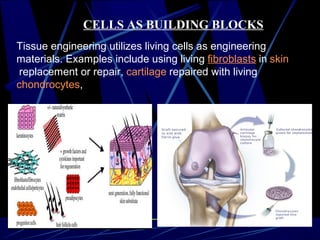
Tissue engineering combines cells, engineering methods, and biochemical factors to improve or replace biological functions, aiming to develop biological substitutes that restore tissue function. The process involves extracting cells, often from blood or solid tissues, and utilizing them alongside scaffolds made of various materials to create three-dimensional tissue structures. Applications include developing artificial organs and repairing tissues, such as skin and heart valves, offering solutions for medical challenges in transplantation and wound healing.

![INTRODUCTION :
Tissue engineering is the use of a combination of cells,
engineering and materials methods, and suitable
biochemical and physicochemical factors to improve or
replace biological functions.
The term has also been applied to efforts to perform
specific biochemical functions using cells within an
artificially-created support system (e.g. an
artificial pancreas, or a bio artificial liver).
A commonly applied definition of tissue engineering, as stated
by Langer and Vacanti is “An interdisciplinary field that
applies the principles of engineering and life sciences
toward the development of biological substitutes that
restore, maintain, or improve [Biological tissue] function or
a whole organ”](https://image.slidesharecdn.com/tissueengineering-151221003149/85/Tissue-engineering-2-320.jpg)