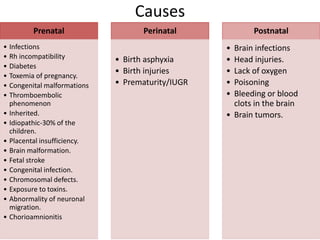
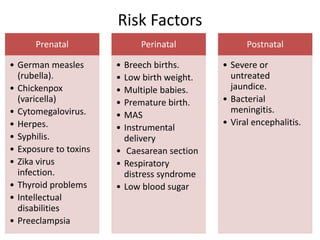
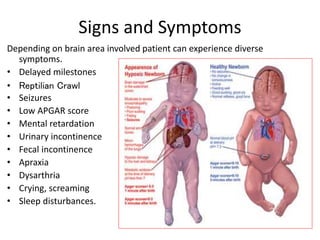
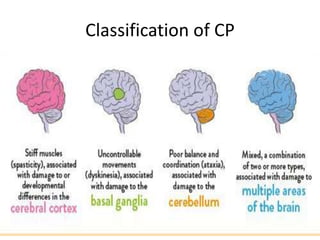
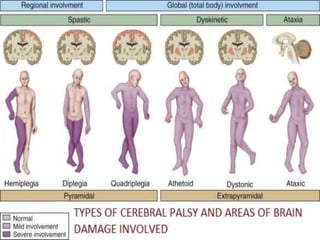
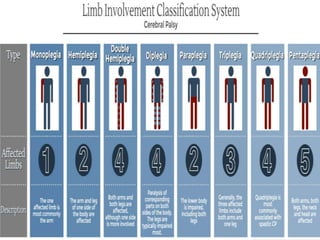
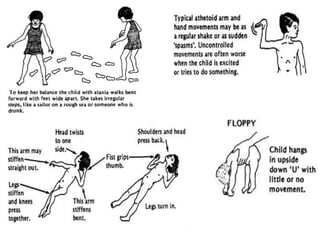
Cerebral palsy is a condition caused by injury to the brain before, during, or after birth that affects muscle movement and coordination. It is the most common physical disability in childhood. The signs and symptoms vary depending on the type and severity but may include difficulties with movement, muscle tone issues, seizures, cognitive impairments, and more. The types are spastic, ataxic, athetoid/dyskinetic, and mixed. Treatment focuses on managing symptoms through therapies, medications, surgery, and assistive devices. Prevention emphasizes prenatal care, immunizations, and neonatal care and resuscitation.