Bed Sore.pptx
- 2. Introduction A bed sore is an ulcer occurring on the skin of any bed ridden patient. Particularly over bony prominences or where two skin surfaces press against one another. Due to pressure the circulation becomes slow and finally death [necrosis] of the tissue occurs. Bedsores — also called pressure ulcers and decubitus ulcers — are injuries to skin and underlying tissue resulting from prolonged pressure on the skin.
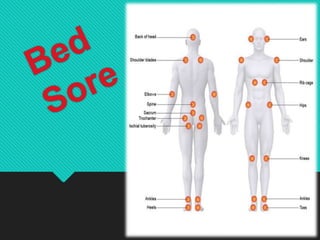
- 3. Common sites of pressure sore • Occiput, scapula, sacral region, hips, elbows, heels. Supine position • Ears, acromion process of the shoulder, greater trochanter of the hip, mideal and lateral condyles of the knee and malleolus of the ankle joint. Side lying position • Acromion process, knees and toes Prone position
- 7. Causes of Bed Sore Actual/ Direct/ immediate Friction Moisture Pressure of pathogenic organism
- 8. A. Actual / Direct / Immediate causes PRESSURE - Pressure is the basic cause of the bed sore. In a sick person the areas of tissue resting against mattress are valnerable areas. The pressure in these areas causes depletion of blood supply. So there is no blood supply to the weight bearing areas which results into the tissue damage. The pressure is caused by weight of the body Splints, Casts Bandages.
- 9. FRICTION FRICTION of the skin with rough bedding causes injury to the skin. Wrinkles in the drawsheet or other bed clothes. Crumbs of food in the bed. Chipped or rough bedpan and its careless handling. Hard surfaces of plaster casts and splints.
- 10. MOISTURE MOISTURE - The skin contact with moisture for a prolong period can lead to maceration of the skin. Patient lying on wet bedding Incontinence of urine and stools Severe perspiration Body discharges
- 11. PRESSURE OF PATHOGENIC ORGANISMS – A. Due to unhygienic condition pathogenic organism multiplies and infection settles on the skin. B. Predisposing or Indirect causes.-Paralysis and limitation of movements. Emaciated and malnourished patients. Oedematous patients, whose tissues are swollen with an accumulation of fluid. Very old with sluggish circulation. Obese patients. Patients with spinal injury. In continent patient. Patient with long term illness, fracture patients.
- 12. Signs and symptoms of Bed sore The early symptoms of bed sore are - redness, heat, tenderness, smarting and discomfort in the area. The area becomes cold to touch and insensitive. Local oedema also present.
- 13. Later symptoms are - area becomes blue, purple or mottled. Due to continued pressure the circulation is cut off, the gangrene develops and affected area is sloughed off.
- 15. Bedsores are divided into 4 stages, from least severe to most severe. These are: Stage 1. The area looks red and feels warm to the touch. With darker skin, the area may have a blue or purple tint. The person may also complain that it burns, hurts, or itches. Stage 2. The area looks more damaged and may have an open sore, scrape, or blister. The person complains of significant pain and the skin around the wound may be discolored.
- 16. Stage 3. The area has a crater-like appearance due to damage below the skin's surface. Stage 4. The area is severely damaged and a large wound is present. Muscles, tendons, bones, and joints can be involved. Infection is a significant risk at this stage.
- 17. Prevention of Bed sore IDENTIFICATION- Identify the patients who are prone to the development of bed sores.
- 18. Prevention of Bed sore DAILY OBSERVATION - Daily observation of the bed sore prone patient for redness, discoloration or blister on pressure points and they should be reported and treated immediately.
- 19. Prevention of Bed sore POSITIONING - Change the position every 2 hourly
- 20. Prevention of Bed sore MASSAGE-Stimulate circulation by regular washing and massage of all areas exposed to pressure.
- 21. a) Frequent movement of helpless patients, if permitted, in order to change their position. Relieve pressure by
- 22. b) Use the comfort devices to take off the pressure from the pressure points e.g. air cushions, air rings etc. Relieve pressure by
- 23. Avoid using rubber rings because, they compress the area of the skin beneath them. So blood supply is decreased around the pressure points. Loosening tight bandages. Padding pressure points inside plaster casts. Relieve pressure by
- 24. Use of pillows to separate parts so that they do not press one another. Use air or water mattresses to decrease the pressure on bony parts Allow the patient to get up and walk about as soon as the doctor gives permission Relieve pressure by
- 25. Well made beds free from crumbs and wrinkles, and with the bottom bedding tightly tucked in. Do not use badly chipped or rough bedpans or drag out bedpans from under the patient without lifting the patient. Avoid Friction By
- 26. Use adequate amount of cotton under splints and plaster casts to avoid friction. Restriction to use sand bags to prevent friction of extremities or head in restless patient, with constant movements. Avoid Friction By
- 27. Immediate changing of any damp linen. Absolute cleanliness and dryness of the skin, particularly where two skin surface come together. After each urination and defecation back must be attended. Wipe off perspiration and keep the patient dry. Avoid Moisture By
- 28. Care of hands to injury by any way. Care while giving and removing bedpan to avoid scratching the skin. Help must be taken while giving and removing bedpans to heavy and seriously ill patients. Care in the use of appliances such as splints, must be well padded and not too tightly applied. Prevent Injury By
- 29. Give a well balanced diet with plenty of vitamins and proteins which will help to keep the tissues healthy and reduce the risk of bed sores. Ask the patient to take adequate fluids. Diet
- 30. Curative Treatment Bed sore is due to the carelessness of the nurse. But if develops do as follows Report to the sister in charge and doctor the early symptoms of a bed sore so that steps may be taken as early as possible to prevent further damage. Prevent the ulcerated area from becoming infected. Use normal saline to clean the ulcered area.
- 31. Curative Treatment Apply heat for the healing of the wound. Use 100 watt electric bulb for 10 minutes. Apply zinc oxide [water proof] ointment on the surface of the wound which will prevent the infection of under lying tissues.
- 32. Curative Treatment It is very helpful. In patients with incontinence of urine. If slough is present, clean the area thoroughly twice in a day with hydrogen peroxide diluted with distilled water. Cut off the slough if it is loose. If there is delay in wound healing, the surgeon may debride the ulcer and a skin graft may be taken over the ulcerated area. If there is infection, give antibiotics according to doctor order.
- 33. Complications Cellulitis. Cellulitis is an infection of the skin and connected soft tissues. It can cause warmth, inflammation and swelling of the affected area. People with nerve damage often do not feel pain in the area affected by cellulitis. Bone and joint infections. An infection from a pressure sore can burrow into joints and bones. Joint infections (septic arthritis) can damage cartilage and tissue. Bone infections (osteomyelitis) can reduce the function of joints and limbs.
- 34. Cancer. Long-term, nonhealing wounds (Marjolin's ulcers) can develop into a type of squamous cell carcinoma. Sepsis. Rarely, a skin ulcer leads to sepsis.
