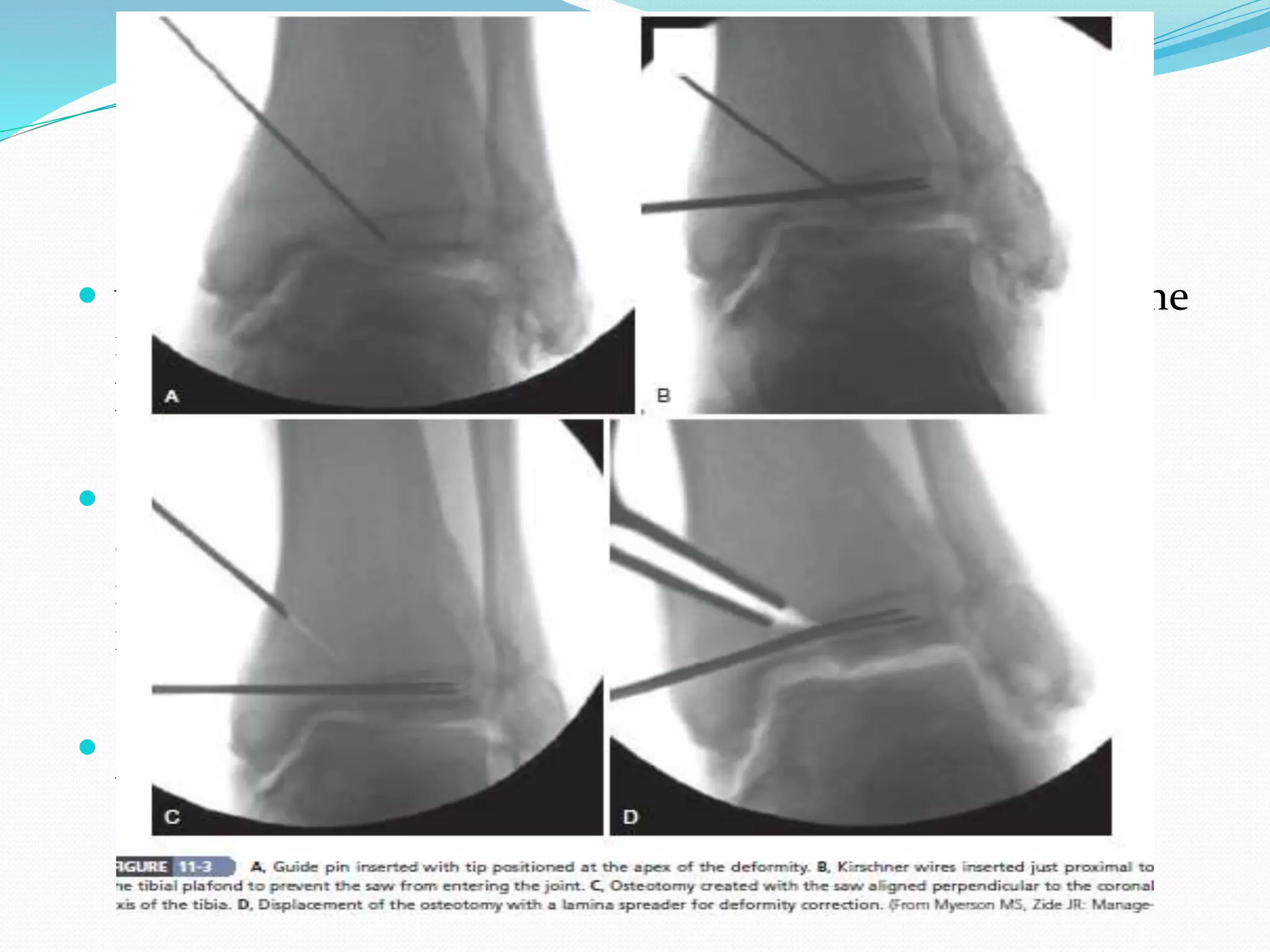
This document provides an overview of the anatomy of the ankle joint and ankle arthrodesis (fusion). It describes the bones and ligaments that make up the ankle joint, including the tibia, fibula, and talus. It discusses the indications, contraindications, surgical technique, and postoperative care of ankle arthrodesis, which is performed to treat ankle arthritis and pain. The optimal position for fusion is slight dorsiflexion with mild hindfoot valgus and external rotation. Preoperative planning involves assessing bone quality, alignment, and arthritis in other joints like the subtalar.