The document describes the development of the dental pulp and root formation. It discusses:
- How the dental pulp develops from mesenchymal cells that differentiate into odontoblasts and fibroblasts.
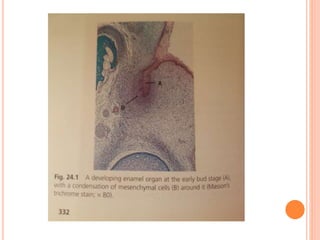
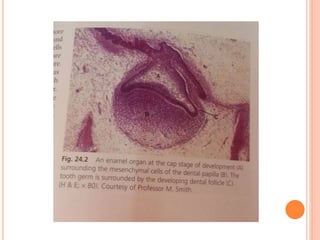
- How the dental papilla and follicle form during the bud and cap stages and their roles in tooth development.
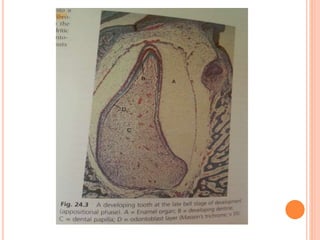
- How odontoblasts and cementoblasts differentiate during the bell stage to lay down dentin and cementum.
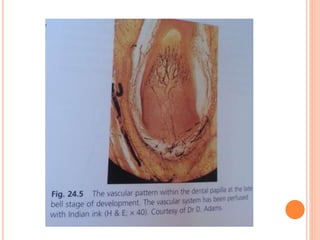
- The development of blood vessels and nerves that enter the dental pulp.
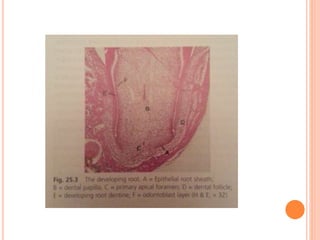
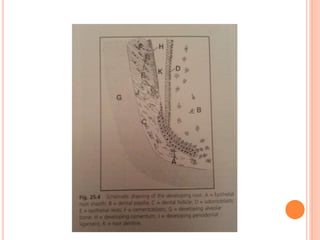
- How root formation is directed by the Hertwig's epithelial root sheath and how this determines root morphology.
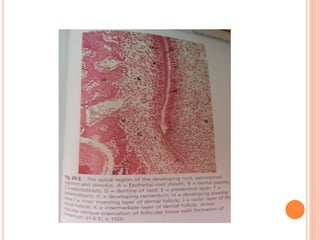
- The formation of acellular cementum on root surfaces by