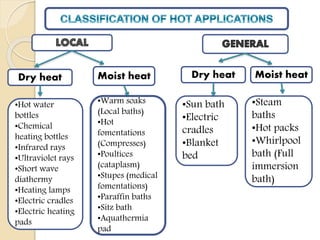
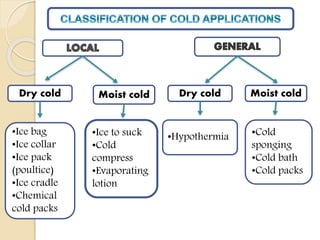
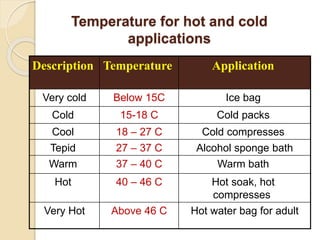
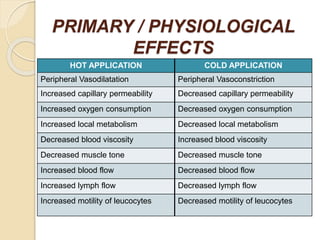
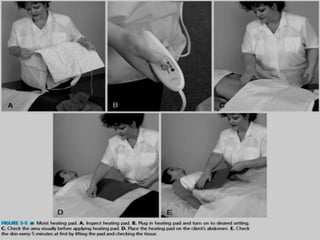
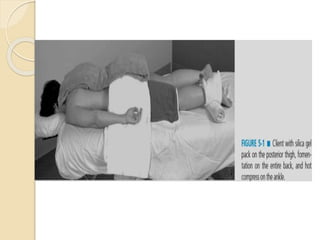
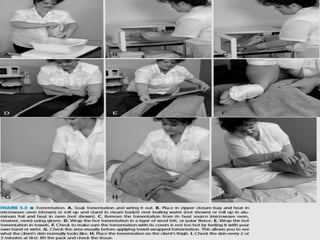
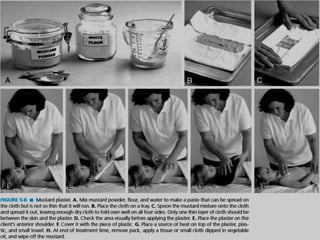
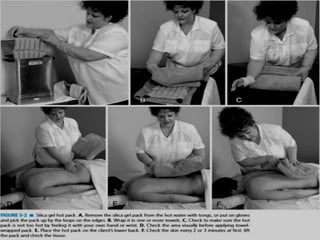
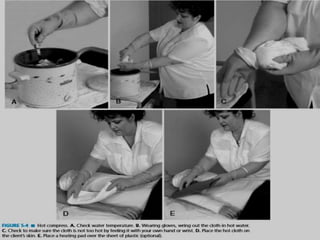
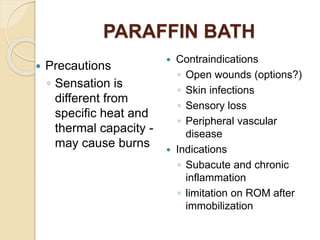
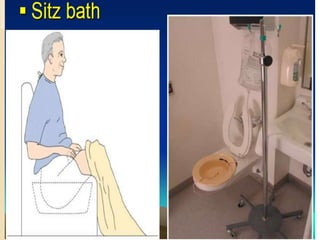
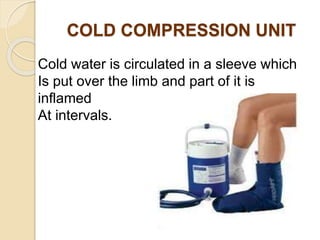
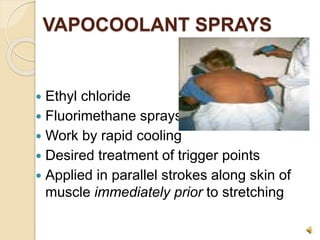
The document discusses the therapeutic uses and application procedures of local heat therapy, including various heating modalities like hot water bottles, heating pads, infrared lamps, and fomentations. It describes the physiological effects of heat in increasing circulation and metabolism, as well as indications and contraindications for different heat therapies. Precautions are outlined to prevent complications like burns during local heat applications.