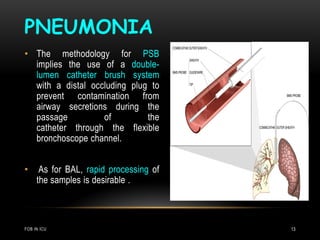
1) Flexible bronchoscopy (FOB) is commonly performed in the ICU for both diagnostic and therapeutic purposes. Some key indications include evaluating pneumonia, hemoptysis, thoracic trauma, and airway inhalation injuries.
2) Performing FOB in critically ill ICU patients presents challenges due to risks of hypoxemia, hypercapnia, and hemodynamic changes from airway obstruction. Careful preparation and monitoring is important.
3) Technical considerations for safe FOB in ventilated patients include using a large ETT, adjusting ventilator settings to minimize changes in tidal volume, and applying suction intermittently to avoid severe desaturation. Proper anesthesia and monitoring of vitals is