Bedsores 2
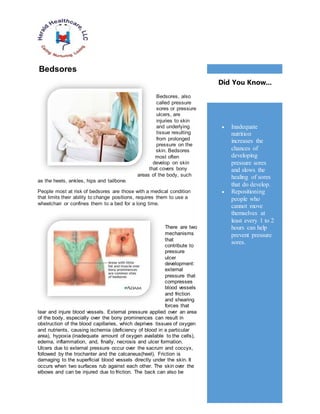
- 1. Bedsores Bedsores, also called pressure sores or pressure ulcers, are injuries to skin and underlying tissue resulting from prolonged pressure on the skin. Bedsores most often develop on skin that covers bony areas of the body, such as the heels, ankles, hips and tailbone. People most at risk of bedsores are those with a medical condition that limits their ability to change positions, requires them to use a wheelchair or confines them to a bed for a long time. There are two mechanisms that contribute to pressure ulcer development: external pressure that compresses blood vessels and friction and shearing forces that tear and injure blood vessels. External pressure applied over an area of the body, especially over the bony prominences can result in obstruction of the blood capillaries, which deprives tissues of oxygen and nutrients, causing ischemia (deficiency of blood in a particular area), hypoxia (inadequate amount of oxygen available to the cells), edema, inflammation, and, finally, necrosis and ulcer formation. Ulcers due to external pressure occur over the sacrum and coccyx, followed by the trochanter and the calcaneus(heel). Friction is damaging to the superficial blood vessels directly under the skin. It occurs when two surfaces rub against each other. The skin over the elbows and can be injured due to friction. The back can also be Inadequate nutrition increases the chances of developing pressure sores and slows the healing of sores that do develop. Repositioning people who cannot move themselves at least every 1 to 2 hours can help prevent pressure sores. Did You Know...
- 2. injured when patients are pulled or slid over bed sheets while being moved up in bed or transferred onto a stretcher. A shear is a separation of the skin from underlying tissues. When a patient is partially sitting up in bed, their skin may stick to the sheet, making them susceptible to shearing in case underlying tissues move downward with the body toward the foot of the bed. This may also be possible on a patient who slides down while sitting in a chair. In addition to pressure, friction, and shear, there are more risk factors of pressure ulcers. Physiological (intrinsic) and non-physiological (extrinsic)) factors that may place a patient at risk include diabetes mellitus, peripheral vascular disease, cerebral vascular accident and hypotension. Other factors are age of 70 years and older, current smoking history, dry skin, low body mass index, impaired mobility, altered mental status, urinary and fecal incontinence, malnutrition, physical restraints, malignancy, history of pressure ulcers. Knowing patient’s condition, risk factors for pressure ulcers, prevention measures are very important. For example, older adults have a higher risk of developing pressure ulcers because chronic diseases, more common in this age group, may compromise circulation and oxygenation of dermal structures. The nutrition and hydration status of elderly may as well predispose them to pressure ulcer formation. Bedsores fall into one of four stages based on their severity. The National Pressure Ulcer Advisory Panel, a professional organization that promotes the prevention and treatment of pressure ulcers, defines each stage as follows: Stage I The beginning stage of a pressure sore has the following characteristics: The skin is not broken. The skin appears red on people with lighter skin color, and the skin doesn't briefly lighten (blanch) when touched. On people with darker skin, the skin may show discoloration, and it doesn't blanch when touched. The site may be tender, painful, firm, soft, warm or cool compared with the surrounding skin. Stage II At stage II: The outer layer of skin (epidermis) and part of the underlying layer of skin (dermis) is damaged or lost. The wound may be shallow and pinkish or red. The wound may look like a fluid-filled blister or a ruptured blister. Stage III At stage III, the ulcer is a deep wound: The loss of skin usually exposes some fat. The ulcer looks crater-like. The bottom of the wound may have some yellowish dead tissue. The damage may extend beyond the primary wound below layers of healthy skin. Stage IV A stage IV ulcer shows large-scale loss of tissue:
- 3. The wound may expose muscle, bone or tendons. The bottom of the wound likely contains dead tissue that's yellowish or dark and crusty. The damage often extends beyond the primary wound below layers of healthy skin. Unstageable A pressure ulcer is considered unstageable if its surface is covered with yellow, brown, black or dead tissue. It’s not possible to see how deep the wound is. Deep tissue injury A deep tissue injury may have the following characteristics: The skin is purple or maroon but the skin is not broken. A blood-filled blister is present. The area is painful, firm or mushy. The area is warm or cool compared with the surrounding skin. In people with darker skin, a shiny patch or a change in skin tone may develop. Pressure ulcers may be caused by inadequate blood supply and resulting reperfusion injury when blood re-enters tissue. A simple example of a mild pressure sore may be experienced by healthy individuals while sitting in the same position for extended periods of time: the dull ache experienced is indicative of impeded blood flow to affected areas. Within 2 hours, this shortage of blood supply, called ischemia, may lead to tissue damage and cell death. The sore will initially start as a red, painful area. The other process of pressure ulcer development is seen when pressure is high enough to damage the cell membrane of muscle cells. The muscle cells die as a result and skin fed through blood vessels coming through the muscle die. This is the deep tissue injury form of pressure ulcers and begins as purple intact skin.
- 4. Healing time is prolonged for higher stage ulcers. While about 75% of Stage II ulcers heal within eight weeks, only 62% of Stage IV pressure ulcers ever heal, and only 52% heal within one year. It is important to note that pressure ulcers do not regress in stage as they heal. A pressure ulcer that is becoming shallower with healing is described in terms of its original deepest depth. Common sites of pressure sores For people who use a wheelchair, pressure sores often occur on skin over the following sites: Tailbone or buttocks Shoulder blades and spine Backs of arms and legs where they rest against the chair For people who are confined to a bed, common sites include the following: Back or sides of the head Rim of the ears Shoulders or shoulder blades Hip, lower back or tailbone Heels, ankles and skin behind the knees Prevention Bedsores are easier to prevent than to treat, but that doesn't mean the process is easy or uncomplicated. And wounds may still develop with consistent, appropriate preventive care. Your doctor and other members of the care team can help develop a good strategy, whether it's personal care with at-home assistance, professional care in a hospital or some other situation. Position changes are key to preventing pressure sores. These changes need to be frequent, repositioning needs to avoid stress on the skin, and body positions need to minimize pressure on vulnerable areas. Other strategies include taking good care of your skin, maintaining good nutrition, quitting smoking and exercising daily.
- 5. In addition, adequate intake of protein and calories is important. vitamin C has been shown to reduce the risk of pressure ulcers. People with higher intakes of vitamin C have a lower frequency of bed sores in those who are bedridden than those with lower intakes. Maintaining proper nutrition in newborns is also important in preventing pressure ulcers. If unable to maintain proper nutrition through protein and calorie intake, it is advised to use supplements to support the proper nutrition levels. Skin care is also important because damaged skin does not tolerate pressure. However, skin that is damaged by exposure to urine or stool is not considered a pressure ulcer. Repositioning in a bed Consider the following recommendations when repositioning in a bed: Reposition yourself frequently. Change your body position every two hours. Look into devices to help you reposition. If you have enough upper body strength, try repositioning yourself using a device such as a trapeze bar. Caregivers can use bed linens to help lift and reposition you. This can reduce friction and shearing. Try a specialized mattress. Use special cushions, a foam mattress pad, an air-filled mattress or a water-filled mattress to help with positioning, relieving pressure and protecting vulnerable areas. Your doctor or other care team members can recommend an appropriate mattress or surface. Adjust the elevation of your bed. If your hospital bed can be elevated at the head, raise it no more than 30 degrees. This helps prevent shearing. Use cushions to protect bony areas. Protect bony areas with proper positioning and cushioning. Rather than lying directly on a hip, lie at an angle with cushions supporting the back or front. You can also use cushions to relieve pressure against and between the knees and ankles. You can cus hion or ''float'' your heels with cushions below the calves Skin care Protecting and monitoring the condition of your skin is important for preventing pressure sores and identifying stage I sores early so that you can treat them before they worsen. Clean the affected skin. Clean the skin with mild soap and warm water or a no-rinse cleanser. Gently pat dry. Protect the skin. Use talcum powder to protect skin vulnerable to excess moisture. Apply lotion to dry skin. Change bedding and clothing frequently. Watch for buttons on the clothing and wrinkles in the bedding that irritate the skin. Inspect the skin daily. Inspect the skin daily to identify vulnerable areas or early signs of pressure sores. You will probably need the help of a care provider to do a thorough skin inspection. If you have enough mobility, you may be able to do this with the help of a mirror. Manage incontinence to keep the skin dry. If you have urinary or bowel incontinence, take steps to prevent exposing the skin to moisture and bacteria. Your care may include frequently scheduled help with urinating, frequent diaper changes, protective lotions on healthy skin, or urinary catheters or rectal tubes. References: http://www.merckmanuals.com/professional/dermatologic-disorders/pressure-ulcers/pressure-ulcers Mayo clinic;Daniela KroshinskyMD, MPH, LaurenStrazzula M
- 6. Name________________________ Date______________ Bedsores 1. Individuals who are at risk of bedsores are which of the following? A.) Obese individuals who do not carry a healthy diet. B.) Individuals who have hearing loss and low daily activity. C.) Individuals with a medical condition that limits their ability to change positions. D.) All of the above 2. How many stages of severity do bedsores have? A.) Two B.) Five C.) Four D.) Three 3. In an unstageable bedsore you are still able to see how deep the wound is. A.) True B.) False 4. Under what stage(s) does the following observation fall into? Wound contains dark yellow crust and bone is easily visible. A.) Stage One & Stage two B.) Stage Two & Stage Four C.) Stage Three D.) Stage Four 5. Which of the following is a good way to prevent bedsores? A.) Bathing twice everyday B.) Having patient in only one position for the whole day. C.) Repositioning patient every two hours without creating stress to the body. D.) All of the above 6. Quitting Smoking can be a way to prevent bedsores. A.) True B.) False 7. You can also use cushions to relieve pressure against and between the knees and ankles. A.) True B.) False 8. One can develop bedsores in fingers, toes and, bottom of the feet. A.) True B.) False 9. Bedsores can also be called pressure ulcers. A.) True B.) False 10. A deep injury has which of the following characteristics A.) A blood-filled blister is present. B.) Skin seems to be broken C.) Both A & B D.) None of the above