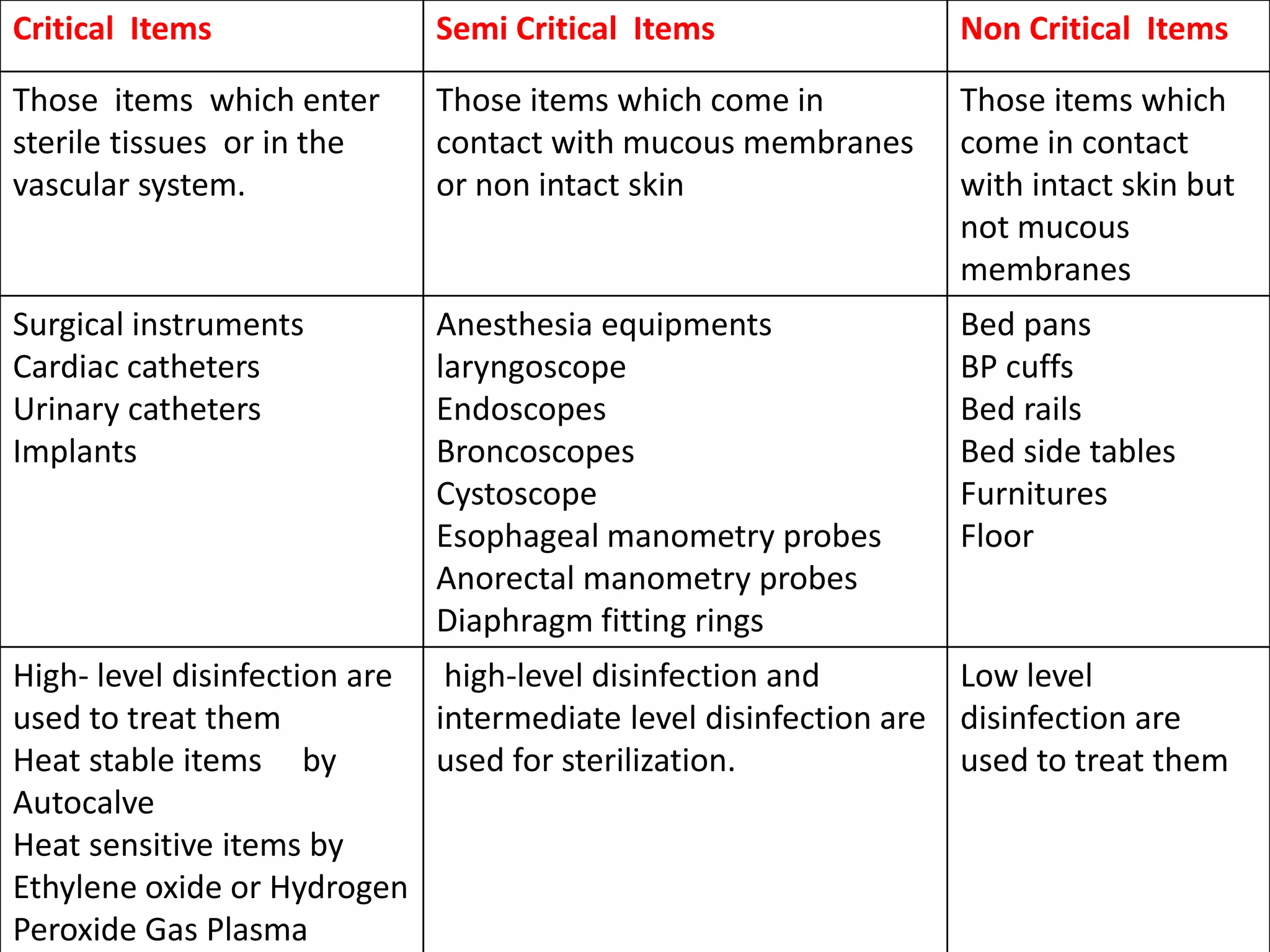
This document discusses various methods of chemical sterilization and disinfection. It defines key terms like sterilization, disinfection, antisepsis, and pasteurization. It describes different physical and chemical sterilizing agents such as heat, radiation, ethylene oxide, formaldehyde, and hydrogen peroxide. It classifies disinfectants based on their efficacy as high, intermediate, or low-level and outlines how items are classified based on Spaulding's system. Factors affecting disinfection effectiveness are also discussed.