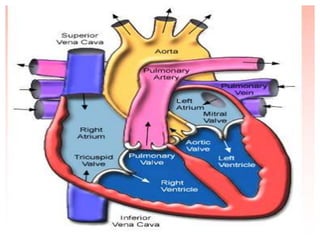
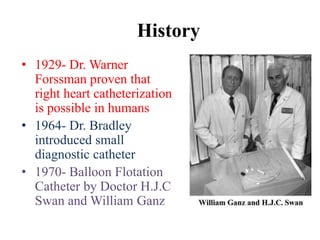
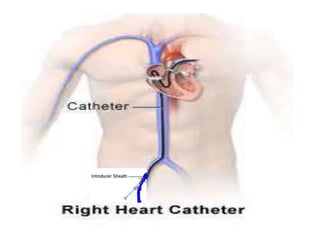
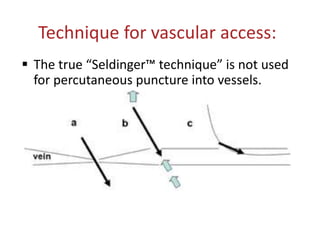
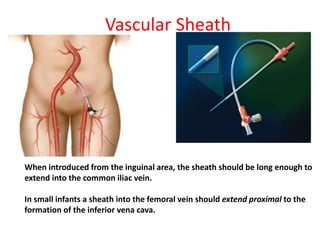
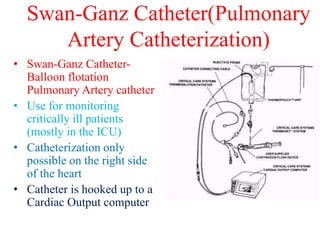
The document discusses the history and techniques of pulmonary artery catheterization, tracing its origins from 1844 when Claude Bernard first performed cardiac catheterization on a horse, to significant advancements made by pioneers like Werner Forssmann and H.J.C. Swan. It highlights the development of various catheter technologies, particularly focusing on the Swan-Ganz catheter, which is crucial for monitoring critically ill patients. The ideal specifications for vascular sheaths and the modern approach to right heart catheterization in pediatric and congenital cases are also detailed.