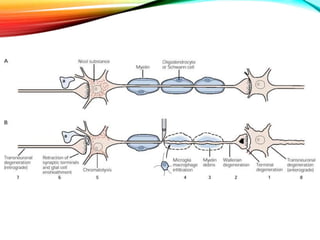
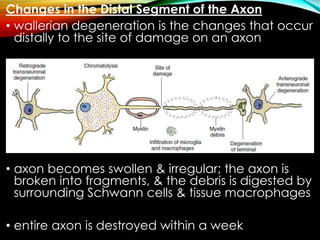
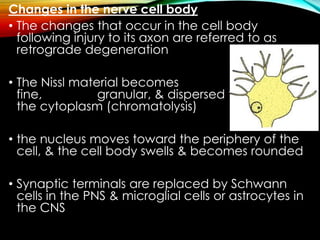
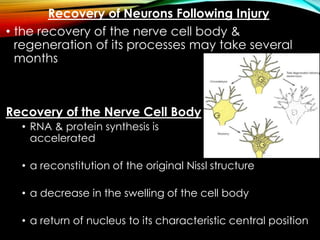
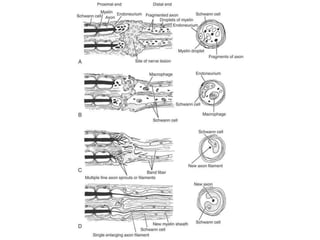
Neurons can be injured through cutting, crushing, pulling or pressure. There are different classifications of nerve injury depending on the extent of damage. Wallerian degeneration occurs after the axon is damaged, causing the distal segment to degenerate within a week. The proximal segment and cell body also exhibit retrograde degeneration changes. Recovery is possible if the nerve sheath remains intact to guide regeneration. In the peripheral nervous system, Schwann cells and macrophages clear debris to allow new axon growth. However, regeneration is more limited in the central nervous system due to inhibitory factors and scar tissue formation by astrocytes.