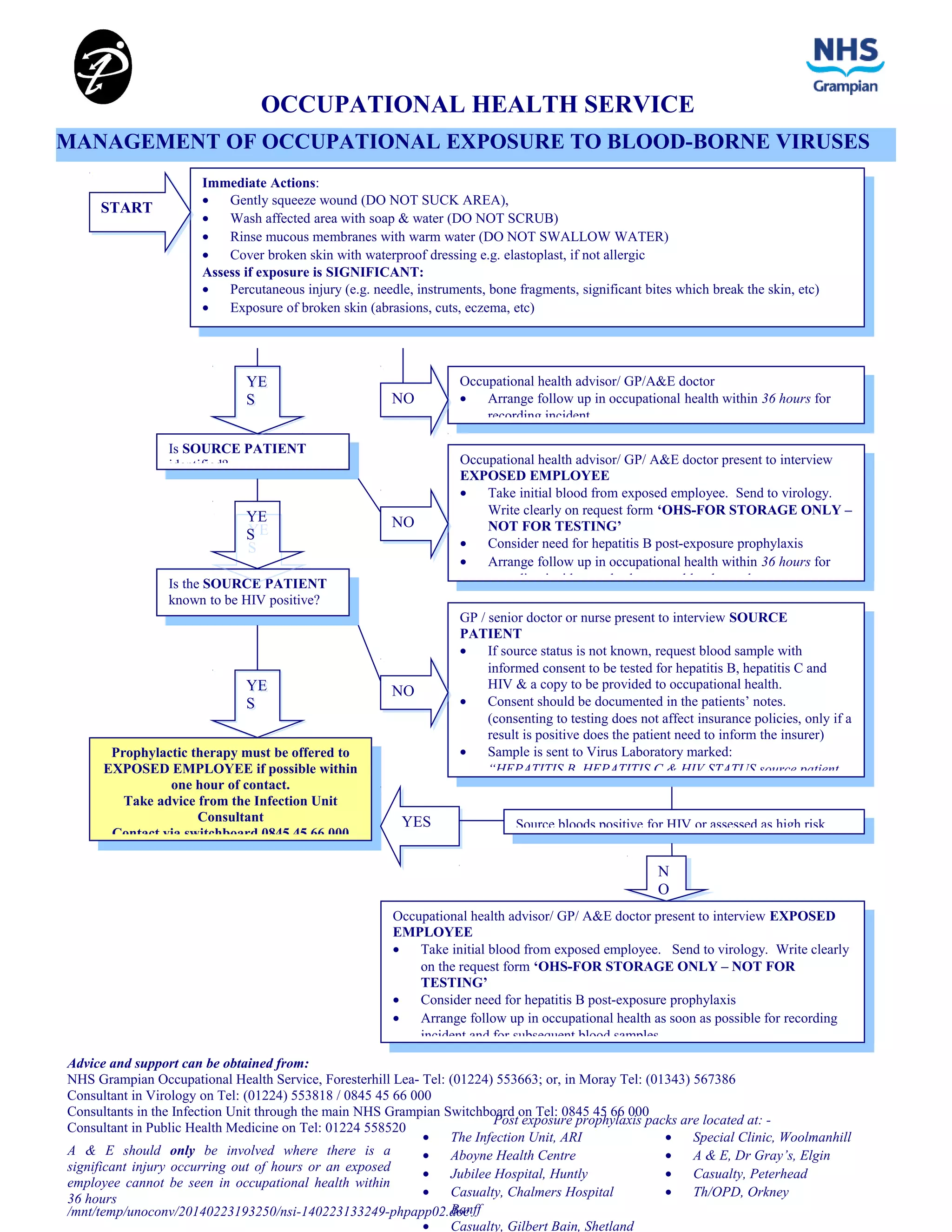
This document provides guidance on immediate actions and assessment for occupational exposure to blood-borne viruses. It outlines steps to take for exposures involving percutaneous injury, broken skin contact, or mucous membrane exposure. It describes arranging follow up care with occupational health or a medical professional within 36 hours to record the incident. For significant exposures, it recommends initial blood samples from the exposed employee and consideration of hepatitis B prophylaxis. If the source patient is identified, consent should be obtained for blood testing and the results provided to occupational health. Prophylactic therapy within one hour of exposure is recommended if the source is known to be HIV positive.