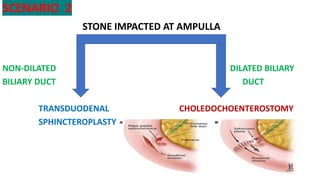
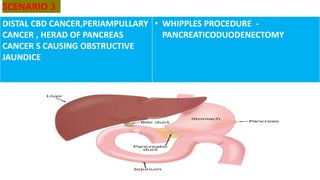
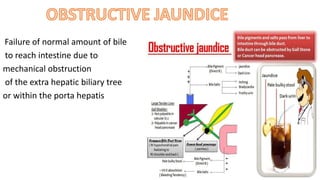
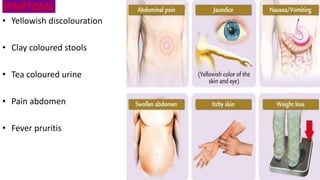
The document discusses the pathophysiology and management of obstructive jaundice, detailing the causes, physiological effects, and various types of biliary obstruction. It outlines the symptoms, diagnostics, and treatment options, including the importance of biochemical tests and imaging techniques like ultrasound and MRCP. Additionally, it emphasizes the critical need for timely intervention to manage complications and prevent recurrence.























![OTHER LAB INVESTINGATIONS
• Prothrombin time
• Serum albumin
• Stool for occult blood
• Presence of occult blood in the stools of a patient with
jaundice must raise the suspicion of malignancy
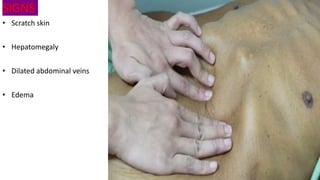
[THOMAS SIGN]](https://image.slidesharecdn.com/0bstructivejaundice-220603160702-e984bf82/85/0bstructive-jaundice-pptx-36-320.jpg)

















![IF CBD DIAMETER > 12 MM
1. CHOLEDOCHODUODENOSTOTMY
PROBLEM :- SUMP SYNDROME
2. HEPATOJEJUNOSTOMY
PROBLEM:- ERCP NOT POSSIBLE
ACCESS [HUDSON’S] LOOP CAN BE
DONE](https://image.slidesharecdn.com/0bstructivejaundice-220603160702-e984bf82/85/0bstructive-jaundice-pptx-72-320.jpg)