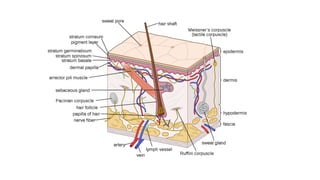
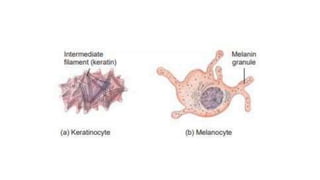
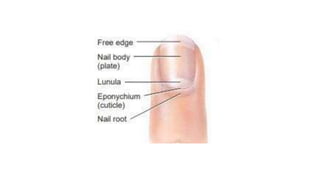
The integumentary system consists of the skin, hair, nails, and glands. The skin is the largest organ and has two main layers - the epidermis and dermis. The epidermis is made of keratinized epithelial tissue and contains keratinocytes, melanocytes, Langerhans cells, and Merkel cells. The dermis is made of connective tissue. Hair, nails, sebaceous glands, and sweat glands are accessory structures that develop from the epidermis and serve protective and temperature regulating functions. The integumentary system maintains body temperature, protects the internal organs, and detects sensations.