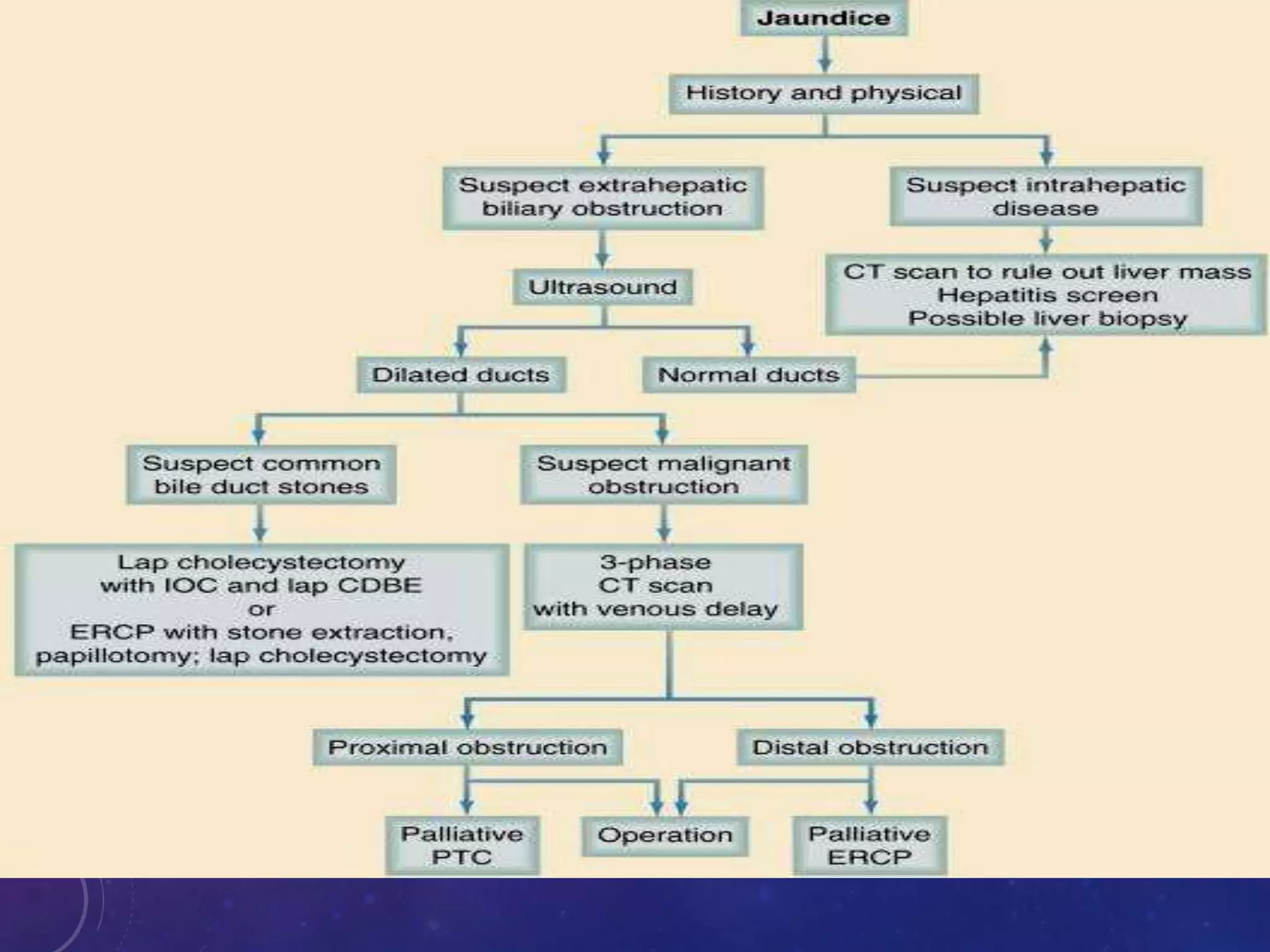
This document discusses obstructive jaundice, including its pathophysiology, workup, and management. It begins with definitions and descriptions of jaundice. Biochemical investigations that can help determine the level and cause of obstruction are outlined. Common etiologies of biliary obstruction include gallstones, strictures, tumors, and pancreatitis. Imaging modalities like ultrasound, MRCP, and EUS are described which can locate the obstruction and identify its cause. The document concludes with an algorithm for evaluating the specific clinical scenarios of ductal obstruction, cholangitis, or suspected cholelithiasis without cholangitis.





































![Ultrasonography
Ultrasound of the abdomen is an extremely useful and accurate method for identifying
gallstones and pathologic changes in the gallbladder consistent with acute cholecystitis.
Abdominal ultrasound, if performed by an experienced operator, should be part of the routine
evaluation of patients suspected of having gallstone disease, given the high specificity (>98%)
and sensitivity (>95%) of this test for the diagnosis of cholelithiasis[1] ( Table 54-1 ). In addition
to identifying gallstones, ultrasound can also detail signs of cholecystitis such as thickening of
the gallbladder wall, pericholecystic fluid, and impacted stone in the neck of the gallbladder. It
is often the initial screening test for patients with suspected extrahepatic biliary obstruction (
Fig. 54-7 ). Dilation of the extrahepatic (>10 mm) or intrahepatic (>4 mm) bile ducts suggests
biliary obstruction. Intraoperative ultrasound is now used frequently to further evaluate
intrahepatic lesions, assess resectability, and determine involvement of vascular structures](https://image.slidesharecdn.com/obstructivejaundice-201118193557/75/Obstructive-jaundice-40-2048.jpg)