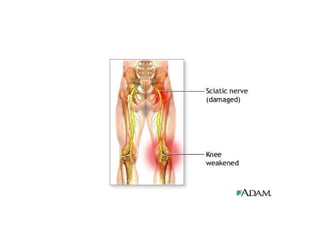
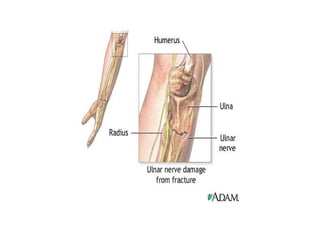
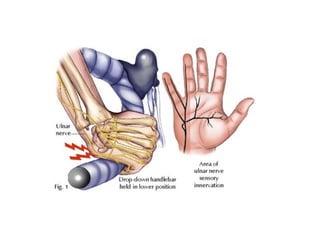
Peripheral neuropathy refers to damage or dysfunction of the peripheral nervous system, which can involve single nerves (mononeuropathy), multiple individual nerves (mononeuropathy multiplex), or nerve plexuses (plexopathy). Mononeuropathy affects a single nerve and can result from pressure or injury. Mononeuropathy multiplex involves multiple individual nerves in a random pattern, often due to vascular or connective tissue diseases. Plexopathy involves damage to nerve plexuses, commonly the brachial plexus, which can be caused by trauma, tumors, or other medical conditions.


![Diagnosis rests on the finding of motor, sensory or reflex changes confined to the territory of - single nerve - several individual nerves[random fashion] - plexus or part of the plexus of nerves](https://image.slidesharecdn.com/peripheralneuropathy-100121140010-phpapp01/85/Peripheral-Neuropathy-Types-3-320.jpg)


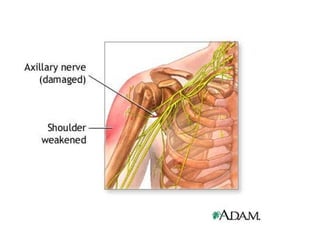


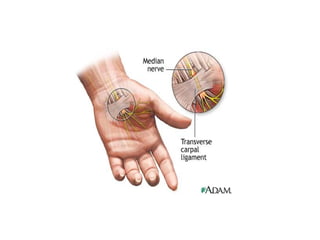
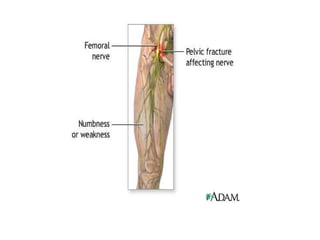
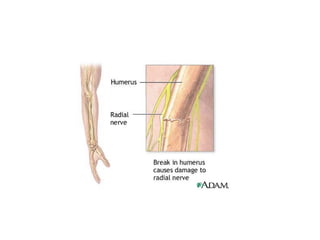







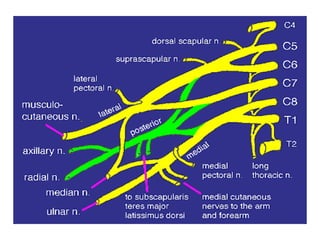

![Nontraumatic pathology of the brachial plexus primary tumour: schwannoma head and neck superior sulcus neoplasm: malignant neoplasm originating from the apical lung; it often invades the superior thoracic wall and may grow into the brachial plexus (Pancoasts neoplasm). Other neoplasms possibly invading the brachial plexus are local extensions or recurrences of breast cancer, soft tissue sarcomas and lymphoma. brachial neuritis: possibly related to an infection or an autoimmune condition[also Parsonage Turner syndrome] brachial plexopathy after irradiation. It is most often seen in patients treated for breast cancer. It is clinically and also radiologically difficult to differentiate from recurrent tumour. The presence of a mass lesion in or near the brachial plexus indicates tumour recurrence in most cases thoracic outlet syndrome](https://image.slidesharecdn.com/peripheralneuropathy-100121140010-phpapp01/85/Peripheral-Neuropathy-Types-25-320.jpg)