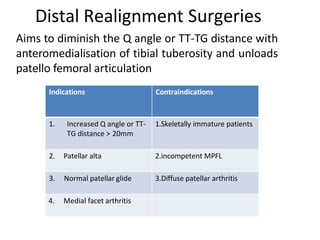
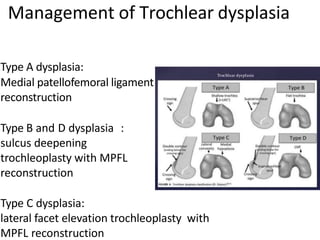
- Causes of patellar instability such as trochlear dysplasia, patella alta, increased Q angle
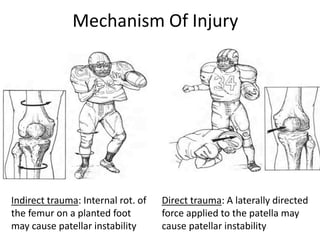
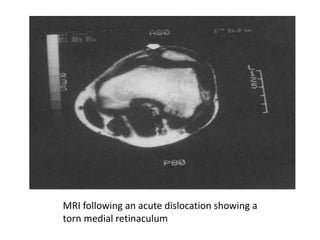
- Mechanisms of injury for acute vs recurrent dislocations
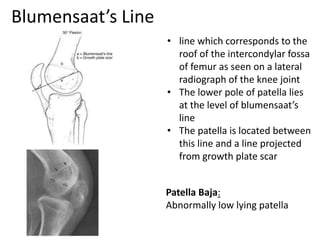
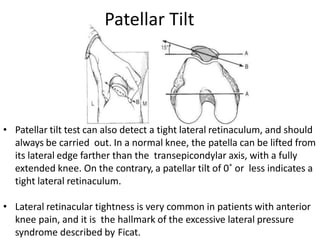
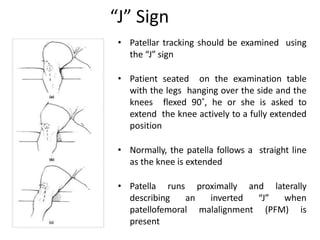
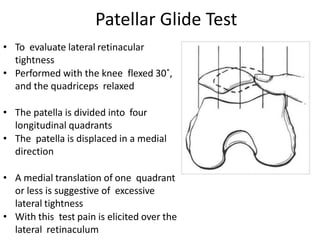
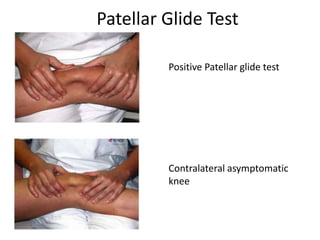
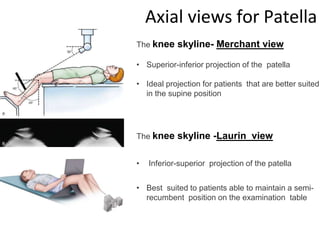
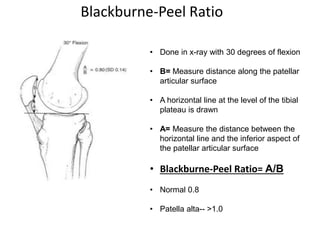
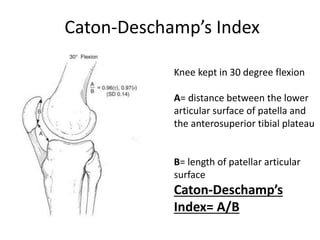
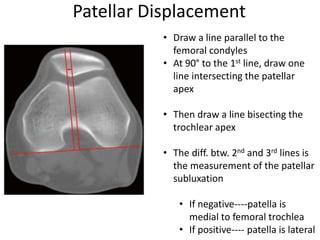
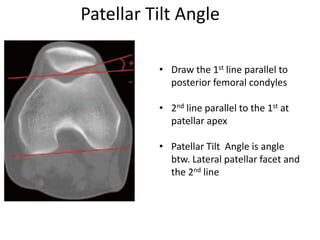
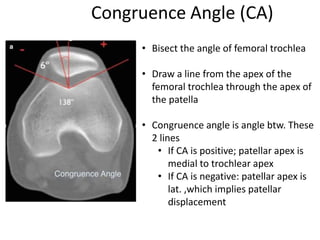
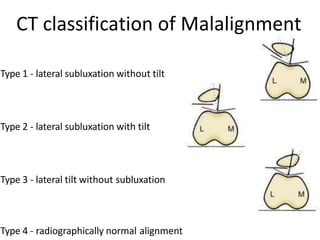
- Evaluation methods like the apprehension test, patellar glide test, and imaging views