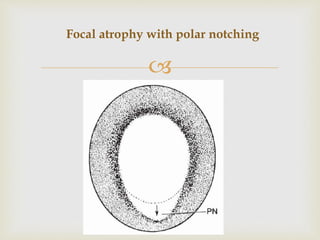
This document discusses the morphological changes that occur in the optic nerve head and retinal nerve fiber layer in glaucoma. It describes the various patterns of glaucomatous optic nerve damage including focal notching, concentric cupping, saucerization, and advanced cupping. Features that indicate glaucomatous damage include neuroretinal rim thinning, disc hemorrhages, and changes in the retinal vasculature around the optic disc. Evaluation of the optic nerve head is important for early detection of glaucoma before visual field loss occurs.